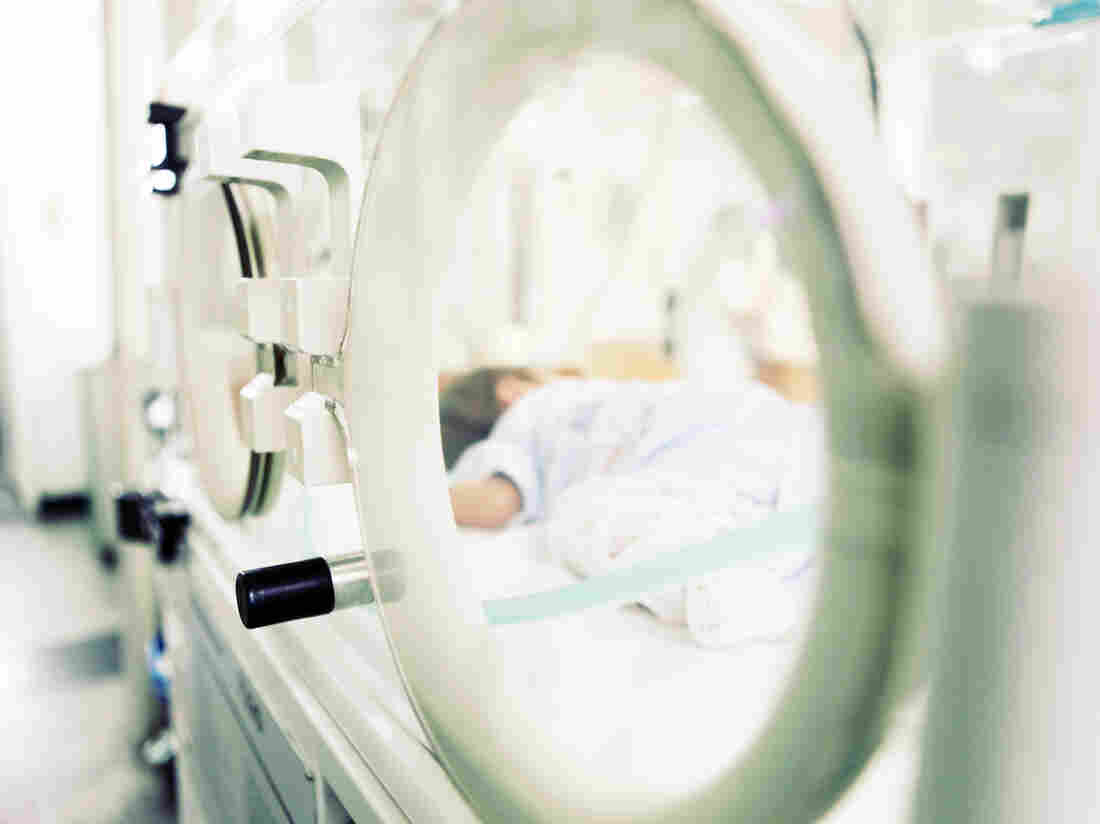
Firefighters are often exposed to carcinogens in the course of their work. Laws in many states say if they get cancer, it should be presumed to be linked to their work.
Arisha Singh/EyeEm/Getty Images
hide caption
toggle caption
Arisha Singh/EyeEm/Getty Images
Doctors told Steve Dillman the throat cancer he was diagnosed with in 2008 came from smoking. He knew it didn’t.
“I thought it had to be job-related because I’ve never smoked a day in my life. I don’t chew. I don’t drink excessively … and that’s the three main criterias,” he says.
But Dillman did spend 38 years as an Indianapolis firefighter — and that included running into burning buildings.
Dillman, who’s now retired, recalls one fire on Aug. 1, 1985. That day, his fire station responded to a call at the American Fletcher National Bank warehouse in downtown Indianapolis.
Firefighters noticed something strange and painful after they put out the flames. Everywhere they sweated – under their arms, around their groins – their skin peeled, like it had been sunburned.
Dillman later learned the warehouse was filled with boxes treated with a flame-retardant chemical that sent toxic gases into the air – including formaldehyde, a known carcinogen.
Dillman was diagnosed with prostate cancer 16 years later, and throat cancer seven years after that.
“It’s just an evil thing that we have to deal with,” 74-year-old Dillman says.
Research from National Institute for Occupational Safety and Health (NIOSH) published in 2013 shows that firefighters are diagnosed with and die from cancer at higher rates than the general population. It confirmed earlier research finding elevated risk for the profession for certain cancers.
The correlation between firefighters’ on-the-job exposure to carcinogens and their subsequent illnesses is concerning enough to policy makers that a growing number of states have passed laws — 42 states and Washington, D.C. — designed to help firefighters who develop cancer, according to the non-profit Firefighter Cancer Support Network.
Generally, these laws say that firefighters diagnosed with cancer while on the job or within a certain time after retirement are presumed to have become ill because of their work. And that should make it easier for them to get workers’ compensation, disability benefits or death benefits for their families.
But firefighters say those protections often fall short.
Leaders of organizations that work with firefighters say, despite these laws, firefighters are often denied workers’ compensation claims after a cancer diagnosis. Firefighters have challenged denials in a number of states, including California, Pennsylvania, Texas, and Washington.
“Presumptive laws aren’t the golden ticket that people think they are,” says Jim Brinkley, director of occupational health and safety for the International Association of Fire Fighters, a Washington, D.C.-based lobbying organization. “Our detractors are the ones who will say it’s not connected to the job because they don’t want to pay the benefits.”
It’s difficult to estimate how many firefighters have been denied benefits, says Keith Tyson, vice president for education and research for the Firefighter Cancer Support Network. He’s a prostate cancer survivor who spent 34 years on the job in Florida, where there is no presumptive law.
Tyson doesn’t know of any organization that tracks such workers compensation claims nationwide. And other than his organization’s analysis of state laws, there isn’t a comprehensive listing of the states offering protection.
“That’s the problem. Nobody is consistent on any of this,” Tyson says. “It’s unfortunate that there couldn’t be a one-standard-fits-all [law]. That would make it so much easier.”
Exposed to contaminants
Heart disease was the leading cause of firefighter deaths until the mid-1990s, when “the burden of cancer significantly surpassed heart disease,” according to a paper on firefighters and cancer published last year in the American Journal of Industrial Medicine.
That study surveyed 2,818 Indiana firefighters who died between 1985 and 2013, and found that they had a 20 percent greater likelihood of dying due to cancer than non-firefighters.
This builds on the findings of the 2013 NIOSH study, which included nearly 30,000 firefighters from Chicago, Philadelphia and San Francisco. It found that firefighters are exposed to contaminants that are known or suspected to cause cancer — everything from asbestos in old buildings to the diesel exhaust from fire trucks — and they are more likely to develop respiratory, digestive and urinary system cancers than the general public.
For one rare cancer, mesothelioma, which is linked to asbestos exposure, the rate is two times greater in firefighters than the general U.S. population.
In July 2018, President Trump signed the Firefighter Cancer Registry Act directing the Centers for Disease Control and Prevention to collect national data about the issue. Fire stations can send information on cancer rates among their staff to the National Institute for Occupational Safety and Health.
NIOSH will look for trends in how cancer affects male and female firefighters, firefighters of different races and those in urban and rural areas.
Brinkley hopes this data will make it “very clear to the legislators and those controlling the purse strings that we need better protection for firefighters.”
Presumptive laws in action
State presumptive laws vary in many ways. Some cover only certain cancers. Some states limit how long after retirement a cancer diagnosis is covered. And in some states, a diagnosis alone isn’t enough to trigger protections such as disability benefits.
Of the states with presumptive cancer laws, the Firefighter Cancer Support Network found one that extends coverage up to three months after retirement. Six states, including Indiana, provide coverage up to five years. One state allows seven years, one state allows 600 weeks and three cover up to 20 years.
This reflects a misunderstanding of science, says Dr. Jefferey Burgess, an environmental health researcher at the University of Arizona College of Public Health. He says cancer can develop “anywhere from less than five years to over 30 years” after exposure to carcinogens.
Burgess, who has researched firefighters and cancer for more than 25 years, says the evidence shows firefighters are regularly exposed to carcinogens in the field, and that firefighters are diagnosed with cancer more than the general public.
“From my perspective, I believe we’ve clearly demonstrated that firefighting is associated with cancer,” he says.
Future research is needed, Burgess says, to determine more specific links between those exposures and a firefighter’s cancer diagnosis. At this point, it’s not possible to prove that a single exposure to a carcinogen caused a specific cancer. In fact, there isn’t definitive research that shows even a career of exposure causes a specific cancer diagnosis.
Instead of demanding documentation of possible exposures from fires long ago, Burgess says fire departments should understand that firefighters’ health is affected by their work.
“To tell you whether it was an individual fire or was a lifetime exposure, I don’t know we have that particular information right now,” Burgess says. “Every fire tends to have these chemicals, and therefore it should just, from my mind, be a question of whether you’re a firefighter and you’ve gone to fires rather than documenting that a specific fire was a problem.”
Even with presumptive laws in place, municipalities across the country often fight firefighter’s cancer-related workers’ comp claims. And firefighters are pushing back.
In Texas, the Houston Chronicle found that in the past six years, nine in 10 Texas firefighters with cancer have had their workers compensation claims denied.
In Philadelphia, the city denied a firefighter’s claim in 2012, leading to a lengthy process of appeals. Ultimately, the Pennsylvania Supreme Court ruled in 2018 in favor of the firefighter, arguing that firefighters diagnosed with cancer must only show that their cancer could be caused by exposure to a known carcinogen. It’s up to their employers to prove it was not work-related.
Brinkley says the International Association of Fire Fighters has tried to develop more information about these claims nationwide. It has asked municipalities for data on workplace injury claims related to cancer — and how often they’re denied. The requests have been refused.
The National Council on Compensation Insurance, which gathers and analyzes data related to states’ workers compensation systems, released a report in 2016 on the impact of presumptive laws.
The report noted that firefighters are typically employed by state and local governments, which are often self-insured. Self-insured entities aren’t required to report claims to the council. Still, the NCCI stated in the report that it “expects that the enactment of such presumptions will result in increases in workers compensation costs.”
‘A moment of weakness’
In Indiana, as in some other states with presumptive laws, when a firefighter makes a cancer-related claim, the city wants to know the specific fire that led to the cancer diagnosis.
But firefighters traditionally haven’t kept records of chemical exposures, Brinkley says.
“To ask a member who is fighting a horrific disease that could end their life to then find that one call that they were exposed to one chemical that causes that one cancer is just a way of holding on to the money and not paying the claim,” he says. “That’s not taking care of your firefighter, who risks their life every day.”
Indianapolis Fire Department division chief for health and safety Kevan Crawley advocates for firefighters’ benefits. He says he spends months arguing with city officials and Broadspire, the company that manages workplace injury claims.
Asked about the issue, a Broadspire spokeswoman said the company won’t comment on how it manages its clients’ claims.
Brett Wineinger, risk manager for Indianapolis, oversees the city’s insurance policies. He says that few of the claims have dealt with cancer.
“We’re going to monitor any claim that’s filed with us against [Indiana’s presumptive law],” Wineinger says. “If it’s something that is linked to a fire instance that’s clearly something they’ve gotten through an exposure, obviously we’re going to take that as a workplace injury because that should be the first line of defense.”
Crawley says he understands that the city is trying to protect its budget. And he doesn’t believe that the insurers who deny claims are “bad people.”
But he says they don’t understand what it’s like to sit down with a newly-diagnosed firefighter and explain that the city won’t help with cancer-related costs.
“Guys you’ve looked up to in your career, and you don’t ever expect to see them in a moment of weakness,” Crawley says.
Growing a culture of safety
Firefighters at the Indianapolis Fire Department say they can’t rely on the state’s presumptive law for protection, so they’re focusing on what is in their control: preventing exposure to carcinogens.
Firefighters can wear a protective mask that filters out gases and particles. Otherwise, they breathe in a lot of smoke.
In the old days, firefighters were called “smoke-eaters,” recalls retired firefighter Dillman, and they wore their charred, soot-covered gear as a badge of honor.
At fires, Dillman didn’t wear hisprotective mask.No one did. If you did you were a “sissy,” he says.
“It was just the way the job was,” Dillman recalls.
Procedures during fires have changed since Dillman retired in 2005. It’s now standard practice for firefighters to wearthese masks at a fire.
Dillman now travels to fire departments around Indiana to urge firefighters to use masks and practice other preventive cancer measures.
To make his point, Dillman brings a couple of props.
“The last thing I tell them, ‘You can either wear your [protective] air mask … ‘” he says, holding one up for emphasis.
Then he shows the oxygen mask he needed to breathe when his cancer was at its worst.
And he says, “Or you can wear this mask. And trust me, you don’t want to wear this mask.”
This story was produced by Side Effects Public Media, a news collaborative covering public health.
Let’s block ads! (Why?)