Facing Critical Labor Shortage, Japan Opens Door Wider To Foreign Workers

In front of Japan’s parliament on Friday, people stage a rally against the bill to allow more foreign workers into the country.
Kazuhiro Nogi/AFP/Getty Images
hide caption
toggle caption
Kazuhiro Nogi/AFP/Getty Images
Japanese lawmakers have passed controversial legislation expanding the number of semi-skilled foreign workers who can live and work in the notably insular nation for up to five years.
Japan has been pressed to make the change because of a critical labor shortage that results from its rapidly aging society and low birth rate.
Japan’s upper house of parliament passed the law 161 to 76 just after 4 a.m. Saturday local time, after a day when the opposition parties tried to unsuccessfully to block the measure.
The law will go into effect in April 2019.
The legislation has been viewed as a last-resort measure by Prime Minister Shinzo Abe’s ultra-conservative government to address a severe shortage of workers in 14 industries, including restaurants, nursing, construction and agriculture.
According to the Associated Press, two categories of workers will be accepted, with conditions that will discourage them from trying to immigrate permanently.
The law will apply to as many as 345,000 less-skilled workers who will be allowed to stay for up to five years, but not bring in family members. It will also permit higher-skilled workers to enter with their families for 10 years and will provide them a path to Japanese citizenship. Both categories will have requirements for Japanese language competency.
Japan’s population is expected to decline from about 127 million to about 88 million by 2065, according to the National Institute of Population and Social Security. In September, Japan’s Internal Affairs and Communications Ministry released data showing that for the first time, one in five people in the nation is older than 70.
Japan has felt the pressure of an aging population and declining birthrates for decades. The government has tried to meet labor shortages by encouraging more employment of women and older workers, and using more robots and other automation.
And it does have foreign workers. Their number has more than doubled since 2000 to nearly 1.3 million last year, out of a working-age population of 67 million, according to the AP.
“Workers from developing Asian countries used to stay mostly behind the scenes, but not anymore. Almost all convenience stores are partly staffed by Asian workers and so are many restaurant chains.”
Many foreigners are working in Japan on training visas “that don’t allow them to switch jobs even if they are abused or underpaid,” says The Wall Street Journal editorial board. Thousands of student visa holders also work in Japan, often for longer than the 28 hours a week legally allowed.
But until now the government has resisted opening the door to a legal influx of semi-skilled foreign laborers, as many Japanese, particularly Abe’s right-wing supporters, fear a loss of cultural distinctiveness and homogeneity. It’s one reason the government has been careful not to characterize the new visa program as immigration.
But, as The Washington Post reports, Abe’s government is “closely entwined with the business community, and the message it hears from every quarter — shipbuilding and construction, agriculture and fishing, elder-care establishments and convenience-store owners — is ever more insistent: We need more workers.”
A report by Tokyo Shoko Research showed the number of bankruptcies in Japan caused by staff shortages doubled between 2016 and 2017, according to The Wall Street Journal.
Poll: Young People More Likely To Defer Health Care Because Of Cost

When to get care and when to pass often comes down to finances.
Johner Images/Getty Images
hide caption
toggle caption
Johner Images/Getty Images
If you’re not feeling well or have a routine health issue, do you go ahead and get it checked out or put if off because of the cost?
And, let’s say you do make an appointment and go. Afterward, do you fill the prescription you received or do financial concerns stop you?
We wondered how often people deferred or skipped care because of cost, so we asked in the latest NPR-IBM Watson Health Health Poll. The survey queried more than 3,000 households nationwide in July.
For starters we asked if people had postponed, delayed or canceled some kind of health care service, such as a doctor’s appointment or medical procedure, because of cost in the preceding three months. About 1 in 5 people had done so.
“I am pretty impressed that it was only 20 percent that had postponed or delayed or canceled health care services,” says Dr. Anil Jain, vice president and chief health information officer for IBM Watson Health. “I thought it would be higher.”
The proportion of people who said cost had deterred them from getting care varied by age, with a third of people under 35 saying it had been a problem compared with only 8 percent of people 65 and older.

Note: Question asked about health care in preceding three months.
NPR-IBM Watson Health Poll
hide caption
toggle caption
NPR-IBM Watson Health Poll
Jain says one area that may not be getting enough attention is preventive care. “I think it’s important that young people never feel the need to forgo or delay preventive services,” he says.
We also asked people if they – or members of their household — had difficulty paying for some kind health care service in the preceding three months. A quarter said yes. And again the strain varied by age, with 41 percent of people under 35 saying they had experienced difficulty while only 11 percent of people 65 and older had.
Almost all the respondents to the survey, about 97 percent, had some form of health coverage. The sample size of respondents reporting no insurance wasn’t large enough to support further analysis within the uninsured population.
We also asked specifically about people’s experience receiving and filling prescriptions. In the three months before the survey, two-thirds of people said they’d received a prescription. A vast majority of older Americans – 84 percent – said they’d received a prescription, while 39 percent of people under 35 had.
Almost everyone who said they’d gotten a prescription went ahead and filled it – 97 percent overall.
The cost of prescriptions appeared to be a bigger concern for younger people, with 38 percent of those under 35 saying they had difficulty paying for their medicine. Only 9 percent of people 65 and older said they had the same problem.
With an eye on costs, we asked people if they were familiar with discount coupons provided by drugmakers, one way to defray out-of-pocket expenses related to prescriptions. About two-thirds of people said they were aware of these coupons.
In a follow-up question, we asked if people had used this kind of coupon. About a third of people said they had. Among older people, 65 and up, the proportion was quite a bit lower – only 19 percent said they’d used this kind of coupon.
Drug costs weigh on people as deductibles and copayments add up.
“Despite insurance, we feel that more people are experiencing a higher out-of-pocket burden due to medications,” says Thomas Goetz, head of research for GoodRx, a clearinghouse for drug pricing information, discounts and coupons. “Insurance is increasingly not covering that expense as much as it used to.”
Manufacturers’ coupons are geared toward brand-name medicines, only one part of the financial challenge. “The burden for most Americans is largely with these generic drugs that are considered very routine to prescribe and are getting more expensive,” Goetz says. “A $20 drug becomes $100.”
Think of all the sacrifices people are making to avoid skipping prescriptions, he says. “We take these medications because they’re supposed to makes us feel better, and the price doesn’t always have that effect.”
The nationwide poll has an overall margin of error of plus or minus 1.8 percentage points. You can find the questions and full results here.
Federal Legislation Seeks Ban On Shackling Of Pregnant Inmates
As Congress prepares to adjourn for the holidays, one piece of legislation that’s still on the table is a bipartisan criminal justice bill known as the First Step Act.
It aims to improve federal prison conditions and reduce some prison sentences, a sticking point for some lawmakers. But the bill also contains a less controversial provision: a ban on shackling pregnant women.
Incarcerated people outside prison walls are considered potential flight risks. That label applies even to pregnant women when they leave prisons for medical care or to give birth.
These women are often restrained with handcuffs, ankle chains or shackles. Roughly two dozen states ban the practice of restraining incarcerated pregnant women during childbirth, but the First Step Act would apply to federal facilities.
The American Civil Liberties Union says shackling incarcerated pregnant women is “dangerous” and “inhumane.” The American College of Obstetricians and Gynecologists says it puts the health of the mother and baby at risk.
Carolyn Sufrin, a medical anthropologist and OB-GYN at Johns Hopkins School of Medicine, works with incarcerated pregnant women. She says that the U.S. correctional system was designed with men in mind.
“When you have something as gender-specific as pregnancy, it reminds you of how flawed the system is and how ill-prepared it is to take care of pregnant people and the reproductive health needs of women in general,” Sufrin says. “They’re, if at all, an afterthought.”
NPR’s Ailsa Chang spoke with Sufrin about the practice of shackling incarcerated women. The interview has been edited for length and clarity.
Interview Highlights
On why incarcerated pregnant women are shackled
The rationale behind shackling is not something that I understand. When taken off-site all incarcerated persons are presumed to be dangerous and a potential flight risk. A pregnant person needs to be taken off-site for medical attention and for childbirth.
So when she’s in a public space, the presumption is that she must be a flight risk and a public safety risk. Because of this default assumption, she needs to be restrained.
On delivering the baby of a shackled woman
When I was a first-year OB-GYN resident in training in Pennsylvania, I delivered the baby of a woman who was shackled to the bed. It made me more nervous and afraid and overwhelmed and also sort of confused me about my own role and my own complicity in this violence of shackling a pregnant woman in labor.
I had no idea that this was even possible and I didn’t know if I was authorized to ask the guard to unshackle her. I just kept worrying about what I would do if there was an emergency. Luckily, the birth itself went fine.
This was a deeply troubling moment for me, of course much more so for the woman herself, but it’s a pretty harrowing experience to have to practice medicine with someone who is in chains.
On the medical risks of shackling pregnant women
In labor, emergencies arise unexpectedly. We might need to do an emergency C-section if there are signs of distress or the baby’s shoulder could get stuck in the birth canal. When one of these emergencies arises, as a health care professional, we need to focus on our patient, not on asking a guard to unshackle her.
And there are dangers throughout pregnancy, not just in labor and childbirth. If a pregnant woman falls, she could have a dangerous condition where the placenta separates and she could hemorrhage. Shackles can increase her risk of falling and also prevent her from being able to break a fall.
But on top of these medical risks, it’s just common sense. The chances that a woman in the middle of labor, or even not in labor, can outrun someone and be a flight risk are just ludicrous.
I just gave birth six months ago and I can tell you that the thought of running off and escaping and outrunning anybody else is just ludicrous to me.
On the variability of medical care for incarcerated pregnant women
There are no mandatory standards that every prison and jail across the country has to follow when it comes to health services delivery. That means that every prison and jail has its own rules that it follows for pregnant people and the care they receive, including the use or nonuse of restraints.
But the issue really extends even much further than the use of restraints. It has to do with the entire health care for a pregnant person. There’s tremendous variability and you can have some places that provide excellent, comprehensive prenatal care and other places where it’s abysmal and even dangerous.
On why there’s still work to do to ensure proper care for incarcerated pregnant women
This bill would only pertain to women incarcerated in federal facilities and under the jurisdiction of the U.S. Marshals Service, so it would not pertain to people incarcerated in state prisons, which is where the majority of women are incarcerated. It would also not pertain to women housed in local jails. And on top of that, it only addresses the issue of shackling pregnant women. That is an important step to take, but it is only the tip of the iceberg when it comes to the care of pregnant and postpartum women in custody.
Rachel D. Cohen is an intern on NPR’s Science Desk.
Andrea Hsu and Jessica Smith produced and edited this conversation for broadcast.
A Push For Diversity In Medical School Is Slowly Paying Off

Currently students of color are underrepresented in medical schools, but their numbers are slowly growing.
Getty Images
hide caption
toggle caption
Getty Images
In 2009, the body that accredits medical schools issued a new requirement: All medical schools must implement policies that help them attract and retain more diverse students. Failure to do so can lead to citations from this body, the Liaison Committee on Medical Education, and can affect their status as accredited institutions.
This effort appears to be working. In a research letter published today in JAMA, researchers examine the changing demographics of medical students from 2002 to 2017. They found an increase in diversity in enrollment, especially since 2012, which the researchers think may be the first year new standards could be expected to have an effect.
But the rate of change, some medical educators say, is too slow. Medical student bodies were still 58.9 percent white in 2017.
“We see the trend going up, but it’s going up very slowly,” says Dr. Dowin Boatright, an assistant professor of emergency medicine at Yale University and coauthor of the study. “If we’re trying to get some degree of representation that matches the proportion of black people in the population as a whole … We’re talking 20 to 50 years.”
The pattern of change over the period studied is noteworthy, Boatright says. Between 2002 and 2012, the proportion of female and black students decreased each year.
In that same time period, the percentage of Latino and Asian students increased. White students were the majority of medical school enrollees throughout that time period.
In 2012, the percentage of female and black students starting medical school began a steady, albeit slow, increase.
Loading…
Don’t see the graphic above? Click here.
By 2017, 7.3 percent of new medical students identified as black, up from 6.8 percent in 2002. Students identifying as female made up 50.4 of matriculants, up from 49 percent in 2002.
Hispanics represented 8.9 percent of students, up from 5.4 percent in 2002 and Asian students were 24.6 percent of students, up from 20.8 percent.
Boatright hypothesizes that the improved numbers reflect that the new requirement that schools have formal programs to attract diverse students.
“I think there’s a strong incentive now to have at least some kind of benchmark to promote diversity,” Boatright says. “Programs actually are being held accountable.”
Many medical schools have hired dean-level administrators who focus on attracting and retaining minority students.
“When you tell people they should do something, they’re like, ‘Oh, we don’t have to do something,’ ” says Dr. John Paul Sanchez, the associate dean for diversity and inclusion at Rutgers New Jersey Medical School. “It makes people think differently when you say you must do something … People have more concrete direction.”
The Liaison Committee on Medical Education also requires that medical schools develop programs to improve the “pipeline” of minority applicants, which usually take the form of science education and mentorship programs for minority college and high school students.
Representatives of the Liaison Committee on Medical Education don’t interpret the data the same way Sanchez and Boatright do. The organization’s co-secretary, Dr. Veronica M. Catanese, said in a written statement that the organization has explicitly promoted diversity in its standards for “more than two decades” and while the organization’s expectations may encourage medical schools to pay attention to diversity, “it likely does not account for the correlation suggested by the authors of the letter.”
This trend the study identified is confirmed by the latest medical school enrollment data also released today by the Association of American Medical Colleges.
In 2018, 8.6 percent of first-year medical students are black, and more women than men started medical school: 51.7 percent identified as female.
The number of black men enrolling in medical school in 2018 — a group that has been significantly underrepresented compared to the general population — increased by 7.3 percent in 2018. Black men made up about 3.4 percent of first-year medical students this year.
This latest data differs from the data the JAMA study authors presented. To assess the effect of the new accreditation requirement, the authors excluded historically Black medical schools and all schools in Puerto Rico because they felt felt the new diversity standards would not affect them in the same way as predominantly white schools.
Sanchez says he thinks the accreditation standards are important, and encourage medical schools to devote money and time to supporting minority students. Still, he says, there’s a difference between meeting the standards and developing long-lasting programs that help minority students feel welcome in medical school.
“That takes decades to build. You can’t train someone to be passionate,” Sanchez says. “But you can hire them and bring them together to serve as faculty at the medical school.”
Mara Gordon is a family physician in Washington, D.C., and a health and media fellow at NPR and Georgetown University School of Medicine.
Medicare To Cut Payments To Nursing Homes Whose Patients End Up Back In The Hospital

Medicare’s new program will alter a year’s worth of payments to 14,959 skilled nursing facilities across the U.S., based on how often in the past fiscal year their residents ended up back in hospitals within 30 days of leaving.
BSIP/Getty Images
hide caption
toggle caption
BSIP/Getty Images
The federal government took a new step this week to reduce avoidable hospital readmissions of nursing home patients. The move targets the homes’ bottom lines by lowering a year’s worth of payments to nearly 11,000 nursing homes, and giving bonuses to nearly 4,000 others.
These financial incentives, determined by each home’s readmission rates, significantly expand Medicare’s effort to pay medical providers based on the quality of care instead of just the number or condition of their patients.
Until now, Medicare mostly limited these kinds of incentives to hospitals, which have gotten used to facing financial repercussions if too many of their patients are readmitted, suffer infections or other injuries, or die.
“To some nursing homes, it could mean a significant amount of money,” says Thomas Martin, director of post-acute care analytics at CarePort Health, which works for both hospitals and nursing homes. “A lot are operating on very small margins.”
The new Medicare program is altering a year’s worth of payments to 14,959 skilled nursing facilities, based on how often their residents ended up back in hospitals within 30 days of leaving.
Hospitalizations of nursing home residents, while decreasing in recent years, remain a problem: Nearly 11 percent of patients in 2016 were sent to hospitals for conditions that might have been averted with better medical oversight.
These bonuses and penalties are also intended to discourage nursing homes from discharging patients too quickly — something that is financially tempting as Medicare fully covers only the first 20 days of a stay and generally stops paying anything after 100 days.
Over this fiscal year, which began Oct. 1 and goes through the end of September 2019, the best-performing homes will receive 1.6 percent more for each Medicare patient than they would have otherwise. The worst-performing homes will lose nearly 2 percent of each payment. The others will fall in between. (You can check the scores for individual nursing facilities in your area here.)
For-profit nursing homes, which make up two-thirds of the nation’s facilities, face deeper cuts on average than do nonprofit and government-owned homes, a Kaiser Health News analysis of the data found.
In Arkansas, Louisiana and Mississippi, 85 percent of homes will lose money, the analysis found. More than half in Alaska, Hawaii and Washington state will get bonuses.
Overall, 10,976 nursing homes will be penalized, 3,983 will get bonuses and the remainder will not experience any change in payment, the KHN analysis found.
Medicare is reducing payments to 12 of the 15 nursing homes run by Otterbein SeniorLife, an Ohio faith-based nonprofit. Pamela Richmond, Otterbein’s chief strategy officer, says most of its readmissions occurred with patients after they went home, not while they were in the nursing facilities. Otterbein anticipates losing $99,000 over the year.
“We’re superdisappointed,” Richmond says about the penalties. She says Otterbein has started to follow up with former patients or with the home health agencies that send nurses and aides to patients’ houses to care for them. If there are signs of trouble, Otterbein will try to arrange care or bring patients back to the nursing home if necessary.
“This really puts the emphasis on us to go out and coordinate better care after they leave,” Richmond says.
Congress created the Skilled Nursing Facility Value-Based Purchasing Program incentives in the 2014 Protecting Access to Medicare Act. In assigning bonuses and penalties, Medicare judged each facility’s performances in two ways: how its hospitalization rates in calendar year 2017 compared with other facilities and how much those rates changed from calendar year 2015.
Facilities received scores of 0 to 100 for their performances and 0 to 90 for their improvements; the higher of the two scores was used to determine their overall score. Facilities were then ranked highest to lowest.
Medicare is not measuring readmission rates of patients who are insured through private Medicare Advantage plans, even though in some regions, the majority of Medicare beneficiaries rely on those to afford their care.
Through the incentives, Medicare will redistribute $316 million from poorer-performing to better-performing nursing homes. Medicare expects it will keep another $211 million that it would have otherwise paid to nursing homes if the program did not exist.
The new payments augment other pressures nursing homes face from Medicare and state Medicaid programs to lower readmissions to hospitals.
“Skilled facilities have been working toward this and knew it was coming,” says Nicole Fallon, vice president of health policy and integrated services at LeadingAge, an association of nonprofit providers of services for seniors.
The American Health Care Association, a trade group of nursing homes, reports in a written statement that it has supported the program and is gratified to see that more than a quarter of facilities received bonuses.
While most researchers believe that readmissions can be reduced, some consumer advocates fear that nursing homes will be reluctant to admit very infirm residents or to rehospitalize patients even when they need medical care.
“It may end up causing great pain to residents who actually need to be hospitalized,” says Patricia McGinnis, executive director of California Advocates For Nursing Home Reform, which is based in San Francisco.
Fallon says Medicare eventually may penalize homes that have done all they can to prevent return trips to the hospital. But because of the program’s design by Congress, Medicare still will need to punish large numbers of homes.
“There are always going to be winners and losers, even if you make good progress,” Fallon says. “At what point have we achieved all we can achieve?”
Meanwhile, Medicare is looking to expand financial incentives to other kinds of providers. Since 2016, it has been testing quality bonuses and penalties for home health agencies in nine states. Richmond, the nursing home executive, applauded that kind of expansion.
“There are a whole bunch of people in this chain” of institutions caring for patients at different stages, she says, “and we all need to be working in a common direction.”
Kaiser Health News, a nonprofit news service, is an editorially independent program of the Kaiser Family Foundation and is not affiliated with Kaiser Permanente. KHN data editor Elizabeth Lucas contributed to this report.
Trump's Move To Give States More Flexibility Undercuts Obamacare, Critics Say

The Trump administration said Thursday it wants states to innovate in ways that could produce more lower-cost health insurance options — even if those alternatives do not provide the same level of financial or medical coverage as an ACA plan.
Getty Images
hide caption
toggle caption
Getty Images
On his first day in office, as part of his mission to dismantle the Affordable Care Act, President Trump signed an order promising to give states flexibility “to create a more free and open healthcare market.”
The administration on Thursday released an official set of examples to help states flex these powers.
It is intended to roll back key elements of Obama-era requirements, which were designed to promote enrollment in ACA plans that cover a broad range of medical needs and meet uniform national standards.
Seema Verma, the Centers for Medicare & Medicaid Services administrator, said those strict rules were seen by many as burdensome, and “virtually impossible” for states to meet.
Instead, the Trump administration wants states to innovate in ways that could produce more lower-cost options, even if those alternatives do not provide the same level of financial or medical coverage as an ACA plan.
“I’m confident states will come up with ideas that will work better,” said Verma.
Still, coupled with other ongoing efforts by the Trump administration to gut Obamacare, policy experts predict the ideas would further foster a parallel market of cheaper, less robust coverage that could draw younger or healthier consumers, but drive up premiums for those who remain in ACA market plans.
“Invariably, the coverage is going to be more expensive for people who really need comprehensive coverage,” said Timothy Jost, a retired Washington and Lee University law professor who follows the ACA closely.
States could change who gets subsidies
One of the biggest changes signaled by the administration involves allowing states to revamp how federal subsidies are used. Currently, these subsidies are strictly targeted to lower-income Americans and are seen as key to bolstering enrollment in marketplace plans.
The Trump guidance would give states wider latitude to expand or narrow the income range eligible for subsidies, target them toward younger people or allow them to be used for less costly but skimpier types of insurance.
This would “potentially upend the subsidy structure,” said Sabrina Corlette, a research professor at Georgetown University’s Health Policy Institute.
Another example would, for the first time, make federal subsidy money available to people who get job-based insurance, countering Obama-era rules that generally prohibited that. It would let states use federal dollars to fund accounts consumers could use to buy insurance or pay other health costs, such as deductibles or copayments. Employers or consumers could also add additional funds to these accounts.
Still, managing those accounts would be a large administrative expense for a state to oversee, said Corlette. “I don’t understand why a state would want to set it up,” she added.
Supporters of Trump’s plan say the examples unveiled Thursday would give consumers more control over how they choose to spend their health care dollars and the types of coverage they want to buy. They say it might also improve the markets, which are seeing declining enrollment as premiums rise.
“If states can provide larger subsidies to younger individuals to attract them to enroll, that will improve the market overall,” said Christopher Condeluci, a Washington, D.C., attorney who specializes in employee benefits and has served as the tax and benefits counsel to the U.S. Senate Finance Committee.
However, if many states follow the administration’s lead, critics say, it would bring back the days when insurance rules varied widely state by state. Consumers could end up buying skimpier plans that leave them vulnerable to high, unexpected medical bills.
While not prescriptive, the examples are designed to encourage states to innovate and apply for permission to offer more choices for consumers, so long as the proposals don’t cost taxpayers more and don’t reduce access to ACA plans, said Verma.
State proposals would still have to be affordable, comprehensive and not raise the federal deficit, she said. And CMS would pay particular attention to potential effects on low-income Americans, she added.
Reshaping the individual insurance market
The administration’s examples focus on states’ health marketplaces, where insurance plans are designed for small businesses and for individuals who don’t get job-based coverage. An estimated 14 million people buy their own coverage through those markets or through brokers.
Premiums in those markets have risen substantially since the law took effect in 2014, for a variety of reasons. Among those reasons are lower-than-expected enrollment by healthy people; actions taken by Congress and the Trump administration that removed the tax penalty for failing to have coverage; and other moves that eliminated some payments to insurers and loosened restrictions on alternative types of insurance plans.
The administration’s examples add a new twist to a provision of the ACA that gave states the option of seeking a federal waiver to develop alternative marketplace proposals.
To get a waiver under Obamacare rules, however, states have to meet four “guardrails” established in 2015. These require states to ensure their proposals would provide equally comprehensive and affordable coverage; would not result in fewer people enrolling; and wouldn’t increase costs for taxpayers.
The examples described Thursday — touted as “waiver concepts” by the Trump administration — build on the administration’s guidance issued in late October to loosen those guardrails.
That October guidance, to take effect in 2020, says states have to provide access to affordable and comprehensive coverage, but will not be held to a strict tally of how many people actually enroll. So long as a state could show that equal numbers of people were buying some kind of coverage — either comprehensive ACA plans or less expensive but skimpier plans — the state’s approach could pass the test.
That October announcement, and Thursday’s concepts, drew immediate criticism from ACA supporters, who said it encourages the use of subsidies to buy short-term plans, which aren’t as comprehensive as ACA coverage and can bar people who have preexisting conditions.
Congressional Democrats sent a letter to top administration officials this week, saying the process by which the changes are being made is illegal, because the administration is not following a formal rule-making process.
“We believe this sub-regulatory guidance exceeds the Secretaries’ statutory authority,” wrote Ways & Means ranking member Richard Neal, D-Mass., and Energy and Commerce ranking member Frank Pallone Jr., D-N.J. “It appears to be part of the administration’s ideologically motivated efforts to sabotage the ACA.”
The Brookings Institution and other experts have raised similar questions and predicted a legal challenge.
“As soon as any state proceeds to go somewhere with this, there will be legal challenges,” said Jost.
Verma pushed back against this warning, noting that the Obama administration also issued its “guardrails” as guidance, not a formal rule.
Verma said she anticipated that critics would say the ideas would adversely affect people with preexisting medical conditions.
Those critics argue that anything that draws younger and healthier people out of the market will drive up costs for those who remain in ACA plans — including those with medical conditions, who might be barred from buying an alternative policy, such as a short-term plan.
But Verma said that “nothing in this guidance would take away protections from people with preexisting conditions.”
Kaiser Health News, a nonprofit news service covering health issues, is an editorially independent program of the Kaiser Family Foundation that is not affiliated with Kaiser Permanente.
Another Drug Crisis: Methamphetamine Use By Pregnant Women
Kristen Philman first tried methamphetamine in her early 20s, as an alternative to heroin and other opioids. When she discovered she was pregnant, she says, it was a wake-up call, and she did what she needed to do to stop using all those drugs.
Theo Stroomer for NPR
hide caption
toggle caption
Theo Stroomer for NPR
Kristen Philman had already been using heroin and prescription painkillers for several years when, one day in 2014, a relative offered her some methamphetamine, a chemical cousin to the stimulant amphetamine.
“I didn’t have any heroin at the time,” says Philman, a resident of Littleton, Colo. “I thought, ‘Oh this might make me feel better.’ “
It did, she says. Soon, she was using both heroin and methamphetamine on a regular basis.
“With heroin I would get sleepy, and then I needed the meth to kind of give me the boost,” she says. “It was a daily thing. I would do heroin and do meth on top of that.”
Then, in December, 2017, after a few months of missed periods, Philman took a home pregnancy test and the result was positive. “I was really scared, because I’d used meth and heroin from the day [my son] was conceived till the day I took the [pregnancy] test,” she says.
Philman is among thousands of women around the United States who used the stimulants methamphetamine or prescription amphetamines during their pregnancy in recent years, researchers say. While the trend has garnered little media attention, physicians in some regions have been struggling to tackle the problem and the impact of the drug on the women and infants.
Philman entered recovery once she was pregnant, and was put on methadone for her opiate use. She says her OB-GYN was candid with her about the potential effects of her meth use on the fetus — including premature birth and death.
Theo Stroomer for NPR
hide caption
toggle caption
Theo Stroomer for NPR
Since there are no medications to treat methamphetamine use disorder, some providers have had to improvise their approaches to treating these women, while many others remain unaware of the problem and how to deal with it.
A study published Thursday in the American Journal of Public Health confirms the rise in meth use among pregnant women and provides new data illustrating the scope of the problem. The research, which analyzed hospital discharge records between 2004 and 2015, found that as opioid use among pregnant women has grown in recent years, so has their use of amphetamines, and particularly methamphetamine.
Though that class of drugs includes prescription medicines like Adderall and Dexedrine that are sometimes used to treat attention deficit hyperactivity disorder, “we think our findings nearly entirely represent illicit methamphetamine use,” says Dr. Lindsay Admon, an assistant professor of obstetrics and gynecology at the University of Michigan and the lead author of the study.
The rise in amphetamine use began after 2008-2009, the study found. By 2015, however, tens of thousands of pregnant women were on the drugs.
“In total, we identified 82,000 deliveries that were affected by amphetamine use disorders,” says Admon.
According to the study, the increased rates of amphetamine use grew disproportionately in three regions of the U.S. — the South, the Midwest and the West. Rural areas had higher rates than cities, with the rural West having the highest rate of all regions. Opioid use among pregnant women on the other hand, was highest — 3 percent of all delivery hospitalizations — in rural northeastern United States.
“By 2014-2015, amphetamine use disorder was identified among approximately one percent of all deliveries in rural western United States,” says Admon. And that’s higher than the prevalence of opioid use among pregnant women in most regions in the country.
Health effects on mom and baby
Long term methamphetamine use during pregnancy has serious health risks for the mother, Admon says. It increase a woman’s risk of dying during or after childbirth or of having lifelong health complications — “things like blood transfusion, heart failure, cardiac arrest,” she says. “And then eclampsia — which is the most severe form of preeclampsia — where a woman has a seizure.”
“That’s something we’re seeing here,” says Dr. Tricia E. Wright, an OB-GYN and associate professor at the University of Hawaii John A. Burns School of Medicine. Wright has been treating pregnant women with methamphetamine use for many years.
The increased risk for preeclampsia signals an increased risk of heart attacks and stroke for the mother later on in life, she adds.
If the mother keeps using the drug through the pregnancy and doesn’t get prenatal care early on, the consequences can sometimes be fatal.
“I had a recent maternal death from methamphetamine use,” says Wright.
The woman was 28 weeks pregnant, “had a very bad heart disease” and did not receive any prenatal care, Wright says.
“She had a heart attack at home while using drugs,” Wright says. The woman’s boyfriend gave her chest compressions and rushed her to the emergency room, where doctors did an emergency C-section and put her on life support. But neither the mother or the baby survived.
The new study found that methamphetamine and prescription amphetamines, pose some risks to the infant, too.
It increases the risk of premature birth. It also increases the chances of having a condition called placental abruption, which cuts off oxygen supply to the fetus and causes heavy bleeding in the mom.
The new study is an important one, says Wright. “It shows with all the focus on opioids in this country, we can’t forget the other drugs — especially methamphetamine.”
National attention tended to turn away from methamphetamine in the late 2000s, because meth use was thought to be on the decline, says Dr. Mishka Terplan, an OB-GYN and an addiction specialist at Virginia Commonwealth University. But healthcare providers working in rural areas in certain regions of the country never really saw the drugs go away, he says.
“And many have been noting an increase in amphetamine and methamphetamine use in general, as well as amongst pregnant women,” adds Terplan.
Challenges of treating amphetamine use in pregnancy
“Over half of our patients that are being treated for opioid use disorders also have stimulant use disorders — meaning that they’re taking methamphetamine regularly,” says Dr. Amanda Risser, a family medicine physician at the Oregon Health & Science University in Portland, who runs a program called Project Nurture for pregnant women with substance use disorders.
Amanda Risser runs a program at Oregon Health & Science University in Portland, Ore., for pregnant women with substance abuse problems. There are currently no medications to treat methamphetamine addiction, she says, and residential treatment is often the best option for patients.
Beth Nakamura for NPR
hide caption
toggle caption
Beth Nakamura for NPR
“Since we started doing this work in 2014, we’ve always cared for women who have a tendency to use meth along with the opiates that they’ve been using,” Risser says.
Her colleagues at clinics in rural Oregon have observed the same trend there, too, she says.
Most patients want to stop using drugs when pregnant, says Risser, but quitting amphetamines is difficult.
The lows experienced with withdrawal from methamphetamine is strong, she says. The women feel depressed, unhappy and ill at ease. That’s because long term use of meth “can cause significant decreases in neurotransmitters responsible for people’s wellbeing and happiness.”
And unlike with opioids, there is no medication to help patients with methamphetamine withdrawal. So, despite their best intentions, some of Risser’s patients continue using methamphetamines even as they start their methadone treatment for opioid use.
The best treatment option for such patients is “time and support,” says Risser. Her clinic also provides behavioral therapy to help patients stay off of methamphetamine.
The project also provides residential treatment, which allows the women, many of whom are homeless, to get off the streets and be somewhere safe during the pregnancy — as well as after the birth of their child.
“Access to high quality residential treatment is very important,” says Wright.
Having a supportive OB-GYN made all the difference to Philman’s pregnancy. When she learned she was pregnant, she rushed to the Denver Recovery Group, where she was put on methadone for her opiate use. She found an OB-GYN who was supportive and understanding about her drug use, Philman says, while being candid with her about the potential effects of methamphetamine use on the baby.
“I was scared that something would be physically wrong with my son,” Philman remembers.
Philman holds her six-month old son, who was born healthy.
Theo Stroomer for NPR
hide caption
toggle caption
Theo Stroomer for NPR
That fear and worry over her son’s health, and the support from her physician, her parents and her Denver Recovery Group counselor are what helped her get through methamphetamine withdrawal, she says. What also helped, she says, was that her partner had also stopped using drugs and was well on his way to recovery.
Still, the first month of treatment during her pregnancy was difficult, she says, and she briefly returned to using meth a couple of times. But after that, she stayed clean.
The monthly ultrasounds were a big motivator, she says. “Just seeing my son grow was kind of a reality check.”
The lingering stigma of addiction
Still, many pregnant women aren’t as lucky as Philman in finding supportive doctors or nurses.
When Andrea Rano, a resident of Portland, became pregnant in 2016, she was living in a friend’s garage with her then-boyfriend. Both of them were using opioids and methamphetamine. Over the next few months, Rano worried about her pregnancy and felt guilty and ashamed about her addiction. Those feelings just fueled her drug use, she says, and kept her from seeking care.
When she did go to a hospital for a dose of methadone, the nurse practitioner she met with was disparaging and insisted on doing a urine test for drugs, Rano says, and threatened to report her to the authorities.
“I ended up leaving that hospital and feeling really uncomfortable about doctors and healthcare after that,” she says,, starting to cry. “It was really hard to be in that situation — to want to get help and feel like it was impossible.”
She felt scared, ashamed and helpless. “All I could think about was, what am I going to do? How am I going to help? Is there any help out there for me? And even if I get help, will it matter? Because what if they take my child away anyway?”
That’s the situation many pregnant women like Rano find themselves in, says Dr. Curtis Lowery, the chairman of the OB-GYN department at the University of Arkansas for the Medical Sciences, in Little Rock, Ark. Most physicians share our society’s stigma around drug abuse, Lowery says, adding that medical education doesn’t teach physicians about substance use disorders or about how to treat these conditions.
“It’s not something that most OB-GYN residencies or family medicine training expose their residents to,” says Lowery.
But that stigma can end up endangering these women’s lives and their babies.
“The worst thing we can do to pregnant women is to vilify them as a result of any kind of drug use,” Lowery says. “All you’re going to do is drive them underground.”
What these women really need is good prenatal care and help staying away from drugs, he says. “One of the things you don’t want to do with meth addiction is delay treatment,” says Lowery. “The faster you can get the patient off the drug, the better it is for the fetus and the mother.”
And that’s the little piece of good news — that with the right kind of help, women can recover from their dependence on the drug and go on to have normal pregnancies.
“We know that getting them screened, getting them into treatment early, getting them to stop using it at any point during the pregnancy — they have better outcomes and actually, normal outcomes,” says Wright. And “the longer they can remain abstinent from the drug, the more chance they have at recovery.”
Philman hasn’t used methamphetamine or opioids for almost a year. She’s going back to finish her degree — enrolled in college classes that will start in January.
Theo Stroomer for NPR
hide caption
toggle caption
Theo Stroomer for NPR
That’s been the happy experience of Philman and her son, who was born full-term and is a healthy 6-month-old now. His mom has been off the drugs for almost a year now, and is already enrolled to return to college in January.
While Rano wasn’t as fortunate initially, someone finally told her about Project Nurture in the seventh month of her pregnancy.
She was living out of a car at the time, along with her boyfriend and their dog. He was still using drugs. Rano was getting methadone for her opioid use, but was having a hard time staying off of meth.
With the support she eventually got from Risser, along with residential treatment at Project Nurture, and support from her counselor, doula and other women getting treated at the program, Rano was able to turn a corner.
She was able to stay off methamphetamine through the remainder of her pregnancy. Her son was born three weeks early — but he was and is healthy.
“It was the most amazing thing ever,” says Rano. “He was just so beautiful.I was just so happy that I was able to be there and do that — and that he was there, and he was fine.”
She credits her recovery and her son’s health to Project Nurture. “I got a huge support network [there],” she says. “I got a doctor who was absolutely amazing. I got in-patient treatment, which was having somewhere to live, somewhere to take my child home after I gave birth. It totally turned my life around.”
Number Of U.S. Kids Who Don't Have Health Insurance Is On The Rise
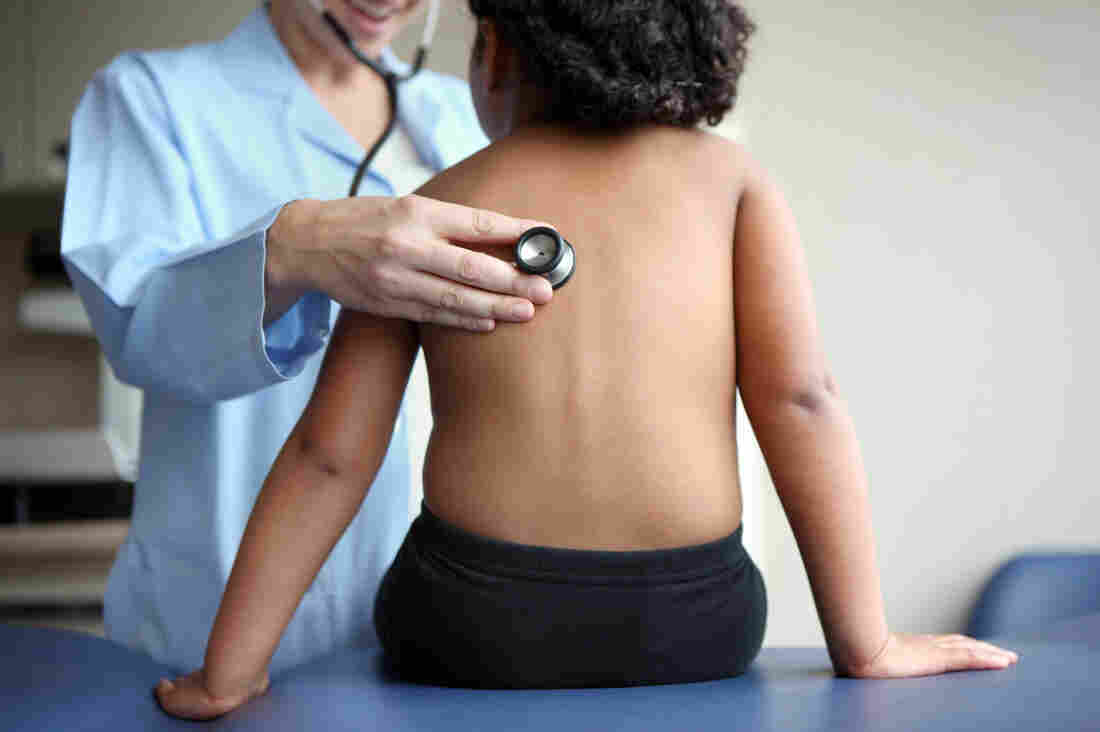
The number of children in the United States without health insurance jumped to 3.9 million in 2017 from about 3.6 million the year before, according to census data.
Katrina Wittkamp/Getty Images
hide caption
toggle caption
Katrina Wittkamp/Getty Images
After years of steady decline, the number of U.S. children without health insurance rose by 276,000 in 2017, according to a Georgetown University report released Thursday.
While not a big jump statistically — the share of uninsured kids rose to 5 percent in 2017 from 4.7 percent a year earlier — it is still striking. The uninsured rate typically remains stable or drops during times of economic growth. In September, the U.S. unemployment rate hit its lowest level since 1969.
“The nation is going backwards on insuring kids and it is likely to get worse,” says Joan Alker, co-author of the study and executive director of Georgetown’s Center for Children and Families.
Alker and other advocates for children’s health place the blame for this change on the Trump administration and the Republican-controlled Congress, saying the Republican policies and actions have cast a pall on enrollment in health plans.
The number of children in the United States without coverage rose to 3.9 million in 2017 from about 3.6 million a year earlier, according to census data analyzed by Alker’s Georgetown team.
The overall uninsured rate for people of all ages — which plummeted from 2013 to 2016 following the health law’s implementation — remained unchanged at 8.8 percent last year.
The share of children with employer-sponsored health coverage rose modestly in 2017, Alker says, but not by enough to make up for the drop in children enrolling in Medicaid or getting coverage from Obamacare insurance exchanges.
While no states made significant strides in reducing the percentage of children who are uninsured, nine states saw their numbers go the wrong way. The largest negative changes occurred in South Dakota (where the rate of uninsured kids rose from 4.7 percent to 6.2 percent), Utah (up from 6 percent to 7.3 percent) and Texas (from 9.8 percent to 10.7 percent).
More than 1 in 5 uninsured children nationwide live in Texas — about 835,000 kids — by far the highest number of any state.
Florida had 325,000 uninsured kids last year, as its uninsured rate for that age group rose 0.7 percentage points to 7.3 percent. California had 301,000 children without insurance — its number remained virtually unchanged, relative to the previous year.
Other states with significant increases were Georgia, South Carolina, Ohio, Tennessee and Massachusetts.
The uninsured rates for children increased at nearly triple the rates in states that did not expand Medicaid under the Affordable Care Act, according to the report. Studies have shown that children whose parents are insured are more likely to have health coverage.
Georgetown has been tracking these figures since 2008, when 7.6 million children — or about 10 percent of kids — lacked health coverage.
Because nearly all low-income children are eligible for Medicaid or the federal Children’s Health Insurance Program, the challenge is making sure parents are aware of the programs, Alker says, and getting the kids enrolled and keeping them signed up as long as they are eligible.
Congress let the CHIP program funding lapse for several months in 2017, putting states in a position of having to warn families that enrollment would soon be frozen. Congress restored federal funding in early in 2018.
In addition, low-income families were bombarded by news reports last year that Congress was threatening to repeal the health law that expanded coverage to millions. And, in the past two years, the Trump administration has slashed funding for Obamacare navigators who help people sign up for coverage.
Alker points to the Trump administration’s September proposal, known as the “public charge” rule as another factor that may have led to fewer children getting health insurance. The rule could make it harder for legal immigrants to get green cards if they have received certain kinds of public assistance — including Medicaid, food stamps and housing subsidies. Green cards allow these legal migrants to live and work permanently in the United States.
OLE Health, a large health provider based in Napa Valley, Calif., that serves many immigrants, says it has seen patients leave the Medicaid rolls in the past year. CEO Alicia Hardy says many have dropped coverage over fears the help could jeopardize their immigration status.
“They are afraid of being deported,” she says.
All those events may have deterred families from getting their kids covered.
“The welcome mat has been pulled back,” Alker says, “and as a result we see more uninsured children.”
She says the easiest way to change the trend would be for more states to expand Medicaid under the health law. Fourteen states have yet to do so. Though the expansion largely affects adults, as parents enroll, their children are likely to follow.
Kaiser Health News, a nonprofit news service, is an editorially independent program of the Kaiser Family Foundation, and not affiliated with Kaiser Permanente. KHN’s coverage of children’s health care issues is supported in part by a grant from the Heising-Simons Foundation.
A Trauma Surgeon Who Survived Gun Violence Is Taking On The NRA

Protesters gather beneath a banner featuring Wayne LaPierre, CEO of the National Rifle Association, during a rally outside the NRA’s annual meeting in Dallas in May. When the NRA told doctors to “stay in their lane” instead of weighing in on gun policies, Dr. Joseph Sakran sprang into action and created a Twitter account to encourage medical professionals to share their stories.
Daniel Acker/Getty Images
hide caption
toggle caption
Daniel Acker/Getty Images
For trauma surgeon Joseph Sakran, gun violence is a very personal issue. He has treated hundreds of gun wound victims, comforted anxious loved ones and told mothers and fathers that their children would not be coming home.
But Sakran’s empathy for his patients and their families extends beyond the hospital. Sakran knows the pain of gun violence because he is a survivor of it; when he was 17, he took a bullet to the throat after a high school football game.
Maybe that’s why he felt the need to do something when the NRA tweeted on Nov. 7, “Someone should tell self-important anti-gun doctors to stay in their lane,” in response to the American College of Physicians’ position paper on reducing firearm injuries and deaths.
“My first reaction was kind of incensed,” Sakran says of the NRA’s tweet. Then, he sprang into action, creating the Twitter account @ThisIsOurLane and encouraging other medical professionals to share their experiences treating victims of gun violence.
As a Trauma Surgeon and survivor of #GunViolence I cannot believe the audacity of the @NRA to make such a divisive statement.
We take care of these patients everyday. Where are you when I’m having to tell all those families their loved one has died. @DocsDemand #Docs4GunSense https://t.co/XrY1G3hIi2
— Joseph Sakran (@JosephSakran) November 7, 2018
Some of the responses have been graphic, but Sakran, who is director of emergency general surgery at Johns Hopkins Hospital in Baltimore, says that helps drive home the point: “By seeing a lot of these photos of bloodstained scrubs or by seeing an operating room floor full of blood or an empty waiting room, it’s made it real.”
When it comes to gun violence, Sakran says, “a lot of times people talk about statistics and numbers, but I think it’s so important to move beyond that, because these aren’t just numbers — these are people. These are fathers, mothers, members of the community that we interact with day in and day out.”
Interview Highlights
On being shot in the throat when he was 17
It was after a high school football game where we were just hanging out with some friends the way typical high school students do, and we were at a park at a nearby elementary school when a fight had broken out between two individuals, and a guy pulled out a gun and started firing into the crowd. At that point I got hit in the throat with a .38-caliber bullet.
And I remember that night actually pretty vividly for a variety of reasons, but one of which I was wearing white that night, and very quickly I noticed that I had blood all over my shirt and pants, and as I made my way to the curb my friends were frantically trying to figure out where I had been hit. And then they saw the spurting of blood from my windpipe. …
It might sound a little bit crazy, but it was almost as if I was watching myself and I was watching the pre-hospital workers put IVs in me, ask me different questions, almost like an out-of-body experience. … They were having to perform an emergency tracheostomy, which is providing a secure airway, because I had a ruptured windpipe.
On the stress his family went through when he was shot
I am the victim in this, but now looking back at it even as as the victim I still have a sense of guilt that [I] put [my] parents and family through something that has to be just so stressful. And I think about it often. I say I probably cut 10 years off of their life. I can’t imagine when they initially got the call that, “Your son has been injured please come to the hospital.” They didn’t tell them exactly what happened. And so you can imagine the surprise when they show up to the hospital and they say to them “Your son’s been shot.” …
I often think about this in regards to kind of what I do on a daily basis, and I always tell people the worst part of my job is going out to those waiting rooms and having to talk to families and tell them that their loved one is never coming home.
On deciding to become a trauma surgeon
There was a very profound moment that happened during my recovery period that changed how I thought about what had just happened. I was standing in the bathroom looking at the mirror and I was looking at the scars that I had. At that point I still had the tracheostomy tube, and my father happened to be walking by and kind of peeked in. I think he saw the distraught look on my face and … he said, “What happened was horrible, and either you can look at your scars and the tube that you have in your neck and feel sorry for yourself, or you can take this second opportunity and really make a difference for other people.” And it was that moment that really I think changed me for the rest of my life.
On how his experience helps him talk to families of the victims of gun violence
It’s never easy. It’s by far the worst part of my job, but it’s part of my job. I think having been a victim and now a provider I have a unique experience and I think one of the things I always try to do is to have empathy. I think that it’s very different than sympathy — really being able to kind of put yourself in their shoes and what they must be feeling and going through.
When I walk out there to talk to these families, I often will just kind of stand there for a little bit and just look through the waiting glass window, and it’s difficult. Sometimes I know that what I’m about to do is going to completely change your life. And I look at their faces and … these are all mothers, fathers, sisters, brothers that obviously care for this person who has just been injured. And so I try to be as empathetic as possible, and provide them with as comprehensive as possible a detail of what just took place.
On sharing his personal story with patients
I often do share this story with my patients and families later on if they’re lucky enough to have survived. I use that in a variety of different ways. But some patients will look at me and think, “OK, what does this person understand about gun violence?” When I tell them my story, it allows me to relate to what they’ve just been through, but also what they’ve seen from so many years in their own community.
On what he sees as the priorities for gun policy change
I think there would be really three things: The first is expanding universal background checks. The second is ensuring that we have federal funding to provide data-driven solutions. And the third is focus on safe storage and education.
Therese Madden and Seth Kelley produced and edited the audio of this interview. Bridget Bentz, Molly Seavy-Nesper and Scott Hensley adapted it for the Web.
Obamacare Sign-Ups Lag As Trump Slashes Funds For Enrollment Help

Affordable Care Act navigator Nini Hadwen (right) helped Jorge Hernandez (left) and Marta Aguirre find a plan on the health insurance exchange in Miami in 2013. Today, with fewer navigators, much of that counseling is done by phone instead of in person.
Joe Raedle/Getty Images
hide caption
toggle caption
Joe Raedle/Getty Images
Enrollment is down sharply on the federal health insurance marketplace this fall, and the consumer assistance groups that help with sign-ups think they know why.
They don’t have the staff to help as many customers as before because the Trump administration slashed funding. The federal government is spending $10 million this year on navigators who help individuals enroll in coverage. The government spent $36 million in 2017 and $63 million in 2016.
“We don’t have the people to provide the enrollment assistance nor to do the outreach and marketing to let people know what’s happening,” says Jodi Ray at the University of South Florida. She’s overseen Florida’s largest navigator program since 2014.
Ray’s program received $1.2 million in federal funding this year, down from $5 million a year ago. Florida leads the nation in enrollment in the Affordable Care Act marketplace plans.
With less money, Ray can afford to pay only 59 navigators across the state this year, down from 152 a year ago. With fewer navigators, much of the group’s counseling is done by phone instead of in person. That complicates the job, she says, because it is much easier to talk with customers in person, while looking at dozens of health plans with different costs and benefits.
Open enrollment in the Obamacare plans began Nov. 1 and will run until Dec. 15 for the 39 states covered by the federal exchange, HealthCare.gov. The other exchanges — run by states — typically extend sign-ups until the end of December or into January.
All these health plans sold under the Affordable Care Act are for people who don’t get coverage via their workplace or the government.
Nationwide, navigator groups are scrambling to make up for the loss of federal funding to ensure they can help people make sense of their health insurance options.
- In South Carolina, the Palmetto Project has transformed into the state’s first nonprofit insurance agency. Several of its former federally funded navigators are now licensed insurance agents. In their new role, they get paid a commission on their sales and don’t have to follow Trump administration rules that encourage navigators to talk to customers about short-term plans with limited benefits. The agents can also help customers enroll in Medicaid, Medicare and individual plans not sold on the ACA exchange.
- The Community Council of Greater Dallas, which was funded last year to help with enrollment in 56 counties, has raised money from private donors to continue serving the seven counties around Dallas. But it has 25 fewer navigators, so consumers seeking help must wait three days on average, compared with less than a day last year. Across Texas, 211 of 254 counties have no federally paid navigators.
- In Wisconsin, the organization Covering Wisconsin has raised millions of dollars from cities, counties and local United Way chapters, as well as the state Medicaid agency, to make up for the federal cuts. Even still, the group will be able to provide in-person assistance in only eight counties around Milwaukee and Madison. Twenty other counties are served by telephone.
- The Kansas Association for the Medically Underserved is relying completely on volunteers to help consumers with in-person and telephone assistance. In the past year, the association was able to use government funding to pay about 20 navigators.
Nationally, nearly 800 counties served by the federal marketplace will not have any federally funded navigators this fall — up from 127 counties in 2016, according to the Kaiser Family Foundation.
Federal officials say they are not providing funds for navigators in Iowa, Montana or New Hampshire because no organizations applied in those states.
Nearly 12 million people across the country — including nearly 9 million on the federal exchange — enrolled in Obamacare plans for 2018.
In the first 17 days of open enrollment, 1.9 million people chose a plan for the 2019 coverage year on HealthCare.gov, according to data released last week by the federal Centers for Medicare & Medicaid Services. That compares with nearly 2.3 million consumers who selected their coverage through the exchange during the first 18 days last year.
States with the largest enrollment drops include Pennsylvania (down 29 percent from last year), Missouri (down 27 percent) and Virginia (down 42 percent).
The annual enrollment tally is being closely followed, in part because 2019 marks the first year since the marketplace plans began in 2014 that Americans won’t be fined for failing to have health coverage.
But health insurance specialists think the lack of navigator funding could end up having a bigger impact on enrollment. Caroline Gómez-Tom, navigator program manager of Covering Wisconsin, says the end of the individual mandate penalty has been a “nonissue” among people seeking coverage.
“Some folks mention it, but at the end of the day they still walk away with health coverage,” she says. “The ability to have coverage at affordable prices outweighs the penalty being gone, because people still see health care insurance as important to have.”
Consumers generally have a greater choice of plans for 2019 as more companies enter the individual market and existing plans expand their areas of service. Plus, insurance premiums are dropping in some areas. And where they are rising, the rate of increase is among the lowest in several years.
Katrina McGivern, director of policy and public affairs for the Kansas Association for the Medically Underserved, says people in rural areas of the state will have the most difficulty getting help, as a result of funding cuts.
After five years of experience, she says, she is hopeful that people will be able to figure out how to sign up on their own.
Still, she adds, “we always see a need for people who need assistance to get through it.”
Kaiser Health News, a nonprofit news service, is an editorially independent program of the Kaiser Family Foundation, and not affiliated with Kaiser Permanente.