Trump Administration Sued Over Ending Funding Of Teen Pregnancy Programs

Several Planned Parenthood chapters and other groups involved in prevention of teen pregnancy are suing the administration for halting funding for their programs.
Daniel Acker/Bloomberg/Getty Images
hide caption
toggle caption
Daniel Acker/Bloomberg/Getty Images
It was Julie Liles’ 17-year-old daughter, Emily, who suggested that they attend a sex education program together.
Julie was eager to go. She was just 14 when she gave birth to Emily.
“So always in the back of my mind was a worry that she would get hurt,” says Julie, her voice cracking. “I worried in the back of my mind that she would find herself in the same situation.”
The mother-daughter pair spent an entire Saturday holed up at a local high school talking about relationships, love and, yes, sex. The five-hour seminar called Linking Families and Teens, or LiFT, included group discussions and role-playing to help parents and kids get comfortable talking about dating and sex.
“It was almost instantly that I felt that I could talk to my daughter in a different way, without automatically jumping to assumptions or, you know, just cutting her off and being angry or being embarrassed,” Liles says.
LiFT is the only sex education program available in her rural community of Shelton, Wash., she says.
But come July, LiFT will be gone. The Trump administration cut off the grant funding for it when the Department of Health and Human Services eliminated the Teen Pregnancy Prevention Program.
LiFT is sponsored by Planned Parenthood of the Great Northwest and the Hawaiian Islands, one of 84 organizations losing federal funding that was supposed to last until 2020.
Now the Planned Parenthood chapter, along with eight other groups, is suing HHS, saying it acted unlawfully when it canceled their five-year grants midstream and with no explanation. The organizations — which include city and county health departments, universities, hospitals and nonprofit organizations — operate across the U.S. providing sex education and health information to more than a million teens.
The Teen Pregnancy Prevention Program has been lauded by watchdogs as an example of good government at work. The program grants 80 percent of its budget to groups that implement pregnancy prevention programs that have been shown to be effective. The remaining 20 percent is dedicated to trying new strategies.
The efforts are focused on African-American and Hispanic teens, who have higher pregnancy rates, and those in low-income and rural areas.
And the organizations are required to measure whether their programs are effective in reducing pregnancy, delaying teen sex or increasing contraception use. The plans was to scale up the projects that work and eliminate the ones that don’t.
“There’s a list of proven effective programs that has been developed over time specifically through a lot of these grants,” says Carrie Flaxman, counsel for Planned Parenthood.
Programs like the ones used in Baltimore’s schools.
The Healthy Teen Network helps the city choose its sex education curriculum, using social and demographic data to make sure it meets the needs of teens, says Pat Paluzzi, president and CEO of the network.
The tiny nonprofit has been working to reduce teen pregnancy for 40 years. But now its work is threatened because more than a third of its budget comes from the HHS program.
Paluzzi says the only notice she got that the five-year grant was being eliminated after just three years came in tiny print in the middle of its renewal notice in July.
The Healthy Teen Network also is using federal grant money to create a web app to help teens make choices about sex and dating and to give them information about reproduction, birth control, safety and health care. It is in the process of launching an app designed for 15- to 17-year-olds and is designing a second one for people aged 18 to 20.
The original app – called CrushApp.org – “tells you things like how does a pregnancy occur,” Paluzzi says. “A lot of people don’t actually know where pregnancy occurs.”
A section called “Love & Sex” offers menu options such as “Is He A Keeper?” and “Put One On” about using condoms. There are cartoons and animated videos to help teens navigate relationships, dating and sex.
Work on the CrushApp will continue, Paluzzi says, but work on the second app is ending in July. The group already eliminated three jobs and is planning to move to smaller, cheaper office space.
The Healthy Teen Network and the other groups are suing in U.S. district courts in Washington, D.C., Maryland and Washington state. They accuse the Trump administration of cutting off their grants with no regard for the federal rules that dictate when a grant can be terminated.
HHS in July notified all the grantees that their money would be cut. A few were terminated immediately, and the remainder were granted one more year.
An HHS spokeswoman said the agency ended the program because it’s not effective.
“Teen birth rates have been declining since 1992 and less than 1 percent of the teen population has been served by TPP,” the spokeswoman, who declined to be named, said in an email. “Of the 37 projects funded and evaluated for a 2016 report, 73 percent had no impact or had a negative impact on teen behavior.”
Trump’s budget proposal instead has $75 million for abstinence education programs. Research has shown that “abstinence-only education rarely has a positive effect on teen sexual behavior,” according to a 2014 analysis of sex education.
Teen pregnancy rates have plummeted in the three decades from about 60 births per 1,000 girls ages 15 to 19, to just 24 in 2014. Still, the U.S. has a far higher teen pregnancy and birthrate than most developed countries.
Paluzzi says she is unhappy about the cuts to her organization. But she is more concerned about all the money already spent to develop effective sex education programs that she fears will go to waste, and the knowledge gained will be lost.
“It’s a huge waste of taxpayers’ money,” she says. “But the bigger issue is that we predict we’ll start to see teen birthrates go back up again. And that’s the real shame of it. Organizations can come and go but the young people they deserve better than that.”
Medical Records May Finally Be Coming To Your Apple Smartphone

Richard Klein switched doctors last year. The new doctor put him on a new blood pressure drug.
But it didn’t help.
The failure was entirely predictable.
Klein, an associate professor at Florida International University in Miami, realized later that he had tried the same medicine unsuccessfully a few years before, but he hadn’t remembered that fact during the appointment.
It was an understandable mistake for Klein and his doctor.
An upcoming iOS update will allow Apple users to see their health records on their cellphones.
Apple
hide caption
toggle caption
Apple
Klein’s prescription history was hidden somewhere in the hundreds of pages of medical records his new doctor had to go through.
“If I had been able to go into an app sitting in his office and look through my prescription history, I would have known that, yeah, we tried that a couple years back and it didn’t work well,” he says.
A feature like that will soon be available for some patients with iPhones.
In the upcoming release of Apple’s iOS operating system for iPhones this spring, the Health app will include health records, so patients can take information about their immunizations, medications, lab results and more with them.
The feature will first be available to patients of medical providers who partnered with Apple, including Johns Hopkins Medicine; OhioHealth; Ochsner Health System in Jefferson Parish, La.; and Cedars-Sinai in Los Angeles. It won’t cost those patients anything to use this feature, assuming they’re already iPhone users.
Apple’s announcement says more medical facilities will offer this feature in the coming months.
Some doctors hail it as a big shift away from patients having to handle a big pile of paper records every time they see a new doctor. But Google offered a similar service before and it failed. The search giant shut it down in 2012.
Can Apple succeed where Google didn’t?
Dr. Jonathan Slotkin says yes; he is a medical director handling digital patient engagement at Geisinger Health System in Pennsylvania, one of Apple’s partners. Unlike even a few years ago, a lot more people now use smartphones and the phones are more secure. There’s now also a technical standard for transferring electronic medical records.
“Even if I get care at three different places and maybe they use three different electronic systems, now in one place that I possess in an encrypted way, I have all of that information at my fingertips,” he says.
He adds this will make transferring information easier for patients who have to move, or go to a specialist.
The health records feature could also change doctors’ habits in some ways, says Dr. Isaac Kohane, chair of the department of biomedical informatics at Harvard Medical School and a professor of pediatrics.
“For some reason, and I say this as a physician, most physicians, if they don’t actually know how a test was done, somehow imagine it was done wrongly, and therefore repeat a test, not only at a cost but at some pain to the patient,” Kohane says. “If you have a reliable authoritative description of the test and its results, that uncertainty goes away and that excuse to repeat tests goes away as well.”

Checking your prescription history or past medical tests should be easier soon if you have an iPhone.
Apple
hide caption
toggle caption
Apple
Kohane called Apple’s new feature a “tectonic shift” in a commentary for member station WBUR’s CommonHealth.
But Apple will have to address one big problem that Google had with Google Health, a similar health records service: It was popular with only a niche audience — tech-savvy patients and their caregivers, and fitness enthusiasts. The product didn’t attract a wide base of users.
This time will be different, says Dr. Ida Sim, a co-director of biomedical informatics at the University of California, San Francisco Clinical and Translational Sciences Institute. Why? Because unlike with Google Health, patients no longer have to do the heavy lifting of entering or scanning their own data. Also, the 21st Century Cures Act of 2016 pushed federal agencies and providers to use electronic health records, and now there is a data standard for personal health records, which wasn’t the case in 2011.
However, she writes in an email that wider adoption will still be an issue.
“We’ll probably see huge numbers of people getting their initial Health Records populated. The issue is, then what?… The value will come from third party apps that use Health Records to provide meaningful value to patients, and until this value is demonstrated, I think Health Records uptake will be large but retention and continued engagement of patients will be challenging.”
Alan Yu reports forThe Pulse, WHYY’s health and science show.
Maryland's No-Cost Vasectomy Law May Leave Some Patients Behind

Vasectomies are more common among men over age 36 and those with higher education.
Wendy Ashton/Getty Images
hide caption
toggle caption
Wendy Ashton/Getty Images
It’s a well-intentioned effort to provide men with some of the same financial protection from birth control costs that women get. But a new Maryland law may jeopardize the ability of thousands of consumers — both men and women — to use health savings accounts.
The Maryland law, which took effect Jan. 1, mandates that insurers cover vasectomies without requiring patients to pay anything out-of-pocket — just as they must do for more than a dozen birth control methods for women.
But the measure may run afoul of Internal Revenue Service rules that do not include vasectomies among the approved preventive services for high-deductible health plans. People with health savings accounts (HSAs) tied to those plans could no longer contribute to them because those plans may no longer meet IRS standards.
Under the Maryland Contraceptive Equity Act, insurers generally can’t charge patients a copay or require any other cost sharing for prescription contraceptive drugs or devices approved by the Food and Drug Administration. The 2016 state law is similar to what’s required under the federal Affordable Care Act, with a twist: It adds male sterilization — vasectomies — to the list of services that are free for patients.
“While the ACA made important strides … it completely left men out of the equation,” says Karen Nelson, president and CEO of Planned Parenthood of Maryland, whose organization supports the state’s law.
Before the law took effect, a vasectomy at Planned Parenthood’s Baltimore office would cost between $225 and $1,100, depending on someone’s ability to pay, says Nelson. Now the procedure will generally cost nothing for men in insured plans in Maryland.
The state law doesn’t apply to companies that are “self-funded,” meaning they pay their employees’ health care claims directly rather than buying state-regulated insurance policies.
But there’s a hitch in the law for certain people. Under IRS rules, consumers making tax-free contributions to HSAs that are linked to high-deductible health plans have to pay for all their medical care until they reach their deductible of at least $1,350 for individuals and $2,700 for families in 2018. The only exception is for preventive services.The problem with the Maryland law is that vasectomies aren’t on the IRS list of approved preventive services.
The IRS hasn’t responded to a request for clarification by Maryland Insurance Commissioner Al Redmer Jr. Maryland lawmakers have introduced legislation that would exempt these high-deductible plans from the state mandate to cover vasectomies before the deductible is met. If passed, that could preserve the tax advantages of the HSAs linked to those plans.
Maryland is joining a few other states, including Illinois, Vermont and, starting next year, Oregon, that have expanded contraceptive coverage without cost sharing to include male sterilization.
Vermont’s law includes language to exempt high-deductible plans with health savings accounts. In Illinois and Oregon, the HSA issue hasn’t appeared to generate much attention to date, legislative analysts say.
Some advocates for extending no-cost coverage to vasectomies noted that the IRS’ list of approved preventive services specifically says that it isn’t exhaustive.
But until the issue is clarified, “the safest thing to do is not make a contribution to your HSA,” says Roy Ramthun, a Maryland resident and president of HSA Consulting Services. Ramthun helped implement health savings accounts while working for the Treasury Department during the George W. Bush administration. He stressed that the uncertainty applies only to HSA contributions made after the law became effective in 2018, not to earlier contributions. The issue doesn’t affect people’s medical coverage.
Despite the uncertainty around HSAs, Maryland’s law requiring coverage of vasectomies without cost sharing addresses a gap in men’s preventive coverage.
Still, only 7 percent of men ages 18 to 45 have had a vasectomy, according to a 2013 study by researchers at Northwestern University. The prevalence increased to 16 percent among men ages 36 to 45. Men with higher incomes, higher education and a regular source of health care were more likely to have had the procedure, the study found.
The Maryland law doesn’t apply to the method of birth control that many men use: condoms. A bill introduced this month by state Sen. John Astle, a Democrat, would expand the law to include condom coverage.
Kaiser Health News is an editorially independent news service that is part of the nonpartisan Henry J. Kaiser Family Foundation. Michelle Andrews is on Twitter @mandrews110.
Doctors In Maine Say Halt In OxyContin Marketing Comes '20 Years Late'

Bottles of Purdue Pharma L.P. OxyContin medication sit on a pharmacy shelf in Provo, Utah, in 2016.
George Frey/Bloomberg via Getty Images
hide caption
toggle caption
George Frey/Bloomberg via Getty Images
The maker of OxyContin, one of the most prescribed and aggressively marketed opioid painkillers, will no longer tout the drug or any other opioids to doctors.
The announcement, made Saturday, came as drugmaker Purdue Pharma faces lawsuits for deceptive marketing brought by cities and counties across the U.S., including several in Maine. The company said it’s cutting its U.S. sales force by more than half.
Just how important are these steps against the backdrop of a raging opioid epidemic that took the lives of more than 300 Maine residents in 2016, and accounted for more than 42,000 deaths nationwide?
“They’re 20 years late to the game,” says Dr. Noah Nesin, a family physician and vice president of medical affairs at Penobscot Community Health Care.
Nesin says even after Purdue Pharma paid $600 million in fines about a decade ago for misleading doctors and regulators about the risks opioids posed for addiction and abuse, it continued marketing them.
“I think it’s similar to the tobacco industry learning they could sell tobacco without spending a lot of money on advertising. My guess is this decision is in their self-interest,” he says.
A nationwide lawsuit against Purdue Pharma for deceptive marketing continues to grow. Seven cities in Maine have joined, including Portland, Lewiston and Bangor, along with five counties, to recoup some of the costs of addressing the addiction crisis.
A spokesman for Purdue Pharma said in an email that the decision to stop marketing to prescribers is voluntary and independent of any litigation.
Nesin says that at the very least, the company’s decision to refrain from promoting opioids to doctors reinforces the need for caution when prescribing the drugs.
Maine Medical Association President Dr. Robert Schlager agrees that Purdue Phama’s move is a good, if small, step to fight the opioid epidemic. “I wouldn’t expect it to have a very large role in limiting opioids further,” he says. “Because most of us, as prescribers, do limit our information exchange with the drug representatives who have been marketing opioids.”
Since 2016, doctors in Maine have also adhered to prescribing limits enacted by the Legislature. As of December 2017, legislatures in 17 states had enacted prescribing limits and nine others had authorized other state entities to enact them.
Schlager says Purdue Pharma should go further and suspend opioid marketing worldwide. “It seems a little bit not honest to just limit it here in the United States,” he says.
In an email, Purdue Pharma’s spokesman says that the company operates only in the United States, and that an associated company, Mundipharma, has not marketed opioids in Europe since 2013.
A Los Angeles Timesinvestigation in 2016 found that the family that owns Purdue Pharma has a network of international companies that employ the same kinds of marketing practices that made OxyContin a blockbuster seller in the U.S.
This story is part of a reporting partnership with NPR, Maine Public Radio and Kaiser Health News.
Trump's Budget Proposal Swings At Drug Prices But May Land Only A Glancing Blow

President Trump’s budget request includes provisions that could affect drug prices.
Andrew Harrer/Bloomberg via Getty Images
hide caption
toggle caption
Andrew Harrer/Bloomberg via Getty Images
President Trump’s proposed budget flirts with combating high prescription drug prices, but industry watchers say the tweaks to Medicare and Medicaid do little more than dance around the edges of the problem.
The White House’s proposal, which comes after Congress passed a two-year spending deal Friday, though, sets the tone for the administration’s focus on prescription drugs.
“Drug costs are a populist issue for the president,” and he’s made it clear to his staff that progress needs to be made this year, said Dan Mendelson, president of Avalere Health, a health care consulting firm.
The proposal would cut billions of dollars in drug spending in the federal Medicare program, which provides health care for about 60 million people age 65 and older or younger patients with disabilities. The budget would also alter drug spending in Medicaid’s safety-net program for nearly 70 million Americans. The sheer size of the federal government’s Medicare and Medicaid programs means any drug pricing tweaks that do get made are meaningful — just not necessarily groundbreaking.
“The main question is, how far are they actually going to go in dealing with the underlying problem?” said Paul Van de Water, who spent nearly two decades in the Congressional Budget Office and is now a senior fellow at the Center on Budget and Policy Priorities. Most of the proposals for Medicare, for example, move money around rather than force a drop in prices, Van de Water said.
Alex Azar, the newly appointed secretary of Health and Human Services, said the proposed budget supports the work his agency is already doing to reduce the high cost of prescriptions, “especially for America’s seniors.”
Just last month, the former Eli Lilly executive told Congress during his confirmation hearings that “all drug prices are too high in this country.”
Highlights from the proposals include:
- Passing on the discounts and rebates negotiated by pharmacy benefit managers, the financial middlemen between insurers and drugmakers, to seniors who buy drugs through Medicare Part D. The seniors would pay less out-of-pocket when buying their drugs but the proposal could potentially raise premiums because insurers wouldn’t be getting the discounts.
- Ensuring that low-income seniors in Medicare don’t pay for generics and capping out-of-pocket costs for beneficiaries who pass through the so-called doughnut hole, or coverage gap, and hit the catastrophic stage. Beneficiaries typically pay a 5 percent coinsurance in the catastrophic phase, but under the plan it would be decreased to zero.
- Moving some of the drugs paid for under Medicare Part B, which covers drugs administered in the doctor’s office such as chemotherapy and rheumatoid arthritis infusions, into the Part D part of the program to foster price negotiations. While the government pays sticker price for drugs under the Part B program, the Part D program allows insurers and pharmacy benefit managers to negotiate formularies.
Creating a five-state pilot project to allow state Medicaid programs to negotiate prices with manufacturers and create their own drug formularies, or preferred lists of medicines.
Trump entered office with blustering promises to bring drug prices “way down.” But critics have charged that the White Househas failed to engage Congress on cost-cutting ideas, and that a leaked draft of an executive order last summer read like a wish list for the industry.
With the proposed budget, the administration is trying to recast that narrative at a time when Republicans in Congress may be willing to compromise.
“Americans want Washington to lower prescription drug prices, and our paper provides policy options that would make drugs more accessible to Americans, today and in the future,” wrote D.J. Nordquist, chief of staff for the president’s Council of Economic Advisers, in an email late Friday after the council released a 28-page report on tackling drug prices.
The CEA paper and the president’s budget come on the heels of Congress passing a spending pact Friday that includes a big benefit to Medicare enrollees at the expense of the pharmaceutical industry. The budget proposes closing the doughnut hole in 2019, a year earlier than expected.
Republicans “just showed a propensity to sort of take on the industry,” said Jayson Slotnik, a policy consultant and partner at Health Policy Strategies. And there is political upside for doing more since Republicans are concerned about this year’s November midterm elections approaching, Slotnik said: “They can run and [say] it’s something they have accomplished.”
Yet James Love, director of the nonprofit Knowledge Ecology International, said Trump’s proposals are not “insightful or original” and, referring to the council’s report, said it “could have been written by PhRMA,” the powerful trade group for pharmaceutical manufacturers.
PhRMA released a statement late Monday applauding the provision to pass on rebates to Medicare beneficiaries but also raising concerns about other elements of the budget proposal, saying they would “limit access to innovative medicines.”
Experts from the academic and think-tank world said the district has seen several of these policies before. For example, the rebate and discount pass-through proposal has been a topic of discussion within the Centers for Medicare & Medicaid Services for more than a year and is already in the rulemaking process.
Another proposal that lowers reimbursement for Medicare Part B drugs that are new to the program is reminiscent of an Obama-era pilot that never got off the ground.
Tara O’Neill Hayes, who focuses on health policy at the conservative American Action Forum, said several Medicare proposals were also similar to those found in a June 2016 report by the Medicare Payment Advisory Commission. If all the Medicare proposals took effect — including one that calls for more flexibility in drug formularies — O’Neill Hayes said overall premiums could go up slightly for all Part D beneficiaries, but that would be offset by lowering out-of-pocket payments for the beneficiaries with the highest drug costs.
“You’re going to have winners and losers,” she said. “The real winners here are going to be the incredibly high-cost patients.”
Trump’s budget requires hospitals to provide a minimum level of charity care to get an additional payment adjustment under the 340B program, which requires pharmaceutical manufacturers to provide drugs at steep discounts to hospitals and clinics with a high proportion of low-income patients.
The administration lowered reimbursement amounts for hospitals earlier this year, and Mendelson at Avalere said he expects more changes.
In reviewing Trump’s budget and the council report, Allan Coukell, senior director of health programs at the Pew Charitable Trusts, said several of the proposals “have the potential to reduce out-of-pocket costs, several have the potential to increase competition within the programs and/or move people toward lower cost drugs. None of it changes the overall trajectory” of rising sticker prices.
Kaiser Health News is a nonprofit news service covering health issues. It is an editorially independent program of the Kaiser Family Foundation that is not affiliated with Kaiser Permanente. KHN’s coverage of prescription drug development, costs and pricing is supported by the Laura and John Arnold Foundation.
Cost Of U.S. Opioid Epidemic Since 2001 Is $1 Trillion And Climbing
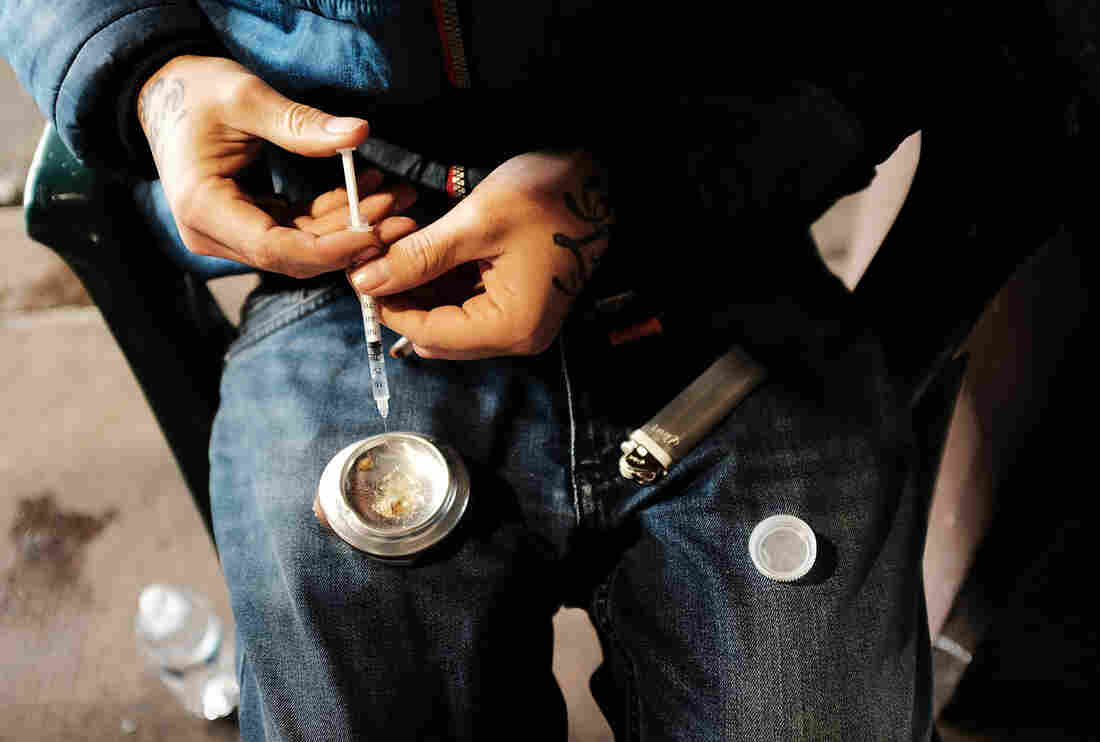
A young man uses heroin under a bridge in the Kensington section of Philadelphia, a neighborhood that has become a hub for heroin use. The economic costs of the epidemic are mounting, researchers say, as the U.S. loses more and more workers in their prime.
Spencer Platt/Getty Images
hide caption
toggle caption
Spencer Platt/Getty Images
The opioid epidemic has cost the U.S. more than a trillion dollars since 2001, according to a new study, and may exceed another $500 billion over the next three years.
The report by Altarum, a nonprofit group that studies the health economy, examined CDC mortality data through June of last year. The greatest financial cost of the opioid epidemic, according to the report, is in lost earnings and productivity losses to employers. Early deaths and substance abuse disorders also take a toll on local, state and federal government through lost tax revenue.
These costs are rising. One reason for the increase, says Corey Rhyan, a senior research analyst with Altarum’s Center for Value and Health Care, is that more young people are being affected as the epidemic moves from prescription opioids to illicit drugs like heroin and fentanyl.
“The average age at which opioid deaths are occurring — you’re looking at something in the late 30s or early 40s,” Rhyan says. “As a result, you’re looking at people that are in the prime of the productive years of their lives.”
Health care expenses linked to the crisis — more than $215 billion since 2001 — have been significant, too, the report suggests. Those expenses stem largely from emergency room visits, ambulance costs and the use of naloxone, a drug used to stop and reverse the effects of an opioid overdose.
The Altarum researchers say the growth in costs between 2011 and 2016 was double the rate of the previous five years and is projected to keep rising steeply unless there is a comprehensive and sustained national response.
Congress is considering spending $6 billion over the next two years to address the national crisis. In his budget, President Trump is proposing $13 billion in new spending on opioids, but that is partially offset by cuts in other health care programs like Medicaid.
Drugmakers Spent Millions Promoting Opioids To Patient Groups, Senate Report Says

OxyContin pills arranged for a photo at a pharmacy in Montpelier, Vt. in a photo taken in 2013.
Toby Talbot/AP
hide caption
toggle caption
Toby Talbot/AP
Drug-makers gave millions of dollars to pain-treatment advocacy groups over a five-year period beginning in 2012, in effect promoting opioids to individuals most vulnerable to addiction, a new report released Monday by a U.S. Senator says.
The 23-page report, put out by Missouri Democratic Sen. Claire McCaskill, sheds light on the pharmaceutical industry’s efforts to shape public opinion and to fuel demand for such lucrative and potentially addictive drugs as OxyContin, Fentanyl and Vicodin that have played a key role in the addiction crisis that has swept the U.S. in recent years, claiming hundreds of thousands of lives.
Fueling an Epidemic: Exposing the Financial Ties Between Opioid Manufacturers and Third Party Advocacy Groups describes how the arrangement between pharmaceutical makers and advocacy groups “may have played a significant role in creating the necessary conditions for the U.S. opioid epidemic.”
“The pharmaceutical industry spent a generation downplaying the risks of opioid addiction and trying to expand their customer base for these incredibly dangerous medications and this report makes clear they made investments in third-party organizations that could further those goals,” McCaskill said. “These financial relationships were insidious, lacked transparency, and are one of many factors that have resulted in arguably the most deadly drug epidemic in American history.”
Sen. Claire McCaskill, D-Mo., announces her findings from an investigation into opioid prescriptions, in September, on Capitol Hill. A full report was released Monday.
Jacquelyn Martin/AP
hide caption
toggle caption
Jacquelyn Martin/AP
The report follows a similar investigation in 2012 carried out by Sen. Max Baucus, D-Mont., and Chuck Grassley, R-Iowa, that looked into financial ties between drug makers and medical providers who helped establish guidelines for prescribing opioids. That investigation was ultimately shelved.
“It looks pretty damning when these groups were pushing the message about how wonderful opioids are and they were being heavily funded, in the millions of dollars, by the manufacturers of those drugs,” Lewis Nelson, a Rutgers University doctor and opioid expert says, according to The Center for Public Integrity.
The report says that nearly all health advocacy groups accept funding from drug manufacturers, adding that “These financial relationships—and the lack of transparency surrounding them—have raised concerns regarding the information and initiatives patient advocacy organizations promote.”
The report cites the Journal of the American Medical Association as saying that 8 percent of such patient groups responding to one study “reported [that] pressure to conform their organizations’ positions to the interests of industry funders is of concern.”
A single company, Purdue Pharma, the maker of OxyContin, funneled $4.7 million to advocacy groups over the five-year period, according to the report.
Also mentioned are Depomed, which markets the narcotic Nucynta, the brand name of the opioid pain reliever tapentadol and three makers of fentanyl, a powerful and potentially addictive pain reliever: Janssen Pharmaceuticals, Mylan and Insys Therapeutics, whose CEO was charged in October for using bribes and kickbacks to promote unacceptable uses of the company’s flagship fentanyl spray, Subsys.
The companies gave more than $10 million between 2012 and 2017 to 14 advocacy groups and affiliated doctors, the report says.
In that period, Insys gave $2.5 million to the U.S. Pain Foundation for one of the group’s patient assistance programs, the report says.
The U.S. Pain Foundation said “any funding we receive has never nor will it ever influence what we will do to help people with chronic pain,” according to a statement published in The St. Louis Post Dispatch.
The Associated Press writes: “The findings [in the report] could bolster hundreds of lawsuits that are aimed at holding opioid drugmakers responsible for helping fuel an epidemic blamed for the deaths of more than 340,000 Americans since 2000.”
OxyContin Manufacturer Says It Will Stop Promoting Opioid Painkiller To Doctors
NPR’s Ari Shapiro talks with journalist Sam Quinones about Purdue Pharma’s announcement that it would stop promoting its blockbuster opioid painkiller OxyContin to doctors. Purdue’s move comes as it faces dozens of lawsuits.
Can A Patient Gown Makeover Move Hospitals To Embrace Change?

The new hospital garment ties in the front, like a robe, allowing the patient more modesty than the standard gown.
Sophie Sahara Barkham/courtesy Care+Wear
hide caption
toggle caption
Sophie Sahara Barkham/courtesy Care+Wear
A medical company is trying to make hospital gowns less terrible — maybe even good. The company is called Care+Wear and it’s currently testing out the new gowns at MedStar Montgomery in Olney, Md.
You know the old gown, sometimes called a “johnny“: It’s got the flimsy ties and the exposed back.
The new gown from Care+Wear ties at the front like a robe. It’s got color coded ties and a pocket for your phone. Maybe most importantly, it covers the butt without sacrificing bedpan access for the bedridden.
A new hospital gown isn’t a completely original thought. Back in 1999, a hospital in Hackensack, N.J., asked designer Nicole Miller to make gowns, robes, and pajama bottoms. In 2010 The Cleveland Clinic recruited Diane Von Furstenberg to help design a new gown modeled after her famous wrap around dresses. In 2014, the Henry Ford Health System in Detroit teamed up with Carhartt to make a robe they dubbed the Model G. While these designs may have been successful on the small scale, none of them have usurped the johnny gown as the industry standard, say industry experts.
Why not? “Hospitals are not designed for patients,” says Dr. Bridget Duffy, the chief medical officer of Vocera, a hospital communications company. More importantly for this story, she was the chief experience officer at the Cleveland Clinic — the one with the Diane Von Furstenburg gown that they still use today — and she helped consult on the new Care+Wear gown. She says a big reason hospitals don’t move toward a more patient-friendly gown is due to your usual bureaucratic inertia, as well as a habit of focusing more on health care provider needs than patients’ needs.
“In the past we’ve never had patients in the room at the very beginning of the design process,” she says.

Instead of flimsy ties, the back of the new gown has a flap to cover the patient’s behind.
Sophie Sahara Barkham/courtesy Care+Wear
hide caption
toggle caption
Sophie Sahara Barkham/courtesy Care+Wear
Dr. Fredrick Finelli, surgeon and vice president at MedStar Montgomery, sums up the gown design conflict: “For me as a doctor, it would be best to have the patient naked,” he says. “Then I wouldn’t have to deal with any gowns or cloth in my way. But for the patient, they basically want the opposite. They’d like to be covered up.”
Care+Wear teamed up with a class at the Parsons School of Design to iron out the kinks of making a new robe that works for both patient and provider. Irene Lu was a student in the class who says they took each step of their design to both clinicians and patients.
“Working with these patients with different opinions on the gowns really helped inform our design,” she says. They took notes on how people felt about the neckline, the buttons, the ties, and how it fit on people of different sizes and mobility.
Jimena Ryan was a patient at MedStar Montgomery who was wearing the new gown when I spoke to her. She was into it. The gown works more or less like a robe, so it felt familiar to her.
“I have many dresses for work that come together the same way, so it’s intuitive to put it together,” she says. “And the fact that it’s not open in the back is a big relief, especially when you’re up and around,” she adds.
Part of Ryan’s recovery was walking around the halls of the hospital. With the old gown, “you’re always wondering what is open and what is flapping, what view am I giving,” she says.
Professor Traci Lamar is less optimistic about any robe overtaking the johnny gown. She teaches at North Carolina State University in the college of textiles, and had a hand in a hospital gown re-design herself back in 2009.
“There are number of pressures in the hospital environment that influence what they purchase and when they purchase. Cost management, inventory management, storage space, all of those kinds of things come into play as factors when they start looking at changing a garment that’s widely used,” she says.
To her, the cost-benefit analysis isn’t going to tip in favor of more hospitals changing gowns until the gowns have something more to offer than coverage.
“There’s more value coming with the apparel item if it also becomes something that replaces or enhances other equipment that’s used in the hospital environment,” she says. Like a gown that can also keep an eye on your blood pressure, or measure your heart rate.
Who knows when textiles can be smart enough to pull that off, so we might be stuck with the old johnny gown for a while.
What The Budget Deal Means For Medicare Drug Prices
The new budget will likely lower the cost of expensive prescription drugs for Medicare patients. Elisabeth Rosenthal of Kaiser Health News talks with NPR’s Scott Simon.
SCOTT SIMON, HOST:
The new budget passed late this week includes changes for Medicare patients. It will require drug companies to give deeper discounts to Medicare on expensive prescriptions. That should reduce the cost of drugs for patients. The skyrocketing cost of prescription drugs is something followed closely by Elisabeth Rosenthal, a veteran healthcare reporter and editor-in-chief of Kaiser Health News, who joins us from her offices. Thanks so much for being with us.
ELISABETH ROSENTHAL: Thanks for having me.
SIMON: Will this and other features you see in the budget help reduce the cost of prescription drugs?
ROSENTHAL: Well, to a small number of people, it will. I mean, this really targets the Medicare-age population and Medicare plans. And for people who have very high drug costs within Medicare, it will definitely help them. But it, of course, doesn’t solve the much larger problem of the very high prescription drug prices that everyone pays in this country. And P.S., what we’re talking about for Medicare patients, even, are discounts on these very high initial prices. So, you know, a discount of a really high price still isn’t a very good deal.
SIMON: Why do we have a problem with this in the United States?
ROSENTHAL: Well, we’re the only country that doesn’t in some way directly negotiate prescription drug prices with manufacturers – the only developed country, that is. I mean, most other countries in some form either evaluate the cost-benefit ratio of a new drug and decide what they’re willing to pay or, you know, very aggressively negotiate with drug manufacturers, particularly for older drugs, as they age.
SIMON: Insulin in one form or another has been saving lives for – what? – 80 years.
ROSENTHAL: Yeah.
SIMON: Why has the price gone up in recent years?
ROSENTHAL: Prices will rise to whatever the market will bear, right? We see that uniquely in the U.S. One vial of insulin in the U.S. costs seven times what it does in Germany. So there’s a huge disparity there. Some of the reasons have to do with reformulations of insulin that are, in fact, better than some of the older ones. Although, when I’m talking about that 1 in 7 price comparison, that’s the same exact insulin.
In the U.S., what’s happened – and this is something that I know the Trump administration is looking at and many experts in the field have decried – the slow arrival of biosimilars or generic insulins onto the market, which are on the market in other countries. The problem in this country is the lowering of prices of insulin. And insulin patents have been held up in the courts for years now in suits and countersuits between the three big insulin drug makers, including by Eli Lilly, which is the former employer of our new HHS Secretary.
SIMON: That’s Alex Azar – has been appointed Secretary of Health and Human Services.
ROSENTHAL: Yes.
SIMON: Is he the kind of choice that gives you optimism that prescription drug prices will come down?
ROSENTHAL: Well, there’s a certain argument to be made that Alex Azar of all people on Earth understands how the games are played and how these suits and countersuits about making generics or making biosimilars have held up the arrival on the U.S. market and have raised prices for everyone. On the other hand, there’s ongoing concern about the revolving door between government and pharmaceutical companies such that you wonder, is their loyalty to the American people, or is their loyalty to the pharmaceutical world from which they came?
SIMON: I don’t think I can think of any politician who says, and if you elect me, I promise prescription drugs will cost more.
ROSENTHAL: (Laughter).
SIMON: I mean, on the contrary, every politician says, elect me, and I’ll do something to bring down the cost of prescription drugs. Why doesn’t that get done?
ROSENTHAL: Yeah. Everyone agrees that our prescription drug costs are too high – both right and left – you know, Democrat, Republican. It’s one of the few points of information, points of fact that everyone agrees on. The problem is everyone disagrees on how best to tackle that. And there are a lot of forces that are resisting any change at all.
The bipartisan solution which Senator Klobuchar and Senator John McCain have proposed is allowing prescription drug imports from other countries, so we allow for a global competition in the sense of, you know, if everyone else is getting a better deal than us, why can’t we buy our prescription drugs from there the same way we buy our, you know, refrigerators and cars?
SIMON: Elisabeth Rosenthal, editor-in-chief of Kaiser Health News and author of “An American Sickness: How Health Care Became Big Business And How You Can Take It Back.” Thanks so much for being with us.
ROSENTHAL: Thanks for having me.
(SOUNDBITE OF THE JAZZ MANDOLIN PROJECT’S “SPIDERS”)
Copyright © 2018 NPR. All rights reserved. Visit our website terms of use and permissions pages at www.npr.org for further information.
NPR transcripts are created on a rush deadline by Verb8tm, Inc., an NPR contractor, and produced using a proprietary transcription process developed with NPR. This text may not be in its final form and may be updated or revised in the future. Accuracy and availability may vary. The authoritative record of NPR’s programming is the audio record.

