Patriots Release Antonio Brown After Another Sexual Misconduct Allegation

The New England Patriots cut Antonio Brown after 11 days with the team. The wide receiver is accused of sexual assault and his future in the NFL is in doubt.
Lynne Sladky/AP
hide caption
toggle caption
Lynne Sladky/AP
The New England Patriots on Friday released wide receiver Antonio Brown, who had only been with the team for a short time, after a second woman accused him of sexual misconduct.
The defending Super Bowl champions announced the move in a statement emailed to reporters, minutes after Brown posted on Twitter: “Thank you for the opportunity @Patriots #GoWinIt.”
Statement from a #Patriots spokesperson: https://t.co/c98rNDX9QG pic.twitter.com/DAohupBLHo
— New England Patriots (@Patriots) September 20, 2019
The team’s statement attributed to a Patriots spokesperson said, in its entirety: “The New England Patriots are releasing Antonio Brown. We appreciate the hard work of many people over the past 11 days, but we feel that it is best to move in a different direction at this time.”
Two women have accused Brown of sexual misconduct. Former trainer Britney Taylor has filed a civil lawsuit against Brown — accusing him of rape and sexual assault on three occasions. The lawsuit became public last week, and Taylor has had meetings with the NFL.
Sports Illustrated reported this week that another woman said Brown sexually harassed her while she working at his home — she turned around to find him standing there naked except for a small towel covering his genitals.
SI reports the unidentified woman said she received “intimidating texts” after the magazine article detailed her allegations:
“The woman previously told SI that Brown had hired her two years ago to paint a mural of him in his home but “ghosted” her after she ignored his advance. On Wednesday night, the woman says, she received a group text message that appeared to come from the same phone number Brown provided to her in 2017. The text chain, with four other phone numbers on it, included photos of her and her children, with the person she believes is Brown encouraging others in the group to investigate the woman. The texter accused the artist of fabricating her account of the 2017 incident for cash. (In her letter to the league, the woman’s attorney repeated that the artist is not seeking remuneration from Brown in connection with the alleged incident.)”
Analysts say they do not expected Brown to join another NFL team this season.
It’s unfortunate things didn’t work out with the Patriots. But Antonio is healthy and is looking forward to his next opportunity in the NFL. He wants to play the game he loves and he hopes to play for another team soon.
— Drew Rosenhaus (@RosenhausSports) September 20, 2019
“It’s unfortunate things didn’t work out with the Patriots,” Brown ‘s agent, Drew Rosenhaus tweeted. “But Antonio is healthy and is looking forward to his next opportunity in the NFL. He wants to play the game he loves and he hopes to play for another team soon.”
Also this week, Nike cut ties with the receiver, saying in an email to The Associated Press on Friday, ” Antonio Brown is not a Nike athlete.”
Brown, a four-time All-Pro, began his career in Pittsburgh after being drafted in 2010 as a sixth-round pick by the Steelers. Over time his relationship with the Steelers soured and he was traded this year to the Oakland Raiders.
Oakland signed Brown to a contract that would have paid him up to $50 million over the next three seasons, but he never played a game for the team. After getting into disagreements with the coach and general manager, he was released.
A few hours later, the Patriots signed Brown to a one-year deal that would have guaranteed him $9 million and paid him up to $15 million this season.
New England Patriots Cut Antonio Brown
The New England Patriots have cut Antonio Brown after just 11 days with the team. The wide receiver is accused of sexual assault and his future in the NFL is now in doubt.
AUDIE CORNISH, HOST:
To the NFL now. The New England Patriots have released receiver Antonio Brown. Pressure had been building on the Patriots after allegations surfaced that Brown sexually assaulted a former trainer. From member station WGBH in Boston, Esteban Bustillos has more.
ESTEBAN BUSTILLOS, BYLINE: Eleven days – that’s how long the professional relationship between Antonio Brown and the New England Patriots lasted. And although the time was short, it was filled with strife from the beginning. Brown came in as something of a character whose antics forced the Oakland Raiders to release him. But the conversation became serious when Brown’s former trainer Britney Taylor accused him of sexual assault and rape in a lawsuit. When the allegations became public, Patriots head coach Bill Belichick remained stoic.
(SOUNDBITE OF ARCHIVED RECORDING)
UNIDENTIFIED REPORTER: Were you aware of the lawsuit when you signed Antonio Brown?
BILL BELICHICK: I’m not going to be expanding on the statements that have already been given.
UNIDENTIFIED REPORTER: Don’t you think the fans deserve to hear a little more from you on…
BELICHICK: When we know more, we’ll say more.
UNIDENTIFIED REPORTER: …Such a major development that, you know, could impact the team?
BELICHICK: I just said that.
BUSTILLOS: But the Patriots didn’t really say much more at all, and neither did Brown when he talked to reporters for the first time as a Patriot just yesterday. He answered a question about whether the NFL had told him anything about his playing status.
(SOUNDBITE OF ARCHIVED RECORDING)
ANTONIO BROWN: I appreciate that question. You know, I’m just here to just focus on ball and look forward to getting out there in the home stadium and being with the team.
BUSTILLOS: The pressure’s been on the NFL to do something. The league has battled image problems with multiple players over the past few years being accused of violence against women. During the past week, the NFL reportedly spoke to his accuser, Taylor, and Sports Illustrated reported that another unnamed woman had also accused him of sexual misconduct. Brown’s agent tweeted this afternoon that Brown wants to play the game he loves and hopes to play for another team soon, which would be his fourth in less than a year.
For NPR News, I’m Esteban Bustillos in Boston.
Copyright © 2019 NPR. All rights reserved. Visit our website terms of use and permissions pages at www.npr.org for further information.
NPR transcripts are created on a rush deadline by Verb8tm, Inc., an NPR contractor, and produced using a proprietary transcription process developed with NPR. This text may not be in its final form and may be updated or revised in the future. Accuracy and availability may vary. The authoritative record of NPR’s programming is the audio record.
A New Way Of Paying For Maternity Care Aims To Reduce C-Sections

Some insurers using this new payment model offer a single fee to one OB-GYN or medical practice, which then uses part of that money to cover the hospital care involved in labor and delivery. Other insurers opt to cut a separate contract with the hospital.
Adene Sanchez/Getty Images
hide caption
toggle caption
Adene Sanchez/Getty Images
The thrill of delivering newborns helped pull Dr. Jack Feltz into the field of obstetrics and gynecology.
More than 30 years later, he still enjoys treating patients, he says. But now Feltz is also working to change the way doctors are paid for maternity care.
Feltz’s New Jersey-based practice, Lifeline Medical Associates, recently partnered with the insurer UnitedHealthcare to test a new payment model. The insurer sets a budget with the practice to pay doctors one lump sum for prenatal services, delivery and 60 days of care afterward. If the costs come in below that amount, the medical practice gets to keep some of the savings. (Hospitals aren’t a part of this contract; the insurer pays them separately for their services.)
“We’ve always been taught to take care of patients as if they were our mothers and our daughters,” says Feltz, who also leads a coalition of obstetricians called the U.S. Women’s Health Alliance that advocates for high-quality, affordable care. “But now we have to take care of our patients as if they were our mothers and our daughters — and as if it was our money.”
This new program, announced in May, is a first step by the insurer to bundle physician payments for maternity care into a single flat fee that covers all care and procedures. A handful of insurers and state Medicaid programs are experimenting with similar models, sometimes incorporating hospitals and other health providers as well.
By moving from paying for maternity care in a piecemeal way to relying on bundled payments, insurers and doctors say they hope to cut costs and improve the quality of care for pregnant women.
But even fans of such a model acknowledge there are still significant obstacles to be worked out before this sort of flat-fee system could be implemented broadly.
The payment model is relatively new and still rare in maternity care; its structure can differ by insurer. Some insurers could pay a single amount to one doctor, who then uses part of it to cover hospital care. Other plans opt to cut a separate contract with the hospital. Insurers also vary in whether they make the lump sum payment before or after patients receive services. And the length of care, eligibility and services included in the bundle also vary.
In addition to, perhaps, reducing the overall cost of maternity care, the lump sums are seen by doctors and insurers as a possible way to improve health outcomes, including driving down the number of unnecessary cesarean sections in the United States.
About one-third of all deliveries in the U.S. occur via C-section, even though the World Health Organization estimates they are medically required in only 10% to 15% of births. The ratio of C-sections to live births varies dramatically among individual hospitals.
These surgeries can increase the risk of infections or other medical problems for the mother and baby. And they are more expensive than a vaginal delivery.
“The way we’ve been doing things is just not justifiable,” says David Lansky, a senior adviser at the Pacific Business Group on Health, a San Francisco-based coalition of private and public organizations that collectively purchase health care for 10 million Americans.
“The shift we’re talking about,” Lansky says, “is to say, ‘Someone is accountable for all the care that needs to be provided to support a family through this experience.’ “
Already, in traditional coverage, insurance payments for some women are delivered as bundled payments for some portions of their prenatal care, says Suzanne Delbanco, executive director of Catalyst for Payment Reform, a nonprofit organization that advises employers and other organizations that buy health coverage. However, she says, the new bundled payment models are different because insurers are adding quality measures that increase accountability to the bundle, as well as additional services such as labor and delivery.
Patients generally are not even aware their care is being handled under a bundled payment.
UnitedHealthcare, which announced its program in May, began testing the option with Feltz’s practice and another in Texas. The insurer says it hopes to expand to as many as 20 practices by the end of the year. Cigna and Humana are also piloting bundled maternity care programs. A few Medicaid programs, including those in Arkansas, Ohio and Tennessee, have experimented with it, too, in recent years.
Expanding the rarely used model to include maternity care could represent a major shift in health care finance. Births were the most common reason for hospitalizations among U.S. patients discharged in 2016, according to government data.
“Maternity care is kind of the sleeper of health care services,” says Dr. Neel Shah, an assistant professor of obstetrics, gynecology and reproductive biology at Harvard Medical School.
The change in payments is being made as the quality of maternity care in the United States comes under renewed scrutiny. An estimated 700 women in the U.S. die each year because of pregnancy-related complications, the federal Centers for Disease Control and Prevention reports. The rate of deaths in the U.S. is worse than in many other affluent countries, NPR and ProPublica reported in 2017.
C-sections also cost more than vaginal deliveries. In the Denver area, for instance, the average vaginal delivery costs $7,716 while the average C-section costs $14,274, according to 2019 data from the Health Care Cost Institute. On average, commercial and Medicaid insurers pay 50% more for C-sections than for vaginal deliveries, according to a 2013 report by Truven Health Analytics, a health industry consulting group.
Lansky’s group provided funding, data and oversight in 2014 for a project to test bundled payments for births in a variety of Southern California hospitals. According to their report, the rate of C-sections in first-time, low-risk pregnancies dropped by nearly 20% in less than one year among the first three participating hospitals.
However, some of the bundled-payment models have fallen short of aspirations. Tennessee saved money in 2017 after adopting the payment model for Medicaid beneficiaries. But the rate of C-sections remained unchanged, according to a report by the Medicaid and CHIP Payment and Access Commission, a nonpartisan advisory group for Congress.
In Ohio, where the Medicaid program covered complicated pregnancies as well as those that were low-risk, bundling payments into a lump sum for OB-GYNs cost the state more than expected, the advisory group found.
Bundling raises other concerns, too. Because some bundled-payment programs assign the total cost of care to a single physician, the financial burden falls on that physician. Dr. Lisa Hollier, the immediate past president of the American College of Obstetricians and Gynecologists, is concerned that these models may discourage team-based care.
If the physician providing prenatal care overlooks a problem that a different doctor must treat during delivery, for example, it wouldn’t be fair for the OB-GYN delivering the baby to bear the financial burden, Hollier says.
How payers define a low-risk pregnancy is also unclear, she says. If the target price for the suite of services in the model is not risk-adjusted for the cost of treating conditions like gestational diabetes, she says, doctors could be penalized for treating these patients.
Gestational diabetes occurs in up to 10% of pregnancies in the U.S. annually, according to the CDC, and patients with the condition need additional tests, checkups and insulin.
Julianne Pantaleone, national director of bundled payments and strategy at UnitedHealthcare, says that as the insurer works through its pilot program, it will cover the cost of physician care beyond the initial budget.
The lack of robust data systems built for handling bundled payments also poses a potential barrier for some medical practices, says Blair Barrett Dudley, a senior manager at the Pacific Business Group on Health.
Insurers and doctors need real-time data to ensure they are meeting the model’s quality measures, she says. However, these information banks are expensive to build, and many of the existing ones aren’t designed to handle this payment structure.
Feltz agrees that getting such data will be imperative to a successful bundled payment program. Without the information, he says, “it’s like launching a ship and not knowing where it’s going to go.”
Kaiser Health News is a nonprofit, editorially independent program of the Kaiser Family Foundation. KHN is not affiliated with Kaiser Permanente.
How An ‘International Price Index’ Might Help Reduce Drug Prices

A pharmacist collects packets of boxed medication from the shelves of a pharmacy in London, U.K. A proposal announced by House Speaker Nancy Pelosi Thursday would allow the government to directly negotiate the price of 250 U.S. drugs, using what the drugs cost in Australia, Canada, France, Germany, Japan, and the United Kingdom as a baseline.
Bloomberg via Getty Images
hide caption
toggle caption
Bloomberg via Getty Images
In gridlocked Washington, both Democrats and Republicans have signaled there’s potential for a deal when it comes to lowering prescription drug prices. Now, there’s an idea both Congressional Democrats and the White House seem to like: They want to base U.S. prices on something called an international price index.
“The basic idea is to peg what the United States pays for a particular drug to the price paid in some set of other countries,” says Rachel Sachs, an associate professor of law at Washington University in St. Louis who specializes in drug pricing policy. “There are many different ways to identify other countries, and there are many different ways in which that international reference price could be used to negotiate for a price here.”
House Speaker Nancy Pelosi unveiled her sweeping plan to reduce drug prices Thursday, which included an international price index. There are lots of differences between that plan and the one the White House floated last fall, but the basics — and the appeal of the concept — are the same.
“It stops drug companies from ripping off Americans while charging other countries less for the drug,” Pelosi said in a press conference announcing the House plan, which would use drug prices in Australia, Canada, France, Germany, Japan, and the United Kingdom to create a baseline in negotiating prices.
She’s speaking President Trump’s language. Here’s what he told reporters in July: “Why should other nations like Canada — why should other nations pay much less than us? They’ve taken advantage of the system for a long time, pharma.”
Earlier this summer, the Department of Health and Human Services sent its own IPI proposal to the White House for review, though the details haven’t been made public. The idea of establishing an IPI is the only element of the administration’s plan to lower prescription drug prices still on the table — other ideas, like displaying list prices in TV ads and ending secret rebates for middlemen have been withdrawn or blocked in the courts.
A glimpse of what the HHS proposal might look like can be found in the outline of a Medicare model HHS released last fall. Like the House Democrats’ plan, the HHS model uses an index of countries to generate an average price. But, unlike the House plan, it would not let the secretary of HHS use that average to negotiate directly with drugmakers.
The HHS outline is also more limited in the drugs that would be eligible for this sort of price-setting. Medications eligible would be only a subset of drugs used by Medicare patients — mostly injections given in doctor’s offices — whereas the House plan would extend to a wider group of 250 brand-name drugs.
Another difference? “The House Democrats’ proposal envisions a non-compliance fee that would financially penalize drug companies who won’t bargain in a good-faith way with the administration,” Sachs says. “There’s no such enforcement mechanism in the administration’s IPI proposal.”
Both plans would use the average price internationally for each drug as a benchmark in negotiations, so that Americans don’t pay more than about 20% above what people in other countries pay. That’s still more than what people pay outside the U.S., but less than they pay now.
“The prices the U.S. is currently paying today can be two or three times as much, [though it] varies a lot by product,” says Stacie Dusetzina, a professor of health policy at Vanderbilt University School of Medicine. “This would be a major price reduction.”
One example of a drug priced much higher in the U.S. than elsewhere is Humira, a brand name rheumatoid arthritis drug. In 2015, it cost $2,669 a month in the U.S., while the list price in the U.K. was about half that — $1,362. The same drug cost only $552 in South Africa, according to the International Federation of Health Plans.
“I believe that the price of Humira now in the U.S. is about $63,000 a year,” says Ben Wakana, executive director of the advocacy group Patients for Affordable Drugs. “And [the drugmaker] AbbVie has raised the price eleven times between 2014 and 2018.” Wakana has a personal connection to Humira — his brother. In the U.S., there’s no generic competition that might push the price down, he notes.
“For patients like my brother and like the thousands of people who take Humira every year, that price is simply too high,” Wakana says. “We need competition. And if we can’t get competition, then we need to be able to negotiate with AbbVie for a fair price — like they are offering in other countries.”
So, would establishing an international price index actually work to lower drug prices?
The Trump administration projects that, in five years, using its IPI would save Medicare patients $3.4 billion. Policy analysts have argued that the amount patients would save is actually a bit murkier because many Medicare patients who use these drugs also have supplemental insurance. In addition, because so many countries — 24 in Europe alone — use this kind of indexing, there’s the risk of a circular effect, with everybody looking to their neighbor instead of basing the cost of the drug on concrete measures of the medicine’s clinical value or the costs of developing and producing it.
In Canada, the government already uses international drug list prices in negotiations, and has recently made moves to go even further.
“The comparison of our list prices in Canada to the list prices in other countries has proven to be not very effective at controlling the real price of medicines in this country,” says Steve Morgan, a professor of health policy at the University of British Columbia. One reason for that, he says, is that list prices don’t reflect real prices after drugmaker rebates. So now, he says, “Canada is trying to implement further price regulations that would make sure that the final negotiated prices are reasonable.”
In the United States, many Republican lawmakers and conservative groups have opposed the idea of an international index — arguing that it runs against free market principles.
Unsurprisingly, drugmakers also object. “Speaker Pelosi’s radical plan would end the current market-based system that has made the United States the global leader in developing innovative, lifesaving treatments and cures,” Stephen Ubl, CEO of lobbying group PhRMA, says in a written statement. “We do not need to blow up the current system to make medicines more affordable.”
But Pelosi and her allies seem to be betting there is political will to go against drugmakers this time. Despite the huge sums spent on lobbying, the pharmaceutical industry is now the most unpopular industry in the country, according to a recent Gallup poll. And with a presidential election coming up, Americans polled say lowering drug prices is a top priority.
This could mean there’s room for the House and the White House to work together, especially on an idea like an international price index that they’ve both proposed.
“We do hope to have White House buy-in,” Pelosi said Thursday. “That seems to be the route to getting any votes in the United States Senate, and certainly we want as strong a bipartisan vote as we can in the House and the Senate. So we would hope that they would support this.”
The Real Bachelor Party Hangover: A $12,460 ER Bill

Cameron and Katlynn Fischer celebrated their April wedding in Colorado. But the day before, Cameron was in such bad shape from a bachelor party hangover that he headed to an emergency room to be rehydrated. That’s when their financial headaches began.
Courtesy of Cameron Fischer
hide caption
toggle caption
Courtesy of Cameron Fischer
Two days before his wedding this past April, Cameron Fischer had one heck of a bachelor party, hitting a few bars in the Old Town section of Fort Collins, Colo., with his friends into the wee hours. The next morning, the 30-year-old IT professional from nearby Loveland woke up with a killer hangover.
“I couldn’t keep anything down,” Fischer says. “I just felt miserable.”
He was in such bad shape that, with their wedding day fast approaching, Fischer’s fiancée urged him to leave their rehearsal dinner in Denver and head to an emergency room to be rehydrated.
That resulted in an even bigger headache: a medical bill that was initially $12,460, all told. That was more than twice the cost of their wedding.
Fischer had run into a sobering fact about America’s health care system. With few constraints on how emergency rooms set prices, hospital systems have jacked up rates and coded patient visits as being more complex than they would have previously, which increases the payments they receive from insurance plans. The result: ER services have some of the fastest-growing prices in the health care system.
Many health economists think free-standing ER facilities, like the one Fischer visited — which are banned in many states but thriving in Colorado — are particularly culpable. While such ERs maintain that they can’t survive on rates paid by Medicare and Medicaid, data suggest they are profit-seeking engines built primarily in high-income ZIP codes.
“It’s because they’ve figured out that they can get away with it,” says Vivian Ho, an economist with the Baker Institute for Public Policy at Rice University in Houston.
Fischer might have avoided the big bill had he sought treatment earlier in the day. But by 7 p.m. on a Saturday, urgent care facilities were closed. He checked Google Maps for the closest emergency room and — clutching a trash can — headed to HealthONE North Suburban Medical Center, a free-standing ER in the Denver suburb of Thornton.
The ER appeared to be devoid of patients, with just a doctor and a couple of nurses on duty. Fischer told them what had happened and that he didn’t do drugs and doesn’t often drink.
“I knew exactly why I was there,” he says. “It wasn’t that I had some unknown reason for my symptoms.”
A nurse started an IV and gave Fischer two bags of saline and a dose of Zofran, an anti-nausea medication. She drew blood; Fischer says he wasn’t told what tests would be run on the blood sample. He was out of the ER within 45 minutes, feeling much better.
Facility fees as the price of entry
A few weeks after Fischer’s April wedding, he received the medical bill.
It included a $7,644 “facility fee.” That’s an expense that hospital systems charge to cover their overhead costs of keeping an ER open 24 hours a day and ready for any emergency.
Facility fees are set on a scale from 1 to 5, depending on how severe the patient’s condition appears during the initial triage. The ER rated Fischer’s visit as a 4, one of moderately high complexity, in terms of care needs.
“There are no limitations on the facility fees that they can charge,” says Adam Fox, director of strategic engagement for the Colorado Consumer Health Initiative, a nonprofit consumer advocacy group. “The facility fee for over $7,000 is simply obscene,” Fox says.
The Health Care Cost Institute, an independent, nonprofit health research firm, recently analyzed millions of insurance bills to get a better sense of the facility fees that ERs are charging. It found the charges nearly doubled from 2009 to 2016, outpacing overall health spending four times over. In Colorado, the average facility fee charged for a Level 4 visit grew from $1,064 to $2,336.
Insurance plans generally don’t pay the full charge but pay a negotiated rate for in-network hospitals. The Center for Improving Value in Health Care, which maintains a database of insurance payments in Colorado, found that insurance plans paid an average of $1,754 for a Level 4 facility fee in 2018.
Still, those prices pale in comparison with the fee charged to Fischer. “That seems like an outlier on the high end,” says John Hargraves, a senior researcher at the Health Care Cost Institute who led the ER study. “That’s more than triple what it was in 2016.”
Other studies have found that ERs are coding visits at the higher 4 and 5 complexity levels at higher rates than in past years. It’s not clear whether that reflects a deliberate attempt by hospital systems to increase payments or a shift in the type of patients who visit emergency rooms. It’s possible the growth in urgent care centers is siphoning off less complex cases.
Treatment costs for a hangover
The ER’s initial bill included $500 for a complete blood count — a test that the online price comparison tool Healthcare Bluebook says could be had for less than $20 in a doctor’s office. It charged more than $1,300 for a complete metabolic panel, a routine test that generally costs about $31.
The two liters of saline, which the ER billed at $700, are available at Walmart for $10.99 a liter.
And spa-like hydration services in Denver market IV fluids for hangover relief, consisting of the same combination of saline and nausea meds that Fischer received in the ER, for just $168.
The ER bill also included $970 for a drug test, something Fischer says he never consented to undergo. Medicare typically pays health care providers about $114 for the same test.
“When you look at the bill, obviously the prices are astronomical,” Fischer says. “But it was also the work that was performed without my authorization that was pretty frustrating.”
HealthONE officials say the prices at its ERs are higher than at urgent care clinics or other outpatient settings because the ERs are staffed by board-certified emergency physicians and cannot turn away any patients, regardless of their ability to pay. So paying patients who show up in their ERs subsidize those who show up and can’t pay.
“The move toward higher-deductible insurance plans has put a strain on many of our patients, but we understand their choice to pay a lower monthly premium, and we also understand their frustration with the larger out-of-pocket expenses they may experience as a result,” HealthONE North Suburban Medical Center spokeswoman Betty Rueda-Aguilar said in a written statement to Kaiser Health News. She adds that Fischer presented with symptoms of alcohol poisoning and had to be treated accordingly. The company declined our requests for an interview.
Emergency rooms tend to lose money on critically ill patients, as well as on Medicare, Medicaid and uninsured patients, says Dr. Jesse Pines, national director of clinical innovation for US Acute Care Solutions, which helps staff more than 200 hospitals and ERs. These facilities try to make up the difference with less sick, privately insured patients, like Fischer, Pines says.
“To make the economics of an emergency department work, those patients have to subsidize the system to make the difference balance out,” he adds.
But as more privately insured patients have high-deductible plans, he says, it has been harder and harder for hospitals to collect on their bills from patients who don’t pay.
Free-standing ERs
Free-standing ERs, such as North Suburban, may have found a way to skew their patient mix toward those who can pay. A report from the Colorado Health Institute finds that free-standing ERs tend to locate in high-income neighborhoods. Residents there are more likely to have higher-paying commercial insurance, rather than Medicare or Medicaid, and are likelier than other patients to be able to pay for out-of-pocket costs their insurance doesn’t cover.
Colorado has more than 50 free-standing ERs, according to the report, trailing only Texas and Ohio. The facilities are licensed as “community clinics and emergency centers,” a designation originally developed to help rural and underserved communities in Colorado that could not otherwise afford inpatient hospitals. But the report identifies only eight free-standing emergency departments in rural Colorado — all in affluent ski resort towns.
For Fischer, the negotiated rates under his health plan knocked the $12,460 bill down to $4,694. The plan paid $2,102. That left Fischer with a bill of $2,593, an amount he says he cannot afford to pay.
“That’s quite the expensive bachelor party,” Fischer says.
Kaiser Health News is a nonprofit, editorially independent program of the Kaiser Family Foundation and is not affiliated with Kaiser Permanente.
The Chess Grandmaster’s Diet
Chess grandmasters spend hours sitting over game boards. And yet, high-level players lose 10 to 12 pounds on average over a 10-day tournament. ESPN’s Aishwarya Kumar dug into that statistic.
Delgres Combines Guadeloupean Heritage With New Orleans Creole And Blues

Delgres performs live in Paris for World Cafe: Sense of Place
Kimberly Junod/WXPN
hide caption
toggle caption
Kimberly Junod/WXPN
- “Mo Jodi”
- “Respecté Nou”
- “Mr. President”
- “Vivre Sur La Route”
- “Lanme La”
Pascal Danaë was born just outside of Paris and the first time he went to the French overseas region Guadeloupe, he was given the “Letter of Freedom” that belonged to his ancestor, Louise Danaë. She was freed from slavery in 1841 at 27 years old. At the time, she had four children, one of whom was Pascal’s grand grandfather.
The history of slavery and French colonialism plays a big role in the music Danaë makes now with his three-piece blues band Delgres. He named the act after Louis Delgrès, the freedom fighter who resisted the reintroduction of slavery in Guadeloupe by Napoleon in 1802 and died for the cause.
We met up with Delgres at La Boule Noire in Paris to hear live performances of songs from the band’s latest album, Mo Jodi, and to talk about some of the features that make the band so unique. Danaë sang in Creole and his bandmate, Rafgee, played the parts that would normally be handled by a bass guitar on the sousaphone, an instrument typically found in New Orleans brass bands. Danaë also shed light on the historic and musical connection between Africa, the French West Indies and Louisiana, as well as the healing power of the blues.
For Arizona Baseball Fans, A Stadium Bratwurst Meant To ‘Blow Their Mind’

Stephen Tilder, the executive chef at Chase Field in Phoenix, holds the SI Cover Dog, a collaboration with a Sports Illustrated reporter.
Bridget Dowd/KJZZ
hide caption
toggle caption
Bridget Dowd/KJZZ
For Arizona Diamondbacks fans who like to stick to the basics at home games, peanuts, popcorn, and Cracker Jack remain obvious options. But for those whose game-day taste borders on outrageous, Stephen Tilder, executive chef at Chase Field in Phoenix, has some options.
You can get 18-inch bratwursts adorned with everything from tater tots to fried eggs.
Chase Field is among the stadiums nationwide that now tout menus brimming with outrageous edible novelties.
“We are always trying to create, basically, restaurant quality food in a ballpark,” Tilder says. “When people come in we want to blow their mind.”
In March, Tilder — in collaboration with a Sports Illustrated reporter — created three new gigantic dogs for Diamondbacks’ fans. One of those, the SI Cover Dog (named after the magazine) is topped with jalapeño-apple coleslaw, barbecue aioli, fried mac and cheese, house cured beer pickles and green onion. It’s all served between an onion bun.
This year we collaborated with @SINow and @TheWilderThings to bring 3 new jaw-dropping #DbacksEats to @ChaseField.
First, meet the SI Cover Dog, an 18-inch bratwurst with jalapeño-apple coleslaw, fried mac and cheese, barbecue aioli, house-cured beer pickles and green onion. pic.twitter.com/EkVmHgwsAd
— Arizona Diamondbacks (@Dbacks) March 18, 2019
There’s also Reuben Some Dirt On It Dog, which features fried pickles and a secret sauce and All-Day Breakfast Dog — with hash browns, country gravy and fried eggs.
Tilder said the Tot Dog, which has tater tots and chili, is one of his top sellers.
“It’s a little spicy from the chili, you get the crunch from the tater tots, you get the coolness of the sour cream — so there’s so many layers that go really well with each other,” Tilder says.
The final ingredient of each of Chase Field’s specialty dogs? A $30 price tag.
This baseball season, NPR’s Morning Edition found that Chase Field is far from the only stadium reinventing the sport’s culinary wheel. From the Diamondbacks’ Blooper Burger to the D.C. Nationals’ Bulgogi Hoagie, nationwide, crazy concoctions are tempting fans to abandon the traditional ballgame snacks of the past.
It’s Not Just Insulin: Diabetes Patients Struggle To Get Crucial Supplies

Ric Peralta and his wife Lisa are both able to check Ric’s blood sugar levels at any time, using the Dexcom app and an arm patch that measures the levels and sends the information wirelessly.
Allison Zaucha for NPR
hide caption
toggle caption
Allison Zaucha for NPR
In the first three months after getting his Dexcom continuous glucose monitor, Ric Peralta managed to reduce his average blood sugar level by three percentage points.
“It took me from not-very-well-managed blood sugar to something that was incredibly well managed,” says Peralta, a 46-year-old optician in Whittier, Calif., who was diagnosed with Type 1 diabetes in 2008.
Peralta was so enthused that he became a “Dexcom Warrior,” a sort of grassroots spokesman for the product. It became hard to imagine life without his new monitor, a device that lets him keep track the trends in his blood sugar 24 hours a day on his smart phone. And yet, he’s spent weeks at a time without the device over the past year because of problems with insurance restrictions. Physician groups and patients consider those rules overly burdensome, but insurance groups defend them as necessary.
Diabetes activists and legislators have started to focus attention on the surging price of insulin, leading to legislative pushes, lawsuits and congressional hearings. But insulin isn’t the only thing people with Type 1 diabetes are struggling to get. Managing the condition requires other essential, often life-saving medical supplies. And patients frequently face hurdles in getting access to those supplies — hurdles put in place by insurance companies.
A life changing device
Peralta learned about the Dexcom continuous glucose monitor from the mother of one of his patients. He visited the company’s website and, within two weeks, the device had been shipped to his front door.
“I still didn’t 100 percent appreciate exactly how it was going to change my life,” Peralta says. “It was amazing.”

In their home in Whittier, Calif., Lisa Peralta pats Ric’s Dexcom sensor to make sure it’s staying on his arm. Before he got the device, Ric had to check his blood glucose via multiple finger pricks and plastic test strips every few hours.
Allison Zaucha for NPR
hide caption
toggle caption
Allison Zaucha for NPR
Typically, people with Type 1 diabetes check their blood sugar by drawing a drop of blood from their finger and placing it on a disposable test strip that’s read by a blood glucose meter. Doctors suggest checking blood sugar this way between four and 10 times per day. These readings are crucial for helping people with diabetes manage their blood sugar — keeping it from getting too low, which can lead to sudden seizures and loss of consciousness, as well as from getting too high, which can cause vision loss, nerve damage and can even, over time, lead to amputations.
Instead, Peralta’s continuous glucose monitor gave accurate blood sugar readings every five minutes. That’s 288 readings per day, or about 278 more readings than even the most conscientious patients get the old-fashioned way.
“When I had to do the old-fashioned finger prick test, I was only doing that right before I ate, so I could see how much [insulin] I was supposed to take,” Peralta says. (People with Type 1 diabetes have to take multiple daily shots of insulin to keep their blood sugar within normal range because their bodies stop producing the naturally occurring hormone.)
“I didn’t realize that I had rather severe [blood sugar] peaks and valleys in between my meal times,” Peralta says.
Tighter control of blood sugar can reduce the risk of heart disease, kidney failure and nerve damage. For Peralta, it also offered peace of mind.
The monitor sounds an alarm when his blood sugar is getting dangerously low; Peralta says his coworkers have started bringing him sugary snacks when they hear the alarm, to help him raise his blood sugar back up to normal. When he takes his family on road trips — a favorite activity — he no longer has to worry about the possibility of passing out while he’s driving.
“It even syncs with my car so I can just say, ‘Siri, what’s my blood sugar?’ And it will come over the car stereo system,” Peralta says. “I’m safe for my family.”
Prior-authorization requirements
When common chronic conditions such as diabetes are well controlled, it prevents worsening disease and saves money for the health system and the patient.
But Peralta says his efforts to use this new tool consistently to manage his diabetes have been stymied by insurance problems that began about a year ago.
The newest Dexcom continuous glucose monitor has three parts: a sensor that measures glucose levels, a transmitter that sends out the sensor’s readings wirelessly, and a receiver that displays those readings on a screen.
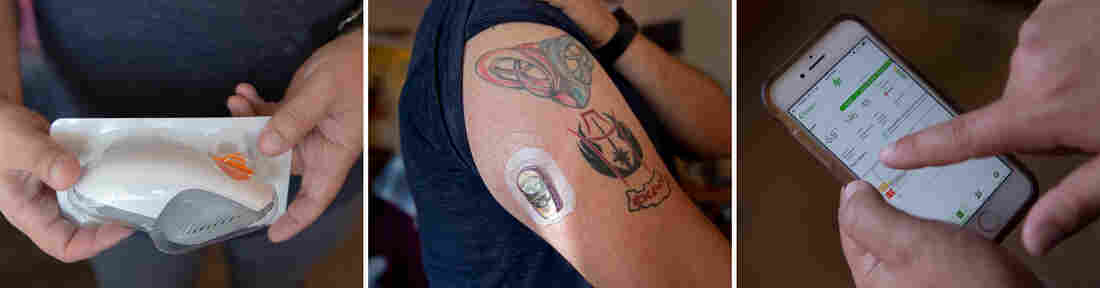
Testing blood sugar now involves three pieces of equipment, Ric Peralta says: (Left) Peralta holds the applicator that contains the Dexcom G6 sensor and transmitter he’s about to affix to his arm. (Center) the Dexcom sensor and transmitter in place. (Right) Peralta checks the Dexcom app on his smart phone to see his glucose levels before he eats.
Allison Zaucha for NPR
hide caption
toggle caption
Allison Zaucha for NPR
For each of these parts, Peralta needs something called a “prior authorization” from his insurer — a requirement from his insurance company that necessitates his physician seeking approval from the insurance company before prescribing the device.
The Dexcom sensors last about 10 days each and Peralta’s insurance allows him to buy a three-month supply at a time. But he also has to get prior authorization for each supply, meaning every three months his doctor needs to reconfirm with his insurance company that the sensors are medically necessary. Same goes for the device’s transmitters — which last about six months each.
“I have to jump through hoops and they have to jump through hoops to get information from my insurance to get authorization,” Peralta says in frustration, adding, “for the last year, basically every time there’s been something that’s gone wrong.”
“Prior authorizations are in place to protect patients, to improve safety and to try to make sure that the care they receive is as safe as possible and also as affordable as possible,” says Kate Berry of the trade group America’s Health Insurance Programs.
But to Ric Peralta, the requirement is a burden.
The most recent snafu happened in March. Peralta ordered a new supply of sensors directly from Dexcom but says the company submitted a request for approval of a new transmitter, as well. And because his insurance approves the sensors and transmitters on different authorization timelines, the whole claim was denied. Peralta estimates he spent four hours on the phone with Dexcom and his insurer over the next month and a half to sort it all out. During that time he had to revert to finger stick tests.
“It’s maddening,” Peralta says. “If I do not have my proper management of this disease I’m going to die from it. And they’re making it as difficult as possible.”

Peralta says he’s become a “Dexcom Warrior” — a sort of grassroots spokesman for patients with diabetes who routinely get stuck in limbo waiting for their insurers to approve the medical supplies their doctors have prescribed.
Allison Zaucha for NPR
hide caption
toggle caption
Allison Zaucha for NPR
A burden on doctors, too
Prior authorizations have become a major concern of physicians across the U.S. health care system, as evidenced by a December 2018 survey by the American Medical Association.
Of the 1,000 physicians surveyed, 91 percent said prior authorizations “have a negative impact on patient clinical outcomes;” 75 percent said the requirements “can at least sometimes lead to patients abandoning a recommended course of treatment;” and 28 percent said the prior authorization process had “led to serious or life-threatening events” for their patients.
“In my practice we have five individual physicians, and we hired five full-time employees whose primary duty is obtaining prior authorization and dealing with insurance companies,” says Dr. Bruce Scott, an otolaryngologist from Kentucky and Vice Speaker of the AMA House of Delegates.
“Prior authorization is a burden on providers and diverts valuable resources,” Scott says. “That’s a problem.”
The AMA has even created a website that catalogs stories of patients and providers who say they’ve struggled to gain access to important medical products and procedures because of problems getting prior authorizations from insurers — everything from pain medication for a cancer patient to X-rays in the ER. Scott says the AMA doesn’t expect insurers to completely do away with requirements for prior authorization, “but we believe that it should be focused and that it should be better planned.”
The American Association of Clinical Endocrinologists — an organization of the physicians whose specialty is often associated with diabetes treatment — goes even further.
“We feel that physicians that are specialists in endocrine disease should not be required to fill out prior authorizations for endocrine treatments,” says Dr. Scott Isaacs, an endocrinologist from Atlanta and member of the board of directors of AACE.
“It’s a huge burden for the patients trying to get this sorted out. Sometimes it’s red tape; sometimes it’s a true denial,” Isaacs says. “It’s a huge burden for the doctors as well, and the doctors resent it.”
Berry, of the insurance group AHIP, acknowledges that there’s room for improvement in the prior authorization process. In fact, in January 2018, the AMA and AHIP signed a consensus statement identifying five areas for improvement. It was cosigned by the American Hospital Association, the American Pharmacists Association, the Blue Cross Blue Shield Association and the Medical Group Management Association.
Who bears the greatest burden?
For Ric Peralta, the ultimate burden of getting all these prescriptions filled falls on him and patients like him.
After his latest mix-up with the sensors in March, he discovered the battery in his transmitter had died.
Peralta made another frustrated call to Dexcom, and recently got a complimentary transmitter to get him back on the system while his formal order goes through the approval process.
“I’m quite nervous about what’s going to happen again in two months when I am needing to call in orders again,” Peralta says.
“Am I going to have to go through this whole thing over again?”
This story is part of NPR’s reporting partnership with Kaiser Health News. Bram Sable-Smith is a freelance reporter based in Madison, Wisc., who often covers health care. Reach him on Twitter: @besables.
American Becomes 1st Person To Swim English Channel 4 Times Without Stopping

Sarah Thomas, a 37-year-old cancer survivor, swims across the 21-mile English Channel. She said she was stung on the face by a jellyfish during her epic swim, in which she crisscrossed the channel four times, a journey that ended up being more than 130 miles because of the tides.
Jon Washer/AP
hide caption
toggle caption
Jon Washer/AP
Sarah Thomas, an American ultramarathon swimmer, has just completed a swim that no other human on the planet has ever accomplished.
The 37-year-old from Colorado plunged into waters off the shore of Dover, England, in the wee hours of Sunday morning. Her goal: swim the entire length of the English Channel.
Then do it again.
And again.
And again.
Thomas completed the final leg of her swim at around 6:30 a.m. local time Tuesday in just over 54 hours— the first person to cross the channel four times without stopping.
According to the Channel Swimming Association, the English Channel is about 21 miles wide.
In an interview with the BBC, Thomas said she was in disbelief that she had done it and was surprised by a group of well-wishers who were waiting for her on shore when she got out of the water.
She’s done it ????
After treatment for breast cancer last year, Sarah Thomas has become the first person to swim across the Channel four times non-stop ????????????????
Congratulations! #channelswimmer #sarahthomas pic.twitter.com/5Kfi4GzOnT— BBC Breakfast (@BBCBreakfast) September 17, 2019
“I’m really just pretty numb,” she said. “There was a lot of people on the beach to meet me and wish me well and it was really nice of them, but I feel just mostly stunned.”
She also told the BBC that she planned to sleep the remainder of the day, adding: “I’m pretty tired right now.”
Just a year ago, Thomas was completing treatment for breast cancer. In a Facebook post on Saturday, a day before starting her epic exploit, Thomas dedicated her swim to “all the Survivors out there.”
“This is for those of us who have prayed for our lives, who have wondered with despair about what comes next, and have battled through pain and fear to overcome,” she wrote. “This is for those of you just starting your cancer journey and those of you who are thriving with cancer kicked firmly into the past, and for everyone in between.”
The Guardian points out that Thomas is not the first person to swim across the English Channel multiple times — four swimmers have crisscrossed it three times without stopping.
As the crow flies, Thomas’ swim should have been approximately 80 miles long. But the journey ended up being more than 130 miles because of the tides, the Guardian reports.
The newspaper also says Thomas drank a carbohydrate-laden shake every half hour to keep her body replenished. Her mother, Becky Baxter, said the shake was “tied to a rope” and tossed to Thomas from a nearby boat where a crew was keeping a watchful eye on her.
As the crow flies, Thomas’ record-setting swim four times across the English Channel should have been approximately 80 miles long. It ended up being more than 50 miles longer because of the pull of tides.
track.rs/ssthomas3; ESRI-National Geographic
hide caption
toggle caption
track.rs/ssthomas3; ESRI-National Geographic
“She drinks a third of that bottle in 10-15 seconds, and then she takes off again,” Baxter said, according to the Guardian. “She is a freak of nature. She really had to dig deep to finish this. She could have quit many, many times. There were several obstacles, but she never quits.”
Before Thomas’ final leg, a member of her team posted on Facebook about water conditions in the channel at the time: “Dark, windy, and choppy conditions tonight for the final leg of the English Channel 4 way crossing.”
And there were other obstacles. Thomas told the BBC that the salt water hurt her throat, mouth and tongue.
The currents on the last leg pushed her “all over,” she told the broadcaster, adding: “I got stung in the face by a jellyfish. [The water] wasn’t as cold as I thought it might be, but it was still chilly.”
The official Twitter account for the Channel Swimming & Piloting Federation, the governing body for English Channel swimming, called Thomas “an absolute legend.”
Congratulations to Sarah Thomas for successfully completing a 4-way historic crossing of the English Channel. An absolute legend! We’ll have official confirmation of times shortly (I assume everyone needs a good sleep after that!)
— CS&PF (@csandpf) September 17, 2019

