Has Your Doctor Talked To You About Climate Change?

Dr. Mary Rice walks with Michael Howard at a Beth Israel Deaconess HealthCare clinic in Chealsea, Mass, as they test his oxygen levels with the addition of oxygen from a portable tank. He has COPD, a progressive lung disease that can be exacerbated by heat and humidity.
Jesse Costa/WBUR
hide caption
toggle caption
Jesse Costa/WBUR
When Michael Howard arrives for a checkup with his lung specialist, he’s worried about how his body will cope with the heat and humidity of a Boston summer.
“I lived in Florida for 14 years and I moved back because the humidity was just too much,” Howard tells pulmonologist Mary Rice, as he settles into an exam room chair at a Beth Israel Deaconess HealthCare clinic.
Howard, who is 57, has COPD, a progressive lung disease that can be exacerbated by heat and humidity. Even inside a comfortable, climate-controlled room, his oxygen levels worry Rice. Howard reluctantly agrees to try using portable oxygen. He’s resigned to wearing the clear plastic tubes looped over his ears and inserted in his nostrils. He assures Rice he has an air conditioner and will stay inside on really hot days. The doctor and patient agree that Howard should take his walks in the evenings to be sure that he gets enough exercise without overheating.
Then Howard turns to Rice with a question she didn’t encounter in medical school: “Can I ask you: Last summer, why was it so hot?”
Rice, who studies air pollution, is ready.

Rice, who studies the health effects of air pollution, talks with Howard about his increased breathing problems and their possible link to the heat waves, increased pollen and longer allergy seasons associated with climate change.
Jesse Costa/WBUR
hide caption
toggle caption
Jesse Costa/WBUR
“The overall trend of the hotter summers that we’re seeing [is] due to climate change,” Rice says, “and with the overall upward trend, we’ve got the consequences of climate change.”
For Rice, connecting those consequences — heat waves, more pollen, longer allergy seasons — to her patients’ health is becoming routine. She is among a very small but growing number of doctors and nurses who discuss those connections with patients.
In June, the American Medical Association, American Academy of Pediatrics and American Heart Association were among 70 medical and public health groups that issued a call to action asking the U.S. government, business and leaders to recognize climate change as a health emergency.
“The health, safety and wellbeing of millions of people in the U.S. have already been harmed by human-caused climate change, and health risks in the future are dire without urgent action to fight climate change,” the coalition statement said.
The World Health Organization calls climate change “the greatest health challenge of the 21st century,” and a dozen U.S. medical societies urge action to limit global warming.
Some societies provide patient handouts that explain related health risks. But none have guidelines that explain how providers should talk to patients about climate change. There is no concrete list of “dos” — as in wear a seat belt, use sunscreen, and get exercise — or “don’ts” — as in don’t smoke, don’t drink too much and don’t text while driving.
Climate change is different, says Rice, because an individual patient can’t prevent it. So Rice focuses on steps her patients can take to cope with the consequences of heatwaves, more potent pollen and a longer allergy season.
That’s Mary Heafy’s main complaint. The 64-year-old has asthma that is worse during the allergy season. During her appointment with Rice, Heafy wants to discuss whether she’s on the right medications. But she also wants to know why her eyes and nose are running and her chest is tight for longer periods every year.
“It feels like once [the allergy season] starts in the springtime, it doesn’t end until there’s a killing frost,” Heafy tells Rice, with some exasperation.

Rice checks Mary Heafy’s breathing during a checkup for her asthma at the Beth Israel Deaconess clinic. Climate change does seem to be extending the Boston region’s ragweed season, Rice tells Heafy.
Jesse Costa/WBUR
hide caption
toggle caption
Jesse Costa/WBUR
“Yes,” Rice nods, “because of global warming, the plants are flowering earlier in the spring. After hot summers, the trees are releasing more pollen the following season. And the ragweed — it’s extending longer into the fall.”
So Heafy may need stronger medicines and more air filters, her doctor says, and may spend more days wearing a mask — although the effort of breathing through a mask is hard on her lungs as well.
As she and the doctor finalize a prescription plan, Heafy observes that “physicians talk about things like smoking, but I don’t know that every physician talks about the environmental impact.”
There are many reasons few do. Besides the lack of guidelines, doctors say they don’t have time during a 15- to 20-minute visit to approach something as complicated as climate change.
And the topic can be controversial: While a recent Pew Research Center poll found that 59% of Americans think climate change affects their local community “a great deal or some,” only 31% say it affects them personally, and views vary widely by political party.
We contacted energy-industry trade groups to ask what role — if any — medical providers should have in the climate change conversation, but neither the American Petroleum Institute nor the American Fuel and Petroleum Manufacturers returned calls or email requests for comment.
Some doctors worry about challenging a patient’s beliefs on the sometimes-fraught topic, according to Dr. Nitin Damle, the past president of the American College of Physicians.
“It’s a difficult conversation to have,” says Damle, who practices internal medicine in Wakefield, R. I. . “Many people still think it’s something they’re not going to be affected by, but it’s really not true.”
Damle says he “takes the temperature” of patients, with some general questions about the environment or the weather, before deciding if he’ll suggest that climate change is affecting their health.
Gaurab Basu, a primary care physician at Cambridge Health Alliance, says he’s ready if patients want to talk about climate change, but he doesn’t bring it up. Basu says he must make sure patients feel safe in the exam room. Raising a controversial political issue might erode that feeling. When patients do ask about climate change, it can be “a difficult conversation,” he says.
“I have to be honest about the science and the threat that is there, and it is quite alarming,” Basu says.
So alarming that Basu says he often refers patients to counseling. Psychiatrists concerned about the effects of climate change on mental health say there are no standards of care in their profession yet. They suggest a response must be tailored for each patient, but some common responses are emerging.
“We Are Hungry for Information”
One environmental group isn’t waiting for doctors and nurses to figure how to talk to patients about climate change.
“We’re trying to create a demand for these conversations to get started,” says Molly Rauch, the public health policy director with Moms Clean Air Force, a project of the Environmental Defense Fund.
Rauch urges the group’s more than one million members to ask doctors and nurses for guidance. For example: When should parents keep children indoors because the outdoor air is too dirty?
“This isn’t too scary for us to hear about,” Rauch says. “We are hungry for information about this, we want to know.”
But Rauch says it doesn’t seem like climate change is breaking into the medical community as a health issue. One study found classes about environmental health or global warming at only 20 out of 140 U.S. medical schools.
A few nursing schools are adding climate-related courses to their training, to prepare students for conversations with patients.
“Nurses need to catch up quickly,” says Patrice Nicholas, director of the Center for Climate Change, Climate Justice and Health at the MGH Institute of Health Professions in Boston.
Nicholas attributes the delay, in part, to politics. “Climate change really needs to be reframed as a public health issue,” Nicholas says.
The few doctors and nurses who have started discussing climate change with their patients say they’ve not had much pushback, but that may be because bringing climate change into the exam room is still very new.
This story is part of NPR’s reporting partnership with WBUR and Kaiser Health News, an editorially independent news service of the Kaiser Family Foundation.
Overhauling Kidney Care
This week, President Trump signed an executive order aimed at improving the care of kidney patients. Nephrologist Amaka Eneanya talks with Scott Simon about some of the new initiatives.
SCOTT SIMON, HOST:
Americans with kidney disease got some encouraging news when President Trump signed an executive order aimed at improving their care.
(SOUNDBITE OF ARCHIVED RECORDING)
PRESIDENT DONALD TRUMP: Those who suffer from kidney disease experience a significant toll on their daily lives.
SIMON: The administration wants to improve detection and diagnosis, increase the number of kidney transplants and move patients away from commercial dialysis centers by encouraging more in-home dialysis. Medicare now spends about $114 billion on kidney care every year, about a third of that on people who need regular dialysis or a transplant.
Dr. Amaka Eneanya is a nephrologist with Penn Medicine at the University of Pennsylvania. She treats patients with chronic kidney disease. Thanks very much for being with us.
AMAKA ENEANYA: Thank you for having me on, Scott.
SIMON: The scope of kidney illness in this country is enormous, isn’t it?
ENEANYA: That’s correct. So approximately 37 million adults have chronic kidney disease in United States. And the majority of those adults are unaware of their diagnosis, upwards of 90%.
SIMON: One of the proposals, and certainly one that a lot of people noticed, is encouraging patients to have dialysis at home…
ENEANYA: That’s correct.
SIMON: …Which I gather is common in some countries around the world, but not the United States. Why not so far?
ENEANYA: So there’s a few reasons for that. So one, the training for clinicians who actually do provide care for patients with kidney disease is not very robust for home dialysis. Also, the payment incentives, as they are now, really favor doing dialysis in in-center dialysis facilities. Also, education for patients is still evolving for them to learn about home dialysis.
SIMON: How do you do home dialysis?
ENEANYA: Basically, what your kidneys do is to, on a regular, you know, 24/7 basis, clean the body of fluid and waste. And that’s basically what your urine is. And so when you’re doing home dialysis, you have machines that are actually doing this for you. So you’re connecting to this machine, and it’s removing fluid and waste from the body, just as your kidneys would do.
SIMON: And this works overseas?
ENEANYA: This works incredibly well. Countries – Guatemala, Mexico, Hong Kong have the majority of their patients using some type of home dialysis.
SIMON: I noticed some medical sources this week, in response to the president’s plan, said, look; what we have is working now. Why endanger that?
ENEANYA: The question is who is it working for? If it’s working for the patients and we have a resounding response from them that that’s what the case is, then by all means, we should reconsider and look at things very closely. But that’s not what research has shown, and that’s not what my experience has been, and many others, in terms of caring for these patients. It’s quite a burden to do things the way that they have been doing, which is most of the patients going to dialysis or receiving their dialysis in a facility.
SIMON: The administration wants to double the number of kidneys available for transplant. How do you do that?
ENEANYA: Part of what he was describing was incentivizing donors – paying them for lost wages and child care that they may have to use after doing a surgery. I think a lot of the time, there’s a focus on the recipient because they have this chronic disease, and they’re getting a fresh, new kidney, and great for them. But I recently had an experience where I spoke to a altruistic donor, so a person who just decided to donate a kidney out of the goodness of their heart. And she really remarked, you know, tearfully, how difficult the post-operative period was and how she really wasn’t prepared for how long she would be…
SIMON: Yeah.
ENEANYA: …Out of work and, you know, how difficult that was. And so I think actually educating donors and providing these incentives will really make a difference.
SIMON: Do you think the executive order signed this week is going to – has the hope of improving life for kidney patients in a couple of years?
ENEANYA: Absolutely. This was a phenomenal kind of monumental time for the field of nephrology and for patients with kidney disease. If the goal is to have 80% of patients with end-stage kidney disease to be on a home dialysis modality or to receive a transplant, that’s a really big change. And so we know that quality of life will be – will improve. Patients will have kind of more choices in terms of what is best for them. It’s really an exciting time.
SIMON: Dr. Amaka Eneanya, a nephrologist with Penn Medicine, University of Pennsylvania. Thanks so much for being with us.
ENEANYA: Thank you so much.
(SOUNDBITE OF MUSIC)
Copyright © 2019 NPR. All rights reserved. Visit our website terms of use and permissions pages at www.npr.org for further information.
NPR transcripts are created on a rush deadline by Verb8tm, Inc., an NPR contractor, and produced using a proprietary transcription process developed with NPR. This text may not be in its final form and may be updated or revised in the future. Accuracy and availability may vary. The authoritative record of NPR’s programming is the audio record.
Keith Hernandez On Baseball, ‘Seinfeld’ And Being His Own ‘Worst Enemy’
The former first baseman played on championship teams with the Cardinals and Mets, and made a memorable appearance on Seinfeld. His memoir is I’m Keith Hernandez. Originally broadcast June 4, 2018.
DAVE DAVIES, HOST:
This is FRESH AIR. I’m Dave Davies, in for Terry Gross.
You might know our guest Keith Hernandez as a big-league ballplayer or as a memorable guest on two episodes of “Seinfeld.” And if you’re a New York Mets fan, you’ll know him as a color analyst for the team’s TV broadcasts. In 17 seasons in the big leagues, Hernandez was known for hitting wicked blind drives and for dazzling defensive plays at first base. He won Gold Glove Awards, a batting title, a Most Valuable Player Award and two World Series rings.
As a broadcaster these days, he’s built quite a social media following, at times posting videos of his aging Bengal cat Hadji. Hernandez has a memoir, now out in paperback, which focuses less on his glory days in the game than on times he struggled, especially when he was young and trying to adjust to big-league pressure, big-league pitchers and the stresses of playing every day. The book is called “I’m Keith Hernandez.” I spoke with him last year, when his memoir was published.
(SOUNDBITE OF ARCHIVED NPR BROADCAST)
DAVIES: Well, Keith Hernandez, welcome to FRESH AIR. You know, I recently read in the new book about Tiger Woods that his dad put him in a highchair in his garage when he was, like, an infant and had him watch his dad taking golf swings. And then he had him swinging a golf club when he was a toddler. And I read in your book that your dad had a kind of a training rig setup in your garage for your brother and you. Tell us about that and what it meant to you.
KEITH HERNANDEZ: Well, our garage in Pacifica, Calif., didn’t have Sheetrock on the ceiling, and it was just all the two-by-fours and the cross bars and the beams. So – and we did have a rafter going across. It was a loft, kind of like – almost like an open attic. And Dad set up, on the middle of the garage – and we were – my brother and I were both left-hand hitters – so he set it up more on the right side of the garage if you were looking at the door so we could take a full swing – a rope tied around one of the two-by-fours and extended the rope down and then put two white cotton athletic socks with a tennis ball in it and then tied it to the rope.
And the rope, at full extension, would be a knee-high strike. We started doing this when we were, like, 6, 7 years old. I mean, it was my brother and I. And then if you wanted to get it up higher to a belt-high strike, you just throw the – you just threw the rope over the two-by-four. If you wanted a high pitch, keep throwing it over, maybe two, three, four times, and it was a high pitch. And the ball would swing like a pendulum. And it would – the arc of the ball going up after we stroked it would hit the underside of the loft, which was, like, one-by-fours. So I marked them – you know, single, out, double, fly ball – and I would swing for hours and play games with that.
And my dad, in the beginning, would watch us swing, make sure we were swinging properly. And eventually, he felt that we had it down pretty good. And you know, he didn’t have to watch. I remember him saying when I was older that he’d come home from work – he was a fireman in San Francisco for 30 years – and he’d hear that pounding of the tennis ball against the rafters. And you know, it would give him a headache sometimes. And – but it made him laugh because I was there taking – you know, I was probably 500 to a thousand swings a day. I just absolutely loved it.
DAVIES: Right. And you know, you and your brother weren’t just slapping at it because your dad knew something about the game. He would look at your mechanics. Tell us a bit about him. How did he know so much about baseball?
HERNANDEZ: Well, my dad was a minor league player, and he was originally drafted by the Brooklyn Dodgers before World War II. He got hit in the head his first year, and his eyes – no helmets those days – eyes progressively got worse. And he eventually played for Cleveland and Oklahoma City and then was traded to the Cardinals and played under Johnny Keane in Houston, where he met my mother. And they got married after the season. He was a very good hitter and a very fine fielding first baseman.
And his career was shortened. And so he put it all – after the war – he served four years in the service – in the Navy at Pearl Harbor in a ship repair unit, played on the U.S. Navy team, which played the U.S. Army team and Army Air Corps. Stan Musial, in ’45, played with my father. Ted Williams was playing on the teams – the Marine team. So there was all these ex – all these major leaguers playing in this league, were entertaining the troops, basically.
DAVIES: Yeah. So it’s clear you had talent. But it was all of that practice from somebody who knew what he was doing that no doubt honed your skills. You were drafted by the St. Louis Cardinals organization and were a prized prospect. A lot was expected of you. And it took years for you, as you write in the book, to really get your stride as a hitter. And partly that was, you know, adjusting mechanics and learning pitches. But a lot of it was emotional. How did your head get in the way?
HERNANDEZ: Well, I always – I describe my fragility – my emotional fragility. I mean, you’re – you come out of high school. You’re a star in your little area you grew up. I grew up with the baby boomers, and there was lots of kids to play ball with. And all of a sudden, my first spring training, there’s 700 kids in the camp, and there’s only eight teams. And I know I’m going to make the team. I got a signing bonus of 30,000, which was unheard of for a 42nd round pick.
But it just – the big adjustment is you play two games a week in summer league in – back in those days, in high school. And now you’re playing – I believe it was 128 games scheduled in the minor leagues, something like that. And you’re playing every day. And you’re not going to hit .500 like you did in high school. I hit .256 in A-ball. I hit .260 in Double-A the next year. And you know, it was tough. It was depressing.
And then you go in slumps, and it’s your first experience with slumps. And it’s all a learning process. And you’re a hotheaded, 18-year-old kid, and you don’t know how to handle it. You throw helmets. You throw bats. You kick dirt. And you know – and you’ve got coaches trying to tell you to calm down and you’ve got to learn to play this game on an even keel. And it’s all part of the process. That’s what the minor leagues are about. But it – you know, it takes a long time, and everybody’s different. It took me a lot longer.
DAVIES: I think you write at one point that one of your coaches thought you needed to be away from your dad a little bit. I mean, he was such…
HERNANDEZ: Yes.
DAVIES: …An important influence in your life. Was he – I don’t know, a challenge, a burden? Was it difficult with him, too?
HERNANDEZ: Well, when the Cardinals were scouting me, Dad negotiated my contract. They got a sense of the strength and the power of my father. Bob Kennedy – there was an A-ball team in Modesto in the California state league. There was three A-ball teams – Cedar Rapids, St. Pete in the Florida State League – and California state league. Bob Kennedy kept me out of the California state league, which he felt I wasn’t ready to play in because that was the top A-ball league. And he put me in the middling Florida State League, which was a tough league.
And he told me years later he wanted to kind of cut the apron strings from my father. So there you go – Bob Kennedy being a real influence on my career.
DAVIES: What – do you think you needed to cut the strings from your father a bit?
HERNANDEZ: Yes, no question. It was the right thing to do because Dad – my brother played in the California state league, and Dad came to all of his games just whenever he could. And that would have drove me crazy. Gary had a different relationship with my father than I did with him. And yes, it was the right thing to do to get me away from him and get me to stand up on my own two feet.
DAVIES: Was he hypercritical? You felt like you just couldn’t please him?
HERNANDEZ: Well, he coached us all through Little League, and he was just wonderful. And the parents and the kids were all benefited from his instruction. And he was really terrific with the kids. But once I got into high school, he was so petrified that a coach would ruin me. And it was – in other words, he lost control. And that’s when things started to get a little dicey between me and him.
He would always watch whenever he can. He was a fireman. He worked 24 hours, off 48. He had two days off, so he would be at every practice in high school, watching. And it was like, you know, “The Central Scrutinizer,” you know, from Frank Zappa’s “Joe’s Garage” album. I mean, it was just like forever watching. And I would feel – it was like a shroud over me. And I would come home on pins and needles. I didn’t know if I would, you know, get laid into or he would smile and praise me. It was kind of a tough situation.
DAVIES: And that continued into your major league career, too, right?
HERNANDEZ: Yes, it did.
DAVIES: Well, I’m sure he was a great guy. And he died in 1992. Right?
HERNANDEZ: He did, ironically, one year after my retirement. So it was too bad he couldn’t have lived longer.
DAVIES: We’re speaking with Keith Hernandez. His new memoir is called “I’m Keith Hernandez.” We’ll continue our conversation in just a moment. This is FRESH AIR.
(SOUNDBITE OF RUDY ROYSTON’S “BED BOBBIN'”)
DAVIES: This is FRESH AIR, and we’re speaking with Keith Hernandez. He spent 17 years in the big leagues, had World Series teams with the St. Louis Cardinals and New York Mets. He has a new memoir called “I’m Keith Hernandez.”
I want to talk about playing first base. First base is a natural place for collisions. Right? I mean, when there’s a ground ball, you’re there to catch a throw from the infielder. And hopefully, it’s on target. But it might be into the path of the runner, who may not see it…
HERNANDEZ: Yes.
DAVIES: …Because the runner is busting it down the line, not necessarily looking at the throw. When you could see that was going to happen – the ball was going to be into the path of the runner – did you have techniques for either warning the runner or just trying to avoid getting hurt or hurting the runner?
HERNANDEZ: Well, No. 1, the runner can’t run inside the baseline. He’s got to be on the chalk. So a throw into him or I got to stretch towards home plate, I feel pretty confident that I’m not going to get hit. It’s up to me to make sure that I stride in fair territory towards the ball – I stretch. Excuse me.
And the only time I was ever scared – when I was older, in my last year in Cleveland, Oakland Raider running back that played for Kansas City, All-American Bo Jackson, hit a ground ball to shortstop. And the throw was down the line into him. And I heard him running like – he was like a herd of buffalo.
DAVIES: (Laughter).
HERNANDEZ: I’m not exaggerating. I’d never had that experience before, and I played against some big guys.
He was running so fast, and he was such a big, strong guy that when I – I remember I cringed when I caught the ball just in hopes that he wouldn’t clip me on my left shoulder. And he missed me. Thank goodness. I made sure I stretched up the line, but that’s the only time ever in my career.
If the throw is too far up the line, you make a judgment. First base was a part of me, and that’s also an extension of knowing where the runner is. I have good peripheral vision. I have good sense of where the runner is. Can I come off the bag? Instead of stretching, can I just come off the bag and get the ball and make the tag instead of staying on the bag? I was able to do that. It was just all second nature to me.
The easy part of the game for me was fielding. If hitting could have been as easy as fielding, I would have hit .400.
DAVIES: (Laughter).
The other thing about playing first base, it’s the one place where there are a lot of – there’s time to converse with an opposing player. A player – a base runner gets on. And you know, I mean, the pitcher and catcher – I mean, the hitter and catcher are near each other, but they’re kind of busy. The catcher’s getting the signs.
When you’re with a runner at first, you’re often waiting for the pitcher to get ready. And you can see there’s chatter.
HERNANDEZ: Yes.
DAVIES: Is it friendly? Were there guys who’d try and use that to get in your head? Or would you try to get in other players’ heads?
HERNANDEZ: I was a chatterbox and for one reason. I would ask the hitters how they felt at the plate. And if a hitter would – it was just the beginning when the – in the old days, you would never talk to the opposing player during a game, before a game in BP. There was no – it was the enemy. And that was starting to change in my era. It started to change in the ’60s. And in the ’70s, it even got – it advanced further.
But I’d always ask, you know, if a guy came to the – first base, how do you feel at the plate? And if they start, well, you know, I don’t feel so good da-da-da-da-da (ph). Oh, man, I feel great. Well, I’m in a hot streak. You know, well, I would relay that information.
DAVIES: To your pitcher.
HERNANDEZ: Rick – yes. And – actually, to the pitching staff and – or the pitching coach. Rick Monday had a funny story. Rick Monday’s a very dear friend. He now does radio for the Dodgers. He goes, oh, we’re flying into St. Louis. Hernandez is on first base. We better all hit doubles…
(LAUGHTER)
HERNANDEZ: …So they wouldn’t have to talk to me (laughter).
DAVIES: You know, game has changed since you played. I mean, we now have – they count visits to the mound. There are challenges. There are instant replays. What do you think of the game today?
HERNANDEZ: Well, I really feel that they’re – the game is going through radical changes. I don’t – all the analytics, I’m kind of – when I finished this book, my – I wish it had been nine months later because I’m kind of getting a grasp of analytics. And I’m kind of – I’ll never 100% go with them, but I’ve talked to too many former players, teammates that are in front offices and say, hey, you can really be surprised what you can wean from analytics. It’s so precise, so in-depth. OK. Fine. I’m coming around on that.
But still, statistics are sterile. I miss the complete game – the pitcher going nine innings. And you know, I can’t blame the pitchers today. That’s what – how they’re brought up – you know, five innings and they’re gone, a hundred pitches, they’re gone. I can’t sink my teeth into it. I can’t wrap my arms around that. I think it lowers the bar. And it’s all about excellence, striving to be the best that you can be. I don’t want someone to come in and finish that game for me. I want to finish the game – or if it’s an inning and you’re in trouble and they take him out – which they do because it’s a pitch count – let him finish the inning.
So I don’t want to go on and on and on. But that’s the way the game is, and that’s the way it’s going to be. And I’ve come to – I’m at peace with it, so I’m not going to get all riled about it. And it’s just the way it is. And I do miss how the game was played before – you know, a couple decades before.
DAVIES: Well, I don’t mind you getting riled at all. What about the pace of play?
HERNANDEZ: Well, I think the big culprits are the pitchers. And I see so many 0-2 counts where they’ve got the hitter really backed up against the wall. I’m in trouble when I’m 0-2. And they don’t know how to pitch and put a – blow a pitcher – blow the hitter away. It goes, inevitably, to 3-2. That adds to pitch count. That adds a – now you’re not going to go seven innings. Now you’re going to go six, maybe five and two-thirds.
And here comes the bullpens. And a lot of the bullpens stink and – guys that come in and don’t throw strikes. I’ve talked to scouts. They look at the guy get the ball the furthest ’cause of home runs in and the pitcher that can throw the hardest. It’s no longer pitch to contact.
Warren Spahn wasn’t a hard thrower, the greatest left-hander of all time. Warren Spahn had a screwball – watching Warren Spahn pitch was like watching Rembrandt paint a masterpiece – on the corners, low, a little extra here, a little off there, screwball here, up-and-in fastball there. These hard throwers – they don’t have the command of their breaking ball. And Major League hitters can hit fastballs, and that makes for long counts and makes for long games. And now you got the analytics, and I’m up there going absolutely out of my mind.
DAVIES: I’m not enough of a baseball geek to really know what Hall of Fame numbers look like, but, I mean, you’ve won 11 straight Gold Gloves. You were a career .296 hitter with 162 home runs. You had a batting title, an MVP award, two World Series rings. Why aren’t you in the Hall of Fame?
HERNANDEZ: Well, my father – I was a really, really good athlete. And I used to be able to run pretty good – not fast, but above average. I stole 19 or – 19 bases in 1982. Home runs – made a lot. I played in St. Louis. It was 386 in the gaps. It was 335 down the lines.
DAVIES: Big park.
HERNANDEZ: It was a huge park.
DAVIES: Yeah.
HERNANDEZ: And it was sunken and underground one street level. And the only open-air part of the ballpark was from left-center to right-center, and it would blow in. And when it got hot in the summer, you had to hit line drives. And we called it Death Valley. And I was a line drive hitter anyway.
So the 162 home runs, whatever it is – you know, if I’d have played at Wrigley Field or if I’d have played at Veterans Stadium or Three Rivers Stadium, I probably would’ve hit over two home – 200 home runs, and that would’ve helped, which means more RBI. I drove in over a thousand runs. So I lost some time playing with some two-strikes and two lockouts, you know? Those are games that won across the board that I wasn’t able to play.
DAVIES: Does it bother you that you’re not in the…
HERNANDEZ: No, and I’ll tell you why. When it’s all said and done and I’m long gone, who’s going remember? And you know, I’m not going to worry about it. What bothers me the most, Dave, is my .300 lifetime batting average. I’m at .296.
And ironically, my childhood idol – born on the same birthday as him – Mickey Mantle, October 20 – when I got my first baseball card and I saw that, he was my idol. I always had a 7 on my back. That is Mickey’s pet peeve. I read in his biography that he lost, ’cause of injury – he stayed around too long – he lost his .300 lifetime batting average. And ironically, I’m in the same boat. I’m a .300 hitter. I’m not a .296 hitter.
DAVIES: Keith Hernandez, it’s been fun. Thanks so much for speaking with us.
HERNANDEZ: I can’t thank you enough for having me.
DAVIES: Keith Hernandez is now a broadcaster for New York Mets games. His book, now in paperback, is called “I’m Keith Hernandez.”
After a break, we’ll remember former pitcher Jim Bouton, whose book “Ball Four” is still regarded as a classic, and actor Rip Torn, best known as the gruff producer Artie on “The Larry Sanders Show.” Both died this week. Also, John Powers reviews the British television series “London Kills.” I’m Dave Davies, and this is FRESH AIR.
(SOUNDBITE OF SONG, “TAKE ME OUT TO THE BALL GAME”)
DR JOHN: (Singing) Take me out to the ballgame. Take me out to the crowd. Buy me some peanuts and Cracker Jack. I don’t care if I never get back ’cause let’s root, root, root for the home team. And if they don’t win, it’s a shame ’cause it’s one, two, three strikes, you’re out, at the old ballgame.
Copyright © 2019 NPR. All rights reserved. Visit our website terms of use and permissions pages at www.npr.org for further information.
NPR transcripts are created on a rush deadline by Verb8tm, Inc., an NPR contractor, and produced using a proprietary transcription process developed with NPR. This text may not be in its final form and may be updated or revised in the future. Accuracy and availability may vary. The authoritative record of NPR’s programming is the audio record.
Remembering Major League Pitcher Jim Bouton, Author Of ‘Ball Four’
Bouton, who died Wednesday, spoke to Fresh Air in 1986 about his 1970 tell-all memoir, in which he drew on his seven years with the New York Yankees to offer an insider’s guide to baseball.
DAVE DAVIES, HOST:
This is FRESH AIR. I’m Dave Davies, in for Terry Gross. Jim Bouton, the former big-league pitcher better known for his prose than his fastball, died Wednesday at his home in Massachusetts. He was 80.
In 1970, Bouton wrote the book “Ball Four,” a raunchy insider’s look at the game that drew heavily on Bouton’s seven seasons with the New York Yankees. He wrote about players getting drunk, peeping through keyholes at women and popping amphetamines like candy. The book enraged players and some sportswriters and drew a rebuke from commissioner Bowie Kuhn, but it was a bestseller.
After a respectable baseball career, Bouton wrote several other books, did some acting and sportscasting and was a George McGovern delegate to the 1972 Democratic convention. Bouton spoke with Terry in 1986 and began with a story from “Ball Four” about Mickey Mantle.
(SOUNDBITE OF ARCHIVED NPR BROADCAST)
JIM BOUTON: I think the most controversial story in the book was I told about the time Mickey Mantle hit a home run with a hangover. And it wasn’t really even so much as a put-down of Mickey Mantle as it was a story of what a great athlete he was. I told about the time we were in Minnesota. And we’d been out the night before a game, having a few drinks – about 2 o’clock in the morning, I guess it was. I don’t want to say Mickey was drunk, but he spent about a half an hour trying to make a telephone call from a grandfather’s clock.
So he comes into the ballpark the following morning, and he’s hungover. And the manager says, you know, sleep it off. Most managers were players themselves. They understand you come to the ballpark once in a while with a hangover.
So Mick is sleeping in the trainer’s room. We’re playing the Minnesota Twins. We get – stick somebody else in the outfield. And so the game’s going on, and it gets tie score after nine innings. And in about the 12th inning, the manager says, I hate to do it, but I need a pinch hitter in the 13th. Go in and wake up the Mick.
So we go in the trainer’s room, you know, wake up Mickey Mantle, dress him in his uniform, steer him through the tunnel up into the dugout. Thirteenth inning comes around – he put a bat in Mickey’s hands and point him in the direction of home plate. The Mick staggers up to the plate. Fortunately, he’s a switch hitter – doesn’t matter what side he gets on – steps into the batter’s box.
To show you what a great athlete this guy was – and Mickey was the best ballplayer I ever saw – he takes one practice swing and hits the first pitch into the center field bleachers, a tremendous blast 450 feet away. We win the game. The crowd is going nuts, and the players are going crazy in the dugout. We’re laughing and pointing and screaming and slapping each other on the back. And suddenly, it occurs to us he still has to round those bases.
TERRY GROSS: (Laughter).
BOUTON: There’s a rule in baseball that you must touch the bases in order. Fortunately, he heads off in the right direction. The minute he hits first base, the entire dugout goes, make a left – goes around, touches second, touches third, comes across, misses home plate – we have to send him back for that – comes over to the dugout.
And, of course, the fans are giving him a standing ovation. And as he’s waving to the crowd, he looks at us in the dugout, and he says, those people don’t know how tough that really was. I went over to his locker afterwards, and I said, how did you do that? You couldn’t even see up there. He said, it was very simple. I hit the middle ball.
GROSS: (Laughter).
BOUTON: So if this destroys America’s illusions about baseball or Mickey Mantle, then I don’t know what you do with all the literature that’s come out since then where each player tries to top the next in terms of what he can tell or how far he can go.
GROSS: Pitching careers are subject to more problems than other careers are, I think, because your arm is so vulnerable. And your career depends on your arm, and it’s what you’re abusing all the time.
BOUTON: Sure. And pitching is not a natural motion. Throwing a ball as hard as you can 120 times every four days is not natural.
GROSS: Did you have to change your pitching style because of injuries you were getting?
BOUTON: Well, I had to change my pitching style when I wasn’t able to throw hard anymore. See, what happened was I threw very hard when I first came up. I was a overhand fastball pitcher. And then when I hurt my arm, I wasn’t able to throw hard for a while. And then when I did, it – the ball didn’t have that zip on it anymore. It didn’t have that snap. Even though the ball was traveling as fast, it wasn’t moving.
So it’s like taking a rubber band and stretching it too far, and then it never gets its elasticity back again. And that’s what happened to my arm. So I had to change from being a fastball pitcher to a knuckleball pitcher.
Fortunately, when I was a kid, I threw a knuckleball, which is not a pitch that requires very much strength. It’s a skill pitch. You push it off with your fingertips. The idea is to get the ball to go through the air without any rotation, and then it jumps around all by itself. And so I became a knuckleball pitcher to compensate for the fact that I couldn’t throw hard anymore.
GROSS: How hard are knuckleballs to hit?
BOUTON: They’re almost impossible to hit when you throw a good one. The difficulty is throwing a good one. When you don’t throw a good one, anybody can hit them. That’s the problem with a knuckleball. Nobody can hit a well-thrown knuckleball, and almost anybody can hit a poorly thrown knuckleball.
GROSS: Say it was a full count, and there were a couple of men on base. What would you throw? Would you throw a knuckleball, knowing that if you made one more – one wrong move, it might be a home run ’cause…
BOUTON: Yes.
GROSS: …It’s easier to hit?
BOUTON: I would throw a knuckleball. I would throw a knuckleball because my feeling is I would rather live and die with my best pitch than take a chance with something that wasn’t my best.
GROSS: Did you have any gestures that you had to do before you threw a pitch and, like, rub your hand on your side three times or (laughter)…
BOUTON: Nothing that was superstitious. Sure, I went through the same sort of little rituals before I threw the ball because it’s important to do that. And athletes need to do that and many performers need to do that because those are the little steps that are really part of the process.
Throwing a ball is not just throwing a ball. Part of it starts when you walk out to the mound – how you walk out to the mound, how you feel about yourself and the fans and the batter and the whole – I mean, all of that – the rosin bag in your hand, how the ball feels. And you want to start playing with that ball in your hand so you get that feeling, and you want to recreate the memory – the muscle memory that brings you back to the last time you were really throwing well. And that whole process starts long before you actually throw the ball.
GROSS: Why do pitchers like to chew when they’re on the mound?
BOUTON: Part of it is because of the nervousness and the tension. And it’s sort of – chewing relieves that. But the spitting part is different, OK? Spitting – and also all this crotch grabbing and spitting back and forth that you see in Major League Baseball – there’s a real reason for that. There’s a behavioral reason for that. And that is that what these are is macho displays, OK? It’s a man-to-man challenge out there, the pitcher versus the batter. And it’s very much like two cats squaring off where they both have to sort of urinate on the shrubbery, saying, OK, this is my yard. I own this space. And the other cat’s saying, yeah, but I own my space, and then they’re fighting.
You see, what the batter is is – he steps into the batter’s box and he spits all over the place. He’s saying he’s – that’s his turf. The pitcher is saying, oh, yeah? Well, (imitating spitting) this is my turf out here, and now we’ll see who’s the best. And so that’s why you have that. It’s that mano-a-mano challenge situation, you know? And that’s what they are. They’re animals marking their territory.
GROSS: Jim Bouton, I want to thank you very much.
BOUTON: Thank you. I’ve enjoyed it.
DAVIES: Jim Bouton spoke with Terry Gross in 1986. Bouton died Wednesday at the age of 80. Coming up, we’ll remember actor Rip Torn, best known for his role as Artie on “The Larry Sanders Show.” This is FRESH AIR.
(SOUNDBITE OF WES MONTGOMERY’S “FOUR ON SIX”)
Copyright © 2019 NPR. All rights reserved. Visit our website terms of use and permissions pages at www.npr.org for further information.
NPR transcripts are created on a rush deadline by Verb8tm, Inc., an NPR contractor, and produced using a proprietary transcription process developed with NPR. This text may not be in its final form and may be updated or revised in the future. Accuracy and availability may vary. The authoritative record of NPR’s programming is the audio record.
A Call For More Research On Cancer’s Environmental Triggers
A stretch of the Mississippi River from New Orleans to Baton Rouge, La., that is crowded with chemical plants has been called “Cancer Alley” because of the health problems there.
Giles Clarke/Getty Images
hide caption
toggle caption
Giles Clarke/Getty Images
We already know how to stop many cancers before they start, scientists say. But there’s a lot more work to be done.
“Around half of cancers could be prevented,” said Christopher Wild in the opening session of an international scientific meeting on cancer’s environmental causes held in June. Wild is the former director of the World Health Organization’s International Agency for Research on Cancer.
“Cancer biology and treatment is where most of the money goes,” he said, but prevention warrants greater attention. “I’m not saying that we shouldn’t work to improve treatment, but we haven’t balanced it properly.”
Perhaps no question about cancer is more contentious than its causes. People wonder, and scientists debate, if most malignancies stem from random DNA mutations and other chance events or from exposure to carcinogens, or from behaviors that might be avoided.
At the conference in Charlotte, N.C., scientists pressed for a reassessment of the role of environmental exposures by applying modern molecular techniques to toxicology. They called for more aggressive collection of examples of human pathology and environmental samples, including water and air, so that cellular responses to chemicals can be elucidated.
The hope is that by identifying specific traces of exposures in human cancer specimens, scientists can identify environmental causes of disease that might be prevented.
“Over 80,000 chemicals are used in the United States, but only a few have been tested for carcinogenic activity,” said Margaret Kripke, an immunologist and professor emeritus at MD Anderson Cancer Center, in an interview at the meeting.
“This has been a very neglected area of cancer research for the last several decades,” said Kripke, the driving force behind the conference, which was put on by the American Association for Cancer Research. “Environmental toxicology was very popular in the 1950s and 1960s,” she said, but genetics then began to overshadow studies of cancer’s environmental causes. “Toxicology fell by the wayside.”
While the incidence of tobacco-linked cancers has been falling, malignancies not associated with smoking are rising, Kripke said. Recent evidence suggests an escalating rate of lung cancer in nonsmokers. That trend implicates other environmental factors.
Around the globe, cancer’s overall incidence is climbing. This year, 18 million people will be diagnosed with some form of cancer and over 9 million will die from it.
Infections — many preventable, such as by human papillomavirus —account for 15% of new cases.
Another rising cause is obesity, along with urbanization. People generally get less physical activity and eat differently in cities, and pollution is heavier there, too. “As people move into cities, that will drive up cancer rates,” Wild said.
One of the biggest obstacles to preventing cancer is that many people just don’t think it’s feasible. Progress “requires long-term vision and commitment,” Wild said. “Funding is limited, and there’s little private sector investment.”
A change in the way benefits of cancer prevention are framed could help. “When I was at the IARC, one thing that struck me was the power of economic arguments over health arguments for preventing cancer,” Wild said.
Cancer treatment costs can be prohibitive. But productivity lost from premature deaths in Brazil, Russia, India, China and South Africa alone runs $46.3 Abillion annually, he said. “Developing countries are not prepared to deal with the rising cancer burden.”
The precise proportion of cancers arising from environmental and occupational exposure to carcinogens is uncertain. In 2009, a report by the President’s Cancer Panel called prior approximations of around 6% “woefully out of date” and low. A 2015 paper by over a hundred concerned scientists cited “credible” estimates of 7% to 19%.
Scientist at the Charlotte meeting emphasized the complexity of cancer’s causes and the need for toxicologists to update methods to reflect that complexity, such as by studying interactions of environmental and genetic risks, and by examining cells after a mix of exposures. “Most toxic exposures do not occur singly,” said Rick Woychik, deputy director of the National Institute of Environmental Health Sciences.
Until recently, many toxicology tests were performed in rodents, because it would be unethical to deliberately evaluate possible carcinogens in people. But these animal experiments are labor-intensive and slow, he said.
New alternatives are now being tried. “We learned from pharma that with robotics and high-throughput technology you can interrogate a lot of biology quickly and at lower costs,” he said.
Epidemiological research of human exposures has been stymied by the difficulty of proving cause-and-effect — that a particular substance actually causes cancer — and by shortcomings of survey data from questionnaires.
At the conference, scientists offered glimpses of new technology that is helping fill informational gaps.
Bogdan Fedeles of MIT explained how DNA serves as a lifelong “recording device.” He and others use duplex sequencing to examine human samples for genetic “fingerprints of exposure.”
Allan Balmain, a geneticist at University of California, San Francisco, spoke about mutational signatures in malignancies. In liver cancer, for instance, these signatures can offer causal clues—such as smoking, alcohol or aflatoxin, a product of mold that grows on some foods.
Many chemicals that cause or stimulate cancer growth are produced inside our bodies. “It’s not all about the environment,” Balmain said.
Others highlighted a conceptual shift in how scientists define carcinogens. Key characteristics may include a substance’s capacity to stimulate growth of malignant cells, or to induce inflammation—without necessarily causing DNA damage, long seen as the necessary .
“The answer to ‘What is a carcinogen?’ is changing” said Ruthann Rudel, a toxicologist at the Silent Spring Institute who has published extensively on breast carcinogens. She detailed new techniques to screen breast cancer cells for changes in response to specific chemical exposures.
The public health stakes for the field are high.
Professor Polly Hoppin, of the University of Massachusetts, Lowell, discussed cancer-causing industrial contamination of drinking water at Camp Lejune, N.C., air pollution in St. John the Baptist Parish, La., and potential exposures to carcinogens from fracking and planned plastics production in Pennsylvania.
Hoppin reflected on the U.S. experience with tobacco cessation. Scientists knew that smoking causes cancer by the 1950s, she said. Implementing that knowledge required policy and incentives — like high cigarette taxes and public smoking bans — and took decades.
“The science wasn’t enough,” Hoppin said. “How many lives could have been saved if we’d acted sooner?”
Elaine Schattner is a physician in New York writing a book on cancer attitudes that will be published by Columbia University Press.
As Its Drug Pricing Plans Fall Through, Trump Administration Turns To Congress To Act

Secretary of Health and Human Services Alex Azar announced his agency is dropping a proposal intended to lower drug prices.
Michael Brochstein/SOPA Images/LightRocket via Getty Images
hide caption
toggle caption
Michael Brochstein/SOPA Images/LightRocket via Getty Images
The Trump administration has dropped one of the meatiest portions of its plan to reduce drug prices.
The Department of Health and Human Services said it will no longer pursue a rule that would have prohibited the payment of certain rebates on drugs in Medicare Part D and Medicaid plans.
The idea was to target the middlemen, pharmacy benefit managers, whose negotiations with drugmakers and insurers influence the costs consumers pay for drugs.
The hope was the rule would have effectively pressured drugmakers to give discounts to consumers instead of middlemen, HHS secretary Alex Azar said in remarks to the media in February. “Passing discounts directly on to the patient will move us toward a real market for drugs,” said Azar. “We’re going to fundamentally rewire how we pay for drugs in this system.”
Right now, if you’re a Medicare Part D beneficiary, and you need to pick up a drug that has a $120 list price, you might have to pay that full price, even if the middleman that negotiates on behalf of your insurer only pays a net price of $100 for it, after rebates. The idea of this proposal was that the consumer would only have to pay the discounted price.
When the rule was first announced, drugmakers supported the idea, and some drug pricing experts said it could be an effective move. “This is a huge potential change, transformative,” Dr. Walid Gellad, director of the Center for Pharmaceutical Policy and Prescribing at the University of Pittsburgh told NPR.
But some critics were concerned that the move wouldn’t address drugs’ list prices that are the starting point for negotiations.
Also, there was a worry that the elimination of rebates could ultimately cost seniors more, in higher premiums on their Medicare plans. The nonpartisan Congressional Budget Office in May determined the plan would cost the federal government $177 billion over nine years, largely from increases in the government’s share in the cost of premiums.
In a briefing with reporters Thursday, Azar said the administration scrapped the plan after getting feedback from the public and stakeholders. “At the end of the day, while we support the concept of getting rid of rebates, while we appreciate and are passionate about the problems and the distortions in the system caused by this opaque rebate system, we’re not going to put seniors at risk of their premiums going up.”
“Congress perhaps might even take this up — they have more tools than we do,” Azar said. “They can actually look more holistically at changes to the system that could also mitigate or protect seniors from bearing any impact of change. I don’t have those tools; they might have those tools.”
A senior Trump administration official, who spoke on background during a separate briefing Thursday, echoed those sentiments, saying their primary focus is to support a legislative deal to lower drug prices and that there was concern this change would disrupt those efforts.
Drugmakers were in favor of trying to bring consumer prices down by targeting middlemen. The drug industry trade group PhRMA called the rollback of the plan “a blow to seniors who could have paid less for their medicines at the pharmacy counter.”
“Of all the policies proposed in Washington right now, this was the only proposal that would provide immediate savings at the pharmacy counter, instead of only saving the government or insurance companies money,” said Holly Campbell, PhRMA’s deputy vice president of public affairs in a statement.
Other stakeholders cheered the administration’s reversal of the proposed rule, including groups representing private insurers, public sector health plans and pharmacy benefit managers. They pointed to the prices set by drugmakers as a better focus for efforts to reduce drug costs.
“Any solution should start with addressing drug prices,” T.J. Crawford, a spokesman for CVS Health, which operates a large pharmacy benefit manager, wrote to NPR.
Matt Eyles, president and CEO of America’s Health Insurance Plans, said in a statement: “As we all know, drug prices and price increases are set and controlled solely by drugmakers. They alone could decide to reduce prices – and can do so today.”
The rebate reversal is the second defeat for the administration on drug pricing in a week, coming just days after a court struck down another pillar of its drug pricing plans, a proposed regulation to require that drug companies disclose prices in ads.
Azar says the administration hasn’t given up on lowering drug prices. But Congress will have to play a bigger role. “We have many other things that we’re doing in drug pricing,” he says. “We are working on a bipartisan basis with Congress on drug pricing legislation.”
The White House official who briefed reporters Thursday said people in the administration don’t plan to “twiddle our thumbs” while the legislative process plays out, and are working on a number of plans.
President Trump hinted at one idea last week — a “most favored nation” clause that would tie American drug prices to what other countries pay. The administration has not released any details about how that would work or when it would roll out.
Young Undocumented Californians Cheer Promise Of Health Benefits
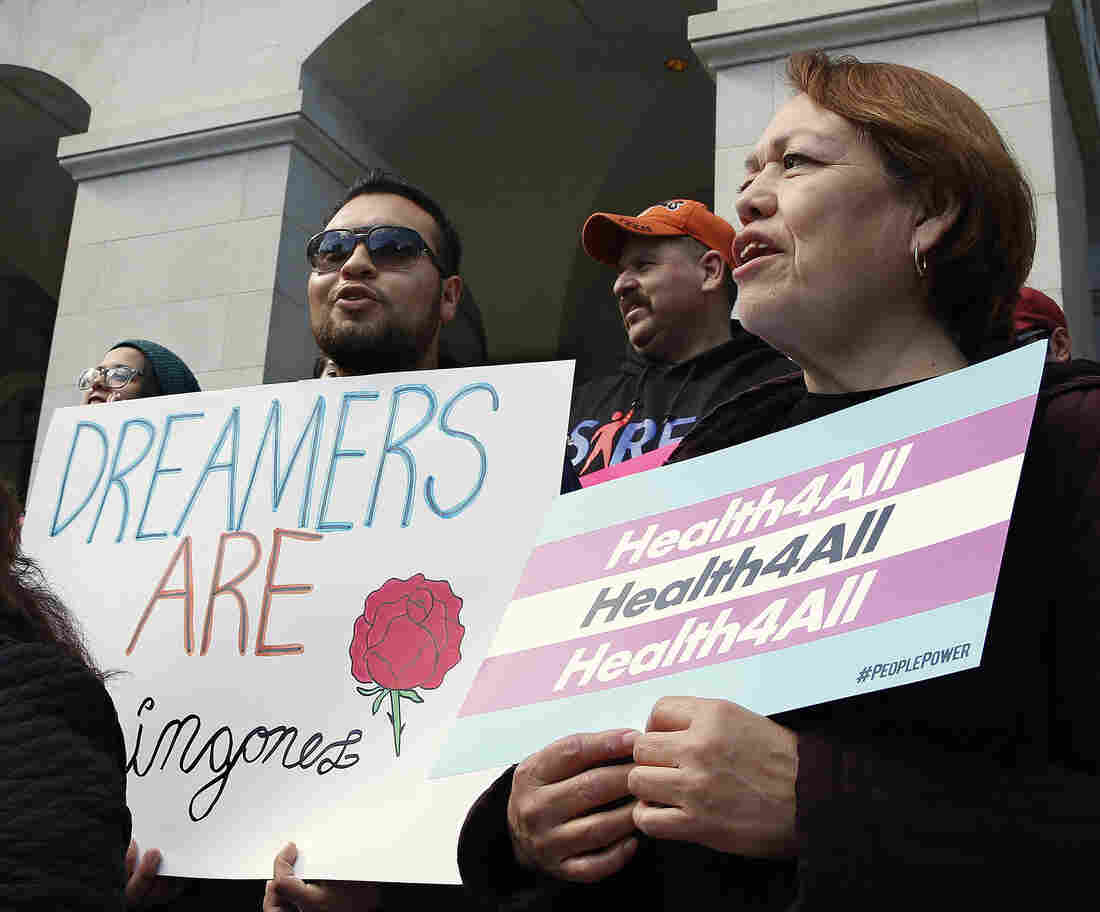
Demonstrators rallied in Sacramento in May for Medi-Cal expansion to undocumented Californians. When the state’s budget was finalized, only young adults up to age 26 were authorized to be included in the expansion. Gov. Gavin Newsom says that’s an important first step.
Rich Pedroncelli/AP
hide caption
toggle caption
Rich Pedroncelli/AP
For years, Beatriz Basurto’s family has had to make hard choices about when to pay for medical care, and who should get treatment.
“To me, it was always the doctor would be the last resort,” she says. “But for my parents, the doctor was never a choice. No matter how sick they got, they had to suck it up.”
Basurto, 19, says her parents always put the kids’ medical needs before their own. The family moved to California from Mexico more than 15 years ago. During that time, most of her family members have been ineligible for Medi-Cal, the state’s version of Medicaid, because they aren’t citizens.
Their situation started to change in 2016, when California expanded the program to all low-income children 18 and under, regardless of immigration status. That opened the doors for Basurto’s little sister to enroll.
And starting in January of 2020, Beatriz will be allowed to sign up, too.
California’s governor signed a law Tuesday that approved $98 million to expand Medi-Cal to income-eligible undocumented adults from age 19 until they turn 26, making it the first state in the United States to cover this group. California estimates 138,000 young adults will become insured under the new policy.
While the state has expanded options for children and young adults, most undocumented people in California still have limited access to health care. They can sign up for “restricted” Medi-Cal, but it only covers emergencies and pregnancy-related care. Many people on this plan end up putting off treatment or turning to county clinics for help.
Supporters who want to further expand Medi-Cal to all residents say that move would boost public health and bring down emergency room costs. California Gov. Gavin Newsom has vowed to make everyone eligible.
“We believe in universal health care,” he said during a speech this month. “Universal health care’s a right, and we’re delivering it — regardless of immigration status — to everyone up to the age of 26, and we’re gonna get the rest of that done, mark my words.”
But after months of debate at the California State Capitol, proposals to offer Medi-Cal to all undocumented adults, as well as a push to cover undocumented seniors, were deemed too costly.
Medicaid is a joint state-federal program, but California would use state dollars to pay for expanded benefits to immigrants living in the U.S. without legal permission.
Some lawmakers argued California should be spending health care dollars on its own citizens, rather than people who are not living in the state legally.
“We are going to be a magnet that is going to further attract people to a state of California that’s willing to write a blank check to anyone that wants to come here,” said state Sen. Jeff Stone, a Republican, at a recent legislative hearing.
President Donald Trump also criticized California for offering health insurance to undocumented people.
“They don’t treat their people as well as they treat illegal immigrants,” the Republican president told reporters in the White House on Monday. “It’s very unfair to our citizens and we’re going to stop it, but we may need an election to stop it.”
But advocates say California isn’t done fighting for Medicaid expansion.
Almas Sayeed, deputy director of the California Immigrant Policy Center, says providing health care is crucial, given federal anti-immigrant hostility.
“For young immigrants, it’s a moment of feeling like we don’t belong in this country,” she says. “We work really hard in California to make sure communities know that they do.”
Beatriz Basurto is eager to sign up for Medi-Cal this January. She attends community college near Los Angeles, and wants to become an environmental scientist. She hopes getting insurance will allow her to seek out mental health care for ongoing stress, some of which she attributes to hostile political rhetoric about immigrants.
“The world isn’t always so welcoming,” she says. “It can be really, really overwhelming. It exhausts you mentally. It’s almost like I have no time to feel anything, because there’s always something else I have to do.”
Brenda Huerta, an undocumented 22-year-old, was enrolled in a health plan through her university. But that coverage expired this summer, after she graduated. She says her college plan was great for checkups, but didn’t cover large expenses.
When Huerta broke her leg she ended up paying for her care out-of-pocket. And she’s still helping pay off hospital bills from when her mom had major surgery.
Huerta needs new glasses, and she wants to continue regular medical and dental care. But she isn’t sure if she’ll sign up for Medi-Cal next year. Even with coverage, she’s worried her costs will stack up.
“Paying the [student] loans that I have, I haven’t really been thinking about health insurance,” she says.
She and other young adults recently met with Gov. Gavin Newsom to lobby for the expansion of Medicaid eligibility to all Californians.
“Everyone in the room, we did talk about our struggles as undocumented people not having health insurance,” she says. “And we also mentioned how our parents suffer from not having health insurance, because it puts an economic burden on us.”
Newsom’s office estimated expanding eligibility to all undocumented adults would cost $3.4 billion. About two thirds of California’s roughly 2.2 million undocumented immigrants would qualify for Medi-Cal based on income guidelines.
Basurto says even though coverage for undocumented young adults is a small step in the larger battle for equal rights, it makes her feel more at home in the U.S.
“I do belong here,” she says, “regardless of what others say.”
This story is part of NPR’s health reporting collaboration with Capital Public Radio and Kaiser Health News.
Leaders From 13 States Urge Federal Court To Allow Supervised Injection Sites

Supplies sit on a check-in desk at a model of a hypothetical injection site in San Francisco, pictured here in September 2018. Local leaders from San Francisco are among a dozen local officials urging a federal court to allow an effort to open a supervised injection site in Philadelphia.
Eric Risberg/AP
hide caption
toggle caption
Eric Risberg/AP
Top officials from 13 states are joining Philadelphia in urging a federal court to allow a site to open where people can inject illegal opioids under medical supervision, the latest escalation in a legal battle with the Justice Department that may determine whether such facilities, known as supervised injection sites, can start to operate in America.
In Philadelphia, where drug overdoses — most involving opioids — kill three times as many people as homicides, a nonprofit called Safehouse has been working to launch an injection site as a way of combating the city’s opioid crisis.
But the Justice Department has mounted a legal challenge to block it before it opens, claiming such a site violates federal drug laws and would enable drug use.
A friend-of-the-court brief submitted Wednesday by leaders from five cities — Ithaca, New York City, Pittsburgh, San Francisco and Seattle — says injection sites, widely used in parts of Canada and Europe, need to be part of the way cities respond to the opioid crisis.
“The opioid crisis has taken a major toll on American cities and counties, including ours,” the city leaders wrote. “Despite our efforts, the existing methods of combating the opioid crisis have proven to be too little, or at least too late, for far too many of our residents.”
In a separate brief, attorneys general from Washington, D.C., and seven states including Michigan, New Mexico and Oregon also urged the court to allow the injection site to open. “As laboratories of experimentation and the primary regulators of public health, States should be free to adopt cutting-edge medical interventions,” the top state law enforcement officials wrote. The other top state law enforcement officials who signed on to the brief are from Delaware, Minnesota, Virginia and Colorado.
The opioid crisis has also resulted in an alarming death rate in the cities that are exploring injection sites like the one Philadelphia is pursuing.
In New York City alone, more than 1,000 people die every year from overdoses. “That means more New Yorkers die of opioid overdoses than from homicides, suicides and vehicle crashes combined,” the city leaders’ brief notes.
But legal uncertainty and other issues have slowed the efforts to open supervised injection sites. However, city leaders say they believe no other option is able to put a significant dent in lethal overdoses.
“These trends have continued despite extensive efforts by local governments and health departments to curb the crisis, including policies to expand medication-assisted treatment, clean needle exchanges, and the distribution of naloxone to first responders and public health workers,” the city officials wrote.
Justice Department officials have stated that the idea of a supervised injection site violates so-called crack house laws that make it a crime to own a property where drugs are being used, but Safehouse planners and an alliance of local leaders counter that statutes from the 1980s were never intended to apply to what they view as a medical facility in the midst of a public health crisis.
The city leaders write that the sites “would be places where drug users can obtain medical supervision and treatment. The act of allowing drug users to [inject drugs] in a supervised environment where they can be rescued if needed, rather than on the street or in a restroom stall.”
A barrage of other briefs were also filed to the federal court in Philadelphia on Wednesday both in support of and opposing the proposed site. Among them, one written by a group of 64 current and former law enforcement officials, including former Justice Department officials, claiming that federal prosecutors were “distorting federal drug laws” in trying to shut down the country’s first attempt at opening a supervised injection site.
But a group of six neighborhood associations around the Philadelphia neighborhood of Kensington, the heart of the city’s opioid crisis and the preferred location of the injection site, wrote a brief pleading with the court to not allow the site in their community, fearing such a facility would invite additional crime and drug trafficking.
“Law abiding citizens walking to and from work and young children traveling to school face the risk of getting caught in the violence and become targets for the dealers looking to increase their customer base,” wrote the neighborhood group, which filed the brief along with the city’s Fraternal Order of Police.
“The police, who are experts in this area, know what Congress knew. They know from bitter experiences that concentrating drug use in a place like the one that Safehouse proposes will bring more addicts, more dealers and more violent crime to neighborhoods that are already suffering,” the brief says.
Yet, the brief from the states’ attorneys generals argues that studies have shown that injection sites have proved to save lives in other countries, and that it is time for the U.S. to give the controversial measure a chance.
“States that are home to metropolitan areas should be free to experiment with this potentially lifesaving intervention, as well as others, without fear that public health nonprofits or doctors in their jurisdictions will be subject to prosecution,” the group wrote.
The case is pending in Philadelphia before U.S. District Judge Gerald A. McHugh, who will rule sometime after a July 22 filing deadline.
Once A Symbol Of Freedom, Sudan’s Pop Radio Station Has Fallen Almost Silent

“I’m trying to keep hope, because everyone is leaving, bro,” says Ahmad Hikmat, Content Director of Capital FM in Khartoum. “I am losing my team one by one.”
Yasuyoshi Chiba/AFP/Getty Images
hide caption
toggle caption
Yasuyoshi Chiba/AFP/Getty Images
When Omar al-Bashir was ousted from the Sudanese presidency in April of 2019, there was an explosion of new culture in Sudan. In a country under strict Islamic law, suddenly, graffiti appeared on walls. Music of all kinds blasted from speakers. Men and women commingled openly at a protest camp in front of military headquarters.
Standing as a stark example of these post-military crackdown changes is Capital FM — a popular music radio station that was at the center of the spring’s cultural revolution.
“It was just so beautiful, and we were just so proud that we’re soulful,” Ahmad Hikmat, Capital FM’s content director, says as he recalls the creativity that Capital exuded. “You’d wake up in the morning, and you’d hear a song on Capital Radio was D’Angelo. Who would play D’Angelo in the morning, you know? It’s just 91.6 FM that would do that.”
But the surge of cultural awakening ended when the military junta running the country violently broke up the protests in the capital city of Khartoum. Now, Capital FM, is fighting for survival.
Now, as Hikmat walks through the empty station, the walls are bare. The sound panels have been taken down. You can still see the dabs of glue that held up vinyl records of Keith Sweat, Kenny Burke, Ray Charles and The Roots that decorated the studio.
Pushing the envelop in a Islamist country, Capital FM had become a symbol for a modern Sudan. It started as a house music station and then became a cultural hub. They had even begun hosting parties with DJs and bands where young Sudanese could quite literally let their hair down. But since the militarization of Khartoum, government censors have been taking the station off the air for hours at a time. To Hikmat, this is a clear warning sign that soon, security forces will break down Capital FM’s doors and confiscate everything — so he has started taking the place apart.
“It’s a bit dark now at the moment, because we painted the walls black because of everything that is happening,” Hikmat says.
Pushing the envelop in a Islamist country, Capital FM had become a symbol for a modern Sudan. Now, the station’s airwaves have gone almost silent.
YASUYOSHI CHIBA/AFP/Getty Images
hide caption
toggle caption
YASUYOSHI CHIBA/AFP/Getty Images
Hikmat says that one of his main jobs at Capital is to keep what it represents — a utopia of progressiveness — intact. Recently, that has been a particularly difficult task. One Capital FM staffer was killed at the protest camp, and many others question whether an enterprise like Capital is even possible in Sudan at this point. “I’m trying to keep hope because everyone is leaving,” he says. “I am losing my team one by one.”
To express what he feels in respect to the situation at Capital FM and in Khartoum, Hikmat says Marvin Gaye‘s “Make Me Wanna Holler” never leaves his mind.
“For me, this is the song that plays in my mind when I am driving in the streets, just looking at the leftovers,” Hikmat says. “I see those guys, you know, sitting there, chilling with their big-a** guns, and this song just plays in my head.”
Listen to the full aired story through the audio link.
USWNT Fans And Players Hope World Cup Win Will Help National Women’s League Succeed
NPR’s Audie Cornish talks with Rachel Bachman, senior sports reporter for The Wall Street Journal, about how this year’s World Cup title might help the National Women’s Soccer League thrive.


